Artículos
Application of Transitional Care Model in Patients with Chronic Heart Disease: A Case-Controlled Intervention Study
Aplicación del modelo de atención de transición en pacientes con enfermedad cardíaca crónica: un estudio de intervención controlado por casos
Application of Transitional Care Model in Patients with Chronic Heart Disease: A Case-Controlled Intervention Study
Revista Latinoamericana de Hipertensión, vol. 13, no. 3, pp. 285-290, 2018
Sociedad Latinoamericana de Hipertensión

This work is licensed under Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International.
Abstract:
: People with chronic heart disease are surrounded by many problems due to the nature of their illness. These include physical problems and disabilities in the daily activities of life, emotional problems as well as social and economic problems that are all the consequences of heart disease. The design and implementation of new care models as well as new managerial approaches are necessary to improve care and patients' access to better outcomes and, in general, to improve the quality of life of this group of patients. People with chronic heart disease are surrounded by many problems due to the nature of their illness. These include physical problems and disabilities in the daily activities of life, emotional problems as well as social and economic problems that are all the consequences of heart disease. The design and implementation of new care models as well as new managerial approaches are necessary to improve care and patients' access to better outcomes and, in general, to improve the quality of life of this group of patients. The present study aims to investigate the effect of transitional care on quality of life in patients with chronic heart failure in physical, emotional-spiritual, and socioeconomic dimensions. The present study is an experimental study on patients with chronic heart failure who need nursing care during hospitalization and after discharge from hospital. The data collection tool is Minnesota Living with Heart Failure Questionnaire (MLHFQ). The sampling method is random. After the referral to the emergency department, the liaison nurses randomly assigned samples to intervention and control groups. The intervention group was followed up and trained by the liaison nurse for 6 months. The control group members were hospitalized as usual and went through their treatment process. A total of 168 samples were evaluated in both intervention and control groups. The results of the study show that the quality of life of patients in the intervention group is significantly higher than the control group in different physical, emotional-spiritual, and socioeconomic dimensions (P <.05). In the transitional care model, nursing care focuses on improving the quality of care in various physical, emotional-spiritual, and socioeconomic dimensions, which leads to increased patient and family outcomes, reduced hospitalization costs for patients with chronic heart disease, and increased role and effect of home care provided.
Keywords: Transitional Care, Chronic Heart Disease, Hospitalization, Liaison Nurse, Nursing.
Resumen:
Las personas con cardiopatía crónica están rodeadas de muchos problemas debido a la naturaleza de su enfermedad. Estos incluyen problemas físicos y discapacidades en las actividades cotidianas de la vida, problemas emocionales, así como problemas sociales y económicos que son todas las consecuencias de la enfermedad cardíaca. El diseño y la implementación de nuevos modelos de atención, así como nuevos enfoques gerenciales son necesarios para mejorar la atención y el acceso de los pacientes a mejores resultados y, en general, para mejorar la calidad de vida de este grupo de pacientes. Las personas con cardiopatía crónica están rodeadas de muchos problemas debido a la naturaleza de su enfermedad. Estos incluyen problemas físicos y discapacidades en las actividades cotidianas de la vida, problemas emocionales, así como problemas sociales y económicos que son todas las consecuencias de la enfermedad cardíaca. El diseño y la implementación de nuevos modelos de atención, así como nuevos enfoques gerenciales son necesarios para mejorar la atención y el acceso de los pacientes a mejores resultados y, en general, para mejorar la calidad de vida de este grupo de pacientes. El presente estudio tiene como objetivo investigar el efecto de la atención de transición en la calidad de vida en pacientes con insuficiencia cardíaca crónica en dimensiones físicas, emocionales, espirituales y socioeconómicas. El presente estudio es un estudio experimental en pacientes con insuficiencia cardíaca crónica que necesitan cuidados de enfermería durante la hospitalización y después del alta hospitalaria. La herramienta de recopilación de datos es Minnesota Living with Heart Failure Questionnaire (MLHFQ). El método de muestreo es aleatorio. Después de la derivación al departamento de emergencia, las enfermeras de enlace asignaron aleatoriamente muestras a los grupos de intervención y control. El grupo de intervención fue seguido y entrenado por la enfermera de enlace durante 6 meses. Los miembros del grupo de control fueron hospitalizados como de costumbre y pasaron por su proceso de tratamiento. Se evaluaron un total de 168 muestras en los grupos de intervención y control. Los resultados del estudio muestran que la calidad de vida de los pacientes en el grupo de intervención es significativamente más alta que el grupo de control en diferentes dimensiones físicas, emocionales, espirituales y socioeconómicas (p<0,05). En el modelo de atención transicional, la atención de enfermería se enfoca en mejorar la calidad de la atención en diversas dimensiones físicas, emocionales, espirituales y socioeconómicas, lo que lleva a mayores resultados para el paciente y la familia, costos de hospitalización reducidos para pacientes con cardiopatía crónica y un mayor papel y efecto de la atención domiciliaria proporcionada.
Palabras clave: Cuidado de transición, enfermedad cardíaca crónica, hospitalización, enfermera de enlace, enfermería.
Introduction
Patients with chronic heart disease face many barriers to managing their health needs. On the other hand, the number of visits of this group of patients to hospitals is higher than other people2. The results of numerous studies show that poor management of the health needs of patients with chronic disease has an important role in worsening the physical and economic status of this group of patients3. In general, six categories of problems will lead to negative outcomes in patients with chronic heart disease during hospitalization and post-discharge at home, including: lack of involvement of the patient in self-care, lack of communication or inadequate communication, lack of collaboration between the treatment team, the limited follow-up and monitoring of the patient, lack of continued care, and a deep gap in the provision of services to the patient, especially after discharge from the hospital4. The frequent hospitalization of this group of patients in the hospital is unavoidable. In addition, the cost of care for them in the hospital will increase with their age. Most of these costs are due to frequent hospitalization that is avoidable. Experience has shown that refining processes and improving their management can have an effective role in the outcome of these patients5. For example, a study by Naylor et al. (2006) was conducted on elderly patients with heart failure, who were admitted to the hospital and discharged after receiving care and treatment. In this study, the time of first referral and re-hospitalization of patients among transitionally-treated patients significantly decreased (p = .026) compared with the control group. In this method, in comparison with the standard care method, the number of re-admission of patients in the hospital after one year after discharge and control of patients had decreased (p = .047). In this study, all patients who received transitional care also had higher quality of life than patients who had experienced other care method6,9. Another study conducted by Hirschman et al. (2015) showed that the combination of patient-centered care model with the transitional care model in chronic patients increased their re-hospitalization time after discharge, compared with patients who had only received patient-centered care model7,10. According to the results of the studies, the treatment of chronic heart disease requires new approaches to management that pursue three important purposes, including enhanced patient experiences, improved health and reduced costs7,8. Control-centered transitional care that provides the patient's care needs during admission to the hospital is considered as an accepted approach among chronic heart disease patients. The transitional care model is designed to improve the quality of life and prevent the complications of diseases in the elderly and chronic patients9. While providing a comprehensive assessment of the patient's health status at the time of hospitalization, this care model is planned to be continued for home care and social support with the help of a liaison nurse and careful planning for caring for people with chronic illness. In this unique care plan, designed and implemented in partnership with the liaison nurse and the patient, care will be provided in accordance with the new evidence-based guidelines from the time the patient is hospitalized until the discharge along with the patient's care plan. Therefore, the present study was designed to investigate the effect of transitional care on the quality of life in patients with chronic heart failure in terms of physical, emotional-spiritual, and socioeconomic dimensions.
Method
The present study is an experimental (case-controlled intervention) study on patients with chronic heart failure referring to the emergency department of hospitals selected by Shahid Beheshti University of Medical Sciences, who need nursing care during hospitalization and after discharge from hospital. In this study, three specific features of experimental studies including intervention, random allocation of samples and the existence of control or comparison group are considered. The data collection tool is Minnesota Living with Heart Failure Questionnaire (MLHFQ). Sampling method is random.
Liaison nurses’ inclusion criteria:
Before starting the sampling, the researcher attempted to identify the liaison nurses. In this study, in each selected hospital, a liaison nurse with the following conditions was considered for sampling and providing transitional care.
- Experience of working with chronic heart disease patients
- Full awareness of the hospital environment and treatment process
- Morally approved by the hospital
- Having good public relations
It should be noted that liaison nurses had at least 3 hours of service for these patients for six months, at least 3 days a week.
In order to familiarize the liaison nurses with the research process, the method of training patients, and expected activities, a one-day workshop was held for 4 hours. In this workshop, training was provided on how to sample, how to follow up the patients and training, how to communicate with the departmental staff and the relevant physician, how to complete the informed consent form and the research questionnaire, and other tasks.
Each liaison nurse was deployed in the emergency department of the selected hospitals for sampling (56 samples from each hospital, in total 168 samples). It should be noted that in each hospital, half of the samples were considered as the control group and the other half as intervention. After the referral to the emergency department, the samples were randomly assigned to the intervention and control groups by the liaison nurse. Both groups initially completed informed consent form, a questionnaire containing demographic information, and a questionnaire on quality of life of patients with chronic heart disease and the intervention group members were supported by liaison nurse during the whole stay in the hospital (time of arrival to the hospital and hospitalization). These supports include training in reducing the anxiety and stress of the patient and his relatives, familiarizing the patient with his/her rights, familiarizing the patient and family with the treatment stages and process, and emotional support. During the hospitalization period, the liaison nurses also supported and trained patients in the CCU and Post CCU departments. After discharge, they were given a telephone call (liaison nurses’ mobile phone was given to the patients) and, if necessary, they were referred to their home in order to continue their care (depending on the patient's condition and need). For the sake of more safety for liaison nurses and ease of communication with patients, a SIM card and separate phone were provided for each liaison nurse. The control group underwent treatment and nursing care in the usual way and then referred to the hospital for further care. After 6 months of follow up by liaison nurses, the quality of life of the patients in the intervention and control groups was assessed using Minnesota Living with Heart Failure Questionnaire (MLHFQ), one of the most commonly used tools for measuring quality of life in patients with chronic heart failure. The content of this questionnaire was designed based on the nature of the illness and the response of the physical, emotional-spiritual, and socioeconomic aspects of quality of life to treatment and care. This questionnaire is highly reliable and validated. The statistics and information about the patients referring and participating in the research (in both intervention and control groups) included information such as the characteristics of the patients referring, the time of visit, the number of visits to the home or the making of telephone calls was recorded and kept by the liaison nurses. It should be noted that all stages of the implementation of the plan have been carried out with the coordination of the nurses of the department, the physician concerned, patient satisfaction and observance of ethical points. In order to provide standardized and uniform training by liaison nurses to the patients, the educational pamphlets were prepared using the latest references from the project implementer and with the help of nurses as well as educational interfaces of selected hospitals and confirmed by the educational supervisor of the relevant hospitals.
Specifying sample number:
The number of samples was obtained using the following equation in each group:
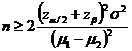
Where,
 [Probability of type I error is:]
[Probability of type I error is:]
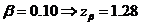 [Probability of type II error is:]
[Probability of type II error is:]
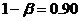 [Power is:]
[Power is:]
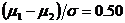 [Observed effect size is:]
[Observed effect size is:]
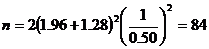 [Minimum sample required:]
[Minimum sample required:]According to the above formula, 84 samples were taken in each group and a total of 168 samples were considered.
Entry criteria for samples:
All subjects in the two intervention and control groups had the following conditions to enter the study:
1. Their diagnosis is merely heart failure (or diseases that have caused heart failure)
2. Have been hospitalized at least once in the past six months (have a history of heart disease)
3. There is no other underlying disease (if there is an underlying illness, the focus will be on the patient's heart problems)
4. Their age is between 20 and 76 years
5. There is no difference between male and female
6. There is no difference between a resident of Tehran or another city
7. Being fluent in Farsi (unless the liaison nurse is fluent in the patient's language)
8. Need to be hospitalized
9. Do not need a heart transplant.
Results
In this study, a total of 168 patients with chronic heart failure were evaluated in two intervention and control groups with a 100% response rate. Table 1 shows the distribution of the frequency of patients according to demographic characteristics.
| Personal specifications | Intervention group | Control group | Total | ||||
| No. | Percentage | No. | Percentage | No. | Percentage | ||
| Age | 30-44 | 5 | 6.1 | 5 | 5.9 | 10 | 6 |
| 45-54 | 30 | 36.6 | 24 | 28.2 | 54 | 32.3 | |
| 55-64 | 24 | 29.3 | 29 | 34.1 | 53 | 31.7 | |
| > 65 | 23 | 28 | 27 | 31.8 | 50 | 29.9 | |
| Gender | Female | 31 | 37.3 | 31 | 36.5 | 62 | 36.9 |
| Male | 52 | 62.7 | 54 | 63.5 | 106 | 63.1 | |
| Job | Homemaker | 20 | 24.1 | 20 | 23.5 | 40 | 23.8 |
| Self-employed | 31 | 37.3 | 29 | 34.1 | 60 | 35.7 | |
| Employed | 21 | 25.3 | 17 | 20 | 38 | 22.6 | |
| Retired | 10 | 12 | 16 | 18.8 | 26 | 15.5 | |
| Unemployed | 1 | 1.2 | 3 | 3.5 | 4 | 2.4 | |
| Education level | Under diploma | 15 | 18.5 | 23 | 27.1 | 38 | 22.9 |
| Diploma | 28 | 34.6 | 17 | 20 | 45 | 27.1 | |
| Associate D. | 5 | 6.2 | 14 | 16.5 | 19 | 11.6 | |
| Bachelor | 26 | 32.1 | 25 | 29.4 | 51 | 30.7 | |
| Master | 7 | 8.6 | 6 | 7.1 | 13 | 7.8 | |
| Marital status | Single | 8 | 10.7 | 3 | 4.1 | 11 | 7.4 |
| Married | 67 | 89.3 | 70 | 95.9 | 137 | 92.6 | |
| Other Diseases | Yes | 19 | 22.9 | 31 | 36.5 | 50 | 29.8 |
| No | 64 | 77.1 | 54 | 63.5 | 118 | 70.2 | |
| Disease type | Diabetes | 5 | 27.8 | 12 | 38.7 | 17 | 34.7 |
| Blood pressure | 6 | 33.3 | 4 | 12.9 | 10 | 20.4 | |
| Kidney disease | 2 | 11.1 | 7 | 22.6 | 9 | 18.4 | |
| Fat | 2 | 11.1 | 2 | 6.5 | 4 | 8.2 | |
| Others | 3 | 16.7 | 6 | 19.4 | 9 | 18.4 | |
Also, the results of the study indicate that the two intervention and control groups are homogeneous in terms of their personal characteristics. Independent t-test results show that the difference between the mean ages in both intervention and control groups is not statistically significant and the two groups are homogeneous in terms of age (p = .349).
The results of chi-square tests also show:
There are no statistical differences between the two intervention and control groups in terms of gender and they are homogeneous (p = .906).
There are no statistical differences between the two intervention and control groups in terms of job and they are homogeneous (p = .58).
There are no statistical differences between the two intervention and control groups in terms of education level and they are homogeneous (p = .071).
There are no statistical differences between the two intervention and control groups in terms of marital status and they are homogeneous (p = .128).
There are no statistical differences between the two intervention and control groups in terms of the history of other illnesses and they are homogeneous (p = .054).
Also, the patients who stated that they had other illnesses were not significantly different in the two intervention and control groups in terms of disease type and they are homogeneous (p = .463).
Based on the results of data analysis and the implementation of Independent Samples Test, quality of life in different dimensions of physical (p = .437), emotional-spiritual (p = .437), and socioeconomic (p = .750) was not statistically different in the two intervention and control groups (p > .05). In other words, the two groups were homogeneous in terms of quality of life before intervention. Table 2 shows the mean and standard deviation of the three dimensions of quality of life in patients with chronic heart failure before intervention.
| P* | SD | Mean | No. | Groups | |
| .862 | 4.96452 | 19.0998 | 83 | Intervention | Physical |
| 5.92795 | 19.2471 | 85 | Control | ||
| .437 | 5.02611 | 14.6988 | 83 | Intervention | Emotional-spiritual |
| 5.86566 | 14.0412 | 85 | Control | ||
| .750 | 4.53167 | 19.0241 | 83 | Intervention | Socioeconomic |
| 4.61677 | 19.2490 | 85 | Control |
Also, the results of data analysis show that quality of life in the three dimensions of physical, emotional-spiritual, and socioeconomic is of significant difference in both intervention and control groups after intervention (p < .05). The mean in the intervention group is lower than the control group, which means that the quality of life in the intervention group is better in all three dimensions of quality of life after the intervention. In terms of intervention, it has been effective in improving the quality of life in the three dimensions of quality in patients with chronic heart disease. Table 3 shows the mean and standard deviation of the three dimensions of quality of life in patients with chronic heart failure after intervention.
| P* | SD | Mean | No. | Groups | |
| .000 | 2.10550 | 8.7952 | 83 | Intervention | Physical |
| .000 | 2.36662 | 28.0739 | 85 | Control | |
| .000 | 1.56051 | 8.7470 | 83 | Intervention | Emotional-spiritual |
| .000 | 2.12251 | 21.9176 | 85 | Control | |
| .000 | 1.93670 | 8.0723 | 83 | Intervention | Socioeconomic |
| .000 | 1.99909 | 26.3647 | 85 | Control |
Discussion and conclusion
Considering the results of the present study and the effect of transitional care on improving the quality of life of the patients in different dimensions, it can be said that the transitional care model is a plan for providing comprehensive care for chronic heart patients in the hospital and its continuity in the patient's home. For thousands of patients suffering from chronic diseases of the heart or complex therapies, the transitional care model uses a managed care approach with emphasis on continued care, prevention and avoidance of complex complications and active involvement of the patient and the family in the care in the coordination of physician and has an effective role in improving the health of these patients7.
The transitional care model emphasizes identifying the patient's goals, designing and implementing a care plan and continuity of care between the hospital and the patient's home. Transitional care is provided as a complementary and supportive care by nurses at the patient's home and after discharge from the hospital8. In this model, patient care is provided through coordination between a professional and skilled nurse with the patient and his family, the physician and other members of the treatment team9,10. In this regard, the results of numerous studies confirm the results of this study and suggest that the transitional care method improves the outcomes of patients, including reducing the number of hospital admissions, reducing the cost of treatment, and improving their quality of life. For example, an intervention study was conducted in 2007 at the Clinical Research Center of the University of Griffith in Australia on the role of the liaison nurse in the hospital. The study suggests that as admission of the patient to the intensive care unit causes many stresses for the patient and his or her family, the transfer of patients from ICU to other units equally causes fear and stress for them. The purpose of this study was to investigate the effect of liaison nurses on patient and family anxiety experiences before transferring from the intensive care unit to the normal unit. This interventional study, designed as before and after intervention with the control group, was tested for four months. In the intervention group, the liaison nurse prepared the patient and his family for transfer to the normal unit, but in the control group the patient was transferred to the unit in the usual way. The results of the study showed that the anxiety level among the patients and their families was decreased in the intervention group and statistical tests showed a significant difference between the intervention and control groups in terms of anxiety level11. Another study was conducted in 2007 at the Pediatric Hospital in Melbourne, Australia. In this study, it was assumed that a liaison nurse would reduce the re-admission of children in the intensive care unit within 48 hours of discharge from this unit. In this study, a liaison nurse was considered as a bridge between the intensive and normal units. After a pilot year, 1388 children were discharged from the intensive care unit. During this period, 67 patients were never re-admitted, and overall, the rate of children's re-admission decreased from 5.4 to 4.8%. After a year of pilot study, staff and patients will be consulted about the impact of the liaison nurse. In this regard, 98.9% of staff members of the intensive care unit positively evaluated liaison nurse’s help, and 99% of the parents of the children considered the idea of liaison nurse as a positive idea. Other results from this study included: improving communication between parents and health care staff, improving the quality of the training provided in the unit, improving patient outcomes and reducing re-hospitalization in the intensive care unit12. Another study was conducted in 2014 at the Metropolitan Hospital in Argentina. The aim of this study was to investigate the role of liaison nurses in re-admission of patients to hospitals. The liaison nurse trained and monitored 200 patients over 18 years of age after discharge from the intensive care unit from April 1 to July 31, 2012. The samples were suffering from heart disease, respiratory illnesses, and diabetes. The results showed that only one-fifth of patients who had been followed up by the liaison nurse and after discharge from the ICU had to be re-visited and re-admitted13.
In general, it can be said that many people who use this model only use some of the model's components to suit their needs. Measurement of changes in the health status of patients through the use of this caring model illustrates the usefulness of the model in promoting health. Measurement of patients’ changes over time, e.g. symptoms of illness, physical functioning (cognitive, physical, mental and psychological state), and patient's quality of life, reflects the impact of the model on improving the patient's condition. Evaluation of patient's family and treatment team’s view on continuity of care in this model is another aspect of the role of transitional care model in improving patient health. Also, the change in the time of the first re-hospitalization, the number of hospitalization, and the number of hospitalized days after applying the model is another reason for its benefits and the investment required for its comprehensive application.
Acknowledgement: We would like to thanks all those who helped the researcher in this project, including the students as liaison nurses, as well as the staff of the target hospitals and also Vice-Chancellor of Research Affairs of the Shahid Beheshti University of Medical Sciences for financial support of the research project.
References
1. Choi Y (2017). Care Coordination and Transitions of Care. Medical Clinics of North America. 101(6), pp. 1041-51.
2. McColl-Kennedy JR, Hogan SJ, Witell L, Snyder H (2017). Cocreative customer practices: Effects of health care customer value cocreation practices on well-being. Journal of Business Research. 70, pp. 55-66.
3. Betz CL, Smith K, Van Speybroeck A, Jacobs RA, Rivera N, Lee J, et al (2018). Descriptive Analysis and Profile of Health Care Transition Services Provided to Adolescents and Emerging Adults in the Movin' On Up Health Care Transition Program. Journal of Pediatric Health Care. 32(3), pp. 273-84.
4. Tingley J, Dolansky MA, Walsh MN (2015). Team-Based Transitions of Care in Heart Failure. Heart Failure Clinics. 11(3), pp. 371-8.
5. Gronroos j (2010). Service management and marketing: A customer relationship approach: Wiley، Chichester.
6. Huber DL, Joseph ML, Halbmaier KA, Carlson M, Crill S, Krieger K, et al (2016). Leadership for Transitions of Care: An Active Learning Innovation. J Contin Educ Nurs. 47(2), pp. 82-8.
7. Bowman B, Zheng S, Yang A, Schiller B, Morfín JA, Seek M, et al (2018). Improving Incident ESRD Care Via a Transitional Care Unit. American Journal of Kidney Diseases.
8. Hader R (2016). Magnet Recognition- Excellence is the standard. Nursing Management. 41(6):6.
9. Naylor M, Brooten D, Campell R, Maislin G, McCauley K, Schwartz J (2006). Transitional care of older adults hospitalized with heart failure: a randomized, controlled trial. J Am Geriatr Soc. p. 52
10. Hirschman KB, Shaid E, McCauley K, Pauly MV, Naylor MD (2015). Continuity of Care: The Transitional Care Model. Online J Issues Nurs. p. 20(3):1
11. Chaboyer, W., et al (2017). The Intensive Care Unit liaison nurse towards a clear role description. Intensive and Critical Care Nursing, 20(2), pp. 77-86
12. Chaboyer, W., et al (2007). The impact of a liaison nurse on ICU nurses' perceptions of discharge planning. Australian Critical Care. 17(1), pp. 25-32
13. Alberto L, Zotárez H, Cañete ÁA, Niklas JEB, Enriquez JM, Gerónimo MR, et al (2014). A description of the ICU liaison nurse role in Argentina Intensive and Critical Care Nursing. 30(1), pp. 31-37
Author notes
rezapour.r@sbmu.ac.ir