research-article
Dispositional Mindfulness Mediates the Relationship between Psychotic Symptoms and Psychological Quality of Life
El mindfulness disposicional media la relación entre los síntomas psicóticos y la calidad de vida psicológica
Dispositional Mindfulness Mediates the Relationship between Psychotic Symptoms and Psychological Quality of Life
Clínica y Salud, vol. 35, no. 1, pp. 1-3, 2024
Colegio Oficial de la Psicología de Madrid
Received: 17 November 2023
Accepted: 20 November 2023
Funding
Funding source: Spanish Ministry of Science and Innovation
Contract number: PID2021-122987OA-I00
Funding statement: This study was supported by the R+D project PID2021-122987OA-I00 funded by the Spanish Ministry of Science and Innovation (MICIN) and AEI
ABSTRACT: Background: To assess the mediator effect of dispositional mindfulness on the relationship between psychotic symptoms and psychological quality of life of people experiencing psychosis. Method: One hundred thirty-eight participants with psychosis were recruited. Psychotic symptoms were assessed through the PANSS scale, dispositional mindfulness was assessed using the MAAS questionnaire, and psychological quality of life was tapped with the WHOQOL-BREF questionnaire. Mediational analysis was performed setting PANSS factors as independent variables, MAAS scores as mediator, and WHOQOL-BREF Psychological as dependent variable. Results: MAAS scores mediated the relationship between WHOQOL-BREF Psychological scores and PANSS Positive (b = -.246, BCa CI [-.345, -.153]), PANSS Negative (b = -.173, BCa CI [-.251, -.096]), and PANSS Depressed scores (b = -.227, BCa CI [-.31, -.148]). Conclusions: Dispositional mindfulness can ameliorate the negative impact of hallucinations, delusions, negative symptoms, and depression feelings on psychological quality of life of people experiencing psychosis.
Keywords: Psychosis, Dispositional mindfulness, Psychotic symptoms, Positive symptoms, Negative symptoms, Mediation analysis.
RESUMEN: Antecedentes: Evaluar el efecto mediador de la atención plena disposicional en la relación entre los síntomas psicóticos y la calidad de vida psicológica de las personas que experimentan psicosis. Método: Se reclutaron 138 participantes con psicosis. Los síntomas psicóticos se evaluaron mediante la escala PANSS, la atención plena disposicional se evaluó utilizando la escala MAAS y la calidad de vida psicológica se exploró con el cuestionario WHOQOL-BREF. Se realizó un análisis de mediación estableciendo los factores PANSS como variables independientes, los puntajes MAAS como mediador y WHOQOL-BREF Psicológico como variable dependiente. Resultados: Las puntuaciones en la MAAS mediaron la relación entre WHOQOL-BREF-Psicológico y PANSS Positivo (b = -.246, IC BCa [-.345, -.153]), PANSS Negativo (b = -.173, IC BCa [-.251, -.096]) y PANSS Depresión (b = -.227, IC BCa [-.31, -.148]). Conclusiones: El mindfulness disposicional puede reducir el impacto negativo de las alucinaciones, delirios, síntomas negativos y sentimientos de depresión en la calidad de vida psicológica de las personas que experimentan psicosis.
Palabras clave: Psicosis, Mindfulness disposicional, Síntomas psicóticos, Síntomas positivos, Síntomas negativos, Análisis de mediación.
Introduction
Mindfulness-based interventions applied to psychosis have shown broad positive findings improving psychological quality of life (Louise et al., 2018) and frequency of negative psychotic symptoms (López-Navarro & Al-Halabí, 2022), among other functional outcomes (Yip et al., 2022). Mindfulness-based interventions teach individuals to observe their own mental experiences with acceptance rather than struggling with the content of the experience. This behavioral tendency has been coined under the umbrella term of dispositional mindfulness (DM; Bishop et al., 2004).
Research about the relationship between DM and psychological quality of life has been increasing during the last decade. DM has been related with less pathognomonic symptoms (Calvete et al., 2021) and better treatment response (Tortella-Feliu et al., 2020). Regarding psychotic disorders, research has shown that people after a mindfulness-based intervention increase their DM (López-Navarro et al., 2020), but so far no study has addressed empirically if DM mediates the effect of psychotic symptoms on psychological quality of life.
Based on the suggestive findings reviewed above, our study aims to analyze the mediating effect of DM on the relationship between psychotic experiences and the psychological quality of life of people with psychosis.
Method
Participants
A cross-sectional study was conducted in three public community rehabilitation centers for people with psychosis. Inclusion criteria were: 1) age between 18-65, 2) a clinical record of paranoid schizophrenia, undifferentiated schizophrenia, or schizoaffective disorder, 3) being in a stable post-acute phase of illness, and 4) being able to understand and read Spanish language. Ethical approval was granted by the university research ethics committee.
Procedure
One hundred thirty-eight users from the public community rehabilitation centers were invited to participate. The users and their legal guardians were contacted by their regular psychiatrist or psychologist to arrange an interview to 1) be informed of the purpose of the study and 2) sign the informed consent and to schedule a date for the assessment.
Instruments
Demographical and clinical data were gathered through a case report form covering age, sex, years of education, and diagnostic according to clinical record and years since initial diagnosis.
Psychotic experiences were assessed with the Spanish version of the of the Positive and Negative Syndrome Scale (PANSS; Peralta & Cuesta, 1994). Scoring was performed according to the five-factor model of Wallwork et al. (2012): Positive (P1, P3, P5, G9), Negative (N1, N2, N3, N4, N6, G7), Disorganized/Concrete (P2, N5, G11), Excited (P4, P7, G8, G14), and Depressed factors (G2, G3, G6).
To assess psychological quality of life we used the Spanish version of the World Health Organization Quality of Life-Bref (WHOQOL-BREF; Lucas Carrasco, 1998). The WHOQOL-BREF is a 26-item scale that assesses quality of life through four dimensions: physical health, psychological health, social relationships, and environment. Based on the aim of the study we used the scores of the psychological dimension as outcome variable.
To assess DM, we used the Spanish version of the Mindfulness Attention Awareness Scale (MAAS; Soler et al., 2012). This 15-item scale focuses on the attention/awareness component of mindfulness construct. MAAS has been used previously in studies with people diagnosed with psychosis (López-Navarro et al., 2020). The Spanish version of the MAAS has demonstrated good reliability indicators and strong temporal stability, as reported by Soler et al. (2012).
Data Analysis
Descriptive statistics were generated for the sample covering demographic and clinical data. To assess the mediational effect of DM we used a mediation analysis following Hayes’ (2017) recommendations. Scores on PANSS factors were set as the independent variable, the scores on WHOQOL-BREF Psychological as the dependent variable, and MAAS scores as the mediator variable. We bootstrapped the specific indirect effects to reduce parameter bias and the coefficients were standardized. The bootstrap estimates were based on 5,000 samples, and a 95% CI was used. Data were analyzed using SPSS 27 for Windows with mediation analysis PROCESS plugin (Hayes, 2017).
Results
The mean age of the sample was 37.94 years (SD = 7.62) with a mean duration of disorder of 12.48 years (SD = 6.27). Table 1 displays detailed information about the demographic and clinical features of the sample.
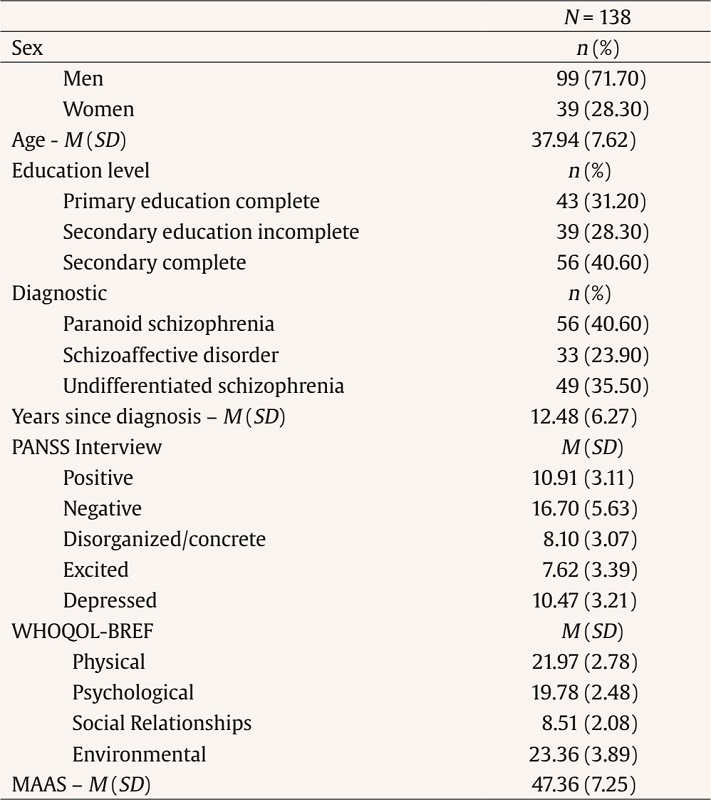
Note. PANSS = Positive and Negative Syndrome Scale; WHOQOL-BREF = World Health Organization Quality of Life-Bref; MAAS = Mindfulness Attention Awareness Scale.
Mediation analysis found a statistically significant indirect effect through MAAS scores on Positive (b = -.246, BCa CI [-.345, -.153]), Negative (b = -.173, BCa CI [-.251, -.096]), and Depressed factor (b = -.227, BCa CI [-.31, -.148]). However, we did not find a statistically significant indirect effect through MAAS scores on Disorganized (b = -.064, BCa CI [-.153, .019]) nor Excited factor scores (b = -.058, BCa CI [-.135, .017]). There were no statistically significant differences between sex on the variables included in the mediational analyses. Diagrams of the statistically significant mediation models are shown in Figure 1.
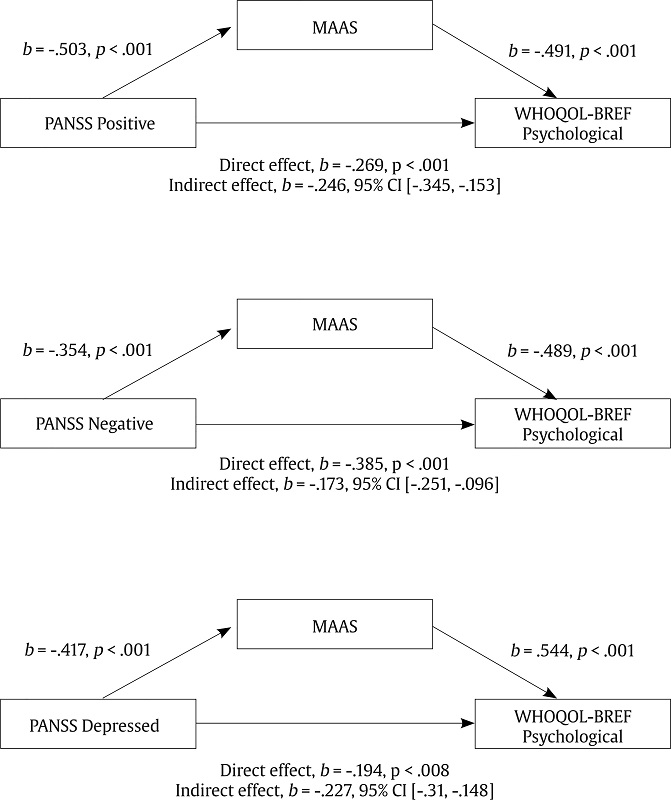
Figure 1
Mediation Diagram. Standardized Coefficients as well Bootstrapped Confidence Intervals are Reported.
Note. PANSS = Positive and Negative Syndrome Scale; WHOQOL-BREF = World Health Organization Quality of Life-Bref; MAAS = Mindfulness Attention Awareness Scale.
Discussion
The main finding of our study is that DM mediates the negative effect of psychotic symptoms on psychological quality of life of people experiencing psychosis. A high DM can lessen the effect of positive, negative, and depression symptoms on psychological well-being.
Convergent with prior research on other mental disorders, the DM affects the relationship between pathognomonic symptoms and subjective psychological quality of life. Also, our findings provide empirical evidence to support the notion that it is the relationship with the psychotic experiences, rather than the experiences themselves, that determines a person’s well-being (Chadwick, 2019).
The main limitation of our study is gender distribution. This gender imbalance may underrepresent female patients, although it is in line with the prevalence of psychosis in the general population. The main strengths are the sample size, which is enough to test the hypothesis, and the use of a statistical approach that goes beyond simple regression methods.
In sum, our study is the first to provide data about the mediating effect of DM on the relationship between psychotic symptoms and psychological quality of life. Future research should explore how to use this finding to optimize interventions for people experiencing psychosis, especially in public mental health centers (Sampietro et al., 2023).
References
Bishop, S. R., Lau, M., Shapiro, S., Carlson, L., Anderson, N. D., Carmody, J., Segal, Z. V, Abbey, S., Speca, M., Velting, D., & Devins, G. (2004). Mindfulness: A proposed operational definition. Clinical Psychology: Science and Practice, 11(3), 230-241. https://doi.org/10.1093/clipsy.bph077
Calvete, E., Franco, M. A. R., Oñate, L., Alonso, M. S.-I., & Bermejo-Toro, L. (2021). Trait mindfulness, rumination, and well-being in family caregivers of people with acquired brain injury. Clínica y Salud, 32(2), 71-77. https://doi.org/10.5093/clysa2021a5
Chadwick, P. (2019). Mindfulness for psychosis: A humanising therapeutic process. Current Opinion in Psychology, 28, 317-320. https://doi.org/10.1016/j.copsyc.2019.07.022
Hayes, A. F. (2017). Introduction to mediation, moderation, and conditional process analysis, second edition: A regression-based approach. Guilford Publications.
López-Navarro, E., & Al-Halabí, S. (2022). Effects of mindfulness on psychotic symptoms: insights from a randomized clinical trial. Psychosis, 14(1), 93-98. https://doi.org/10.1080/17522439.2021.1889649
López-Navarro, E., Del Canto, C., Mayol, A., Fernández-Alonso, O., Reig, J., & Munar, E. (2020). Does mindfulness improve inhibitory control in psychotic disorders? A randomized controlled clinical trial. International Journal of Clinical and Health Psychology, 20(3), 192-199. https://doi.org/10.1016/j.ijchp.2020.07.002
Louise, S., Fitzpatrick, M., Strauss, C., Rossell, S. L., & Thomas, N. (2018). Mindfulness- and acceptance-based interventions for psychosis: Our current understanding and a meta-analysis. Schizophrenia Research, 192, 57-63. https://doi.org/10.1016/j.schres.2017.05.023
Lucas-Carrasco, R. (1998). Versión española del WHOQOL. Editorial Ergón.
Peralta, V., & Cuesta, M. (1994). Validación de la escala de los síndromes positivo y negativo (PANSS) en una muestra de esquizofrénicos españoles. Actas Luso-Españolas de Neurología y Psiquiatría, 22(4), 171-177.
Sampietro, H. M., Rojo, E., & Gómez-Benito, J. (2023). Recovery-oriented care in public mental health policies in Spain: Opportunities and barriers. Clínica y Salud, 34(1), 35-40. https://doi.org/10.5093/clysa2023a4
Soler, J., Tejedor, R., Feliu-Soler, A., Pascual, J. C., Cebolla, A., Soriano, J., Alvarez, E., & Perez, V. (2012). Psychometric proprieties of Spanish version of Mindful Attention Awareness Scale (MAAS). Actas Españolas de Psiquiatría, 40(1), 19-26. https://doi.org/10.1037/t86572-000
Tortella-Feliu, M., Luís-Reig, J., Gea, J., Cebolla, A., & Soler, J. (2020). An exploratory study on the relations between mindfulness and mindfulness-based intervention outcomes. Mindfulness, 11(11), 2561-2572. https://doi.org/10.1007/s12671-020-01471-x
Wallwork, R. S., Fortgang, R., Hashimoto, R., Weinberger, D. R., & Dickinson, D. (2012). Searching for a consensus five-factor model of the Positive and Negative Syndrome Scale for schizophrenia. Schizophrenia Research, 137(1-3), 246-250. https://doi.org/10.1016/j.schres.2012.01.031
Yip, A. L. K., Karatzias, T., & Chien, W. T. (2022). Mindfulness-based interventions for non-affective psychosis: A comprehensive systematic review and meta-analysis. Annals of Medicine, 54(1), 2339-2352. https://doi.org/10.1080/07853890.2022.2108551
Notes
Notes
Author notes
Correspondence: Emilio.lopez@uib.es (E. López-Navarro).
Conflict of interest declaration