Artículos

This work is licensed under Creative Commons Attribution-NonCommercial-ShareAlike 3.0 International.
Received: 20 August 2020
Accepted: 25 October 2020
DOI: https://doi.org/10.5281/zenodo.4278348
Abstract: This article shows the development and implementation of a functional telerehabilitation system by using interactive virtual environments and biomedical technologies in patients with cerebral palsy sequelae, with limited upper and lower limb movements. The system facilitates therapeutic intervention with telerehabilitation through video games developed in Scratch®, by means of Kinect as an interface for acquiring movements. By developing a video game in an easily configured programming language, therapists can change and adjust the challenges of each therapeutic intervention in an interactive, friendly and funny way, according to progress, and motivating the patient to continue with his evolution. Results show improvement in children with cerebral palsy, with movement limitations of their upper or lower limbs.
Keywords: Telerehabilitation, disability, virtual reality, video games, biomedical..
Resumen: En este artículo se muestra el desarrollo e implementación de un sistema de telerehabilitación funcional empleando entornos virtuales interactivos y tecnologías biomédicas en pacientes con secuelas de parálisis cerebral con limitación en los movimientos de las extremidades superiores e inferiores. El sistema facilita la intervención terapéutica empleando la telerehabilitación a través de videojuegos desarrollados en Scratch®, con el uso de Kinect como interfaz de adquisición de movimientos. Al desarrollar un videojuego en un lenguaje de programación de fácil configuración, permite que los terapeutas puedan cambiar y ajustar los retos de cada intervención terapéutica de forma interactiva, amigable y divertida, acorde al progreso y motivando al paciente a continuar con su evolución. Los resultados muestran mejora en niños con parálisis cerebral, con limitaciones en movimiento a nivel de miembros superiores o inferiores.
Palabras clave: Telerehabilitación, discapacidad, realidad virtual, videojuegos, biomédica..
INTRODUCTION
Telerehabilitation has dramatically expanded in recent years due to technological advance, increased telecommunication speed, and decreased costs of computer hardware and software (De Araujo et al., 2019; Hukic et al., 2017). It can be divided into three main categories: image-based telerehabilitation, sensor-based telerehabilitation, and virtual technology-based telerehabilitation (H et al., 2014). Therapies through a virtual environment seem to promote motor learning, retention of learned skills, and skill transfer to real-world situations (Levac et al., 2019; Quadrado et al., 2019). Virtual reality (VR) is used in physical rehabilitation to improve motor function (Dockx et al., 2016; Dulau et al., 2019; Glegg, 2017). Currently, this technology is applied more frequently in pathologies of neurological origin (stroke, Parkinson's disease, spinal cord injuries, infantile cerebral palsy, and others), achieving improved results in the patients’ intervention and motivation to attain a prominent level of functional (Barrios et al., 2019; Benrachou et al., 2020; Ferencik et al., 2020; Shahab et al., 2019).
VR environment depends on the technology (hardware and software) used and, considering the immersion degree of the patient in the environment, these systems can be immersive and non-immersive (Feng et al., 2019). In immersive systems, the user is fully integrated into the virtual environment, watching only the computer-generated images, blocking the rest of the physical world (Arlati et al., 2020; Scheideman-Miller et al., 2003). Glasstrom, IREX, and Playstation EyeMotion are among these systems. In non-immersive or semi- immersive systems, the user perceives part of the real world and part of the virtual world-environment, there is no total immersion in the virtual environment. Currently, the most widely used non-immersive systems are Virtual Teacher, X-box, Cyberglobe, Virtual Reality Motion, Pneumoglobe and Nintendo-Wii (Viñas-Diz & Sobrido- Prieto, 2016).
State of the art
According to (Ramírez et al., 2014) virtual reality-based therapy has a specific and stimulating functional context for patients, bringing direct benefit to both the patient and the therapist due to the adaptability of these systems. The authors carry out tests with patients between 6 and 12 years of age with disabilities in the upper extremities, based on a hardware and software architecture through video games that induce particular physical activities in the patient, seeking their attention through dynamic and entertaining content in an interactive way. Likewise, (Yagüe et al., 2016) also confirm the beneficial and interesting application of the video game mediated by new technologies, for the physiotherapeutic treatment of cerebral palsy.
(Eng et al., 2007) in their article on stroke rehabilitation using virtual reality, they review the main immersive and non-immersive virtual reality systems used in the treatment of stroke patients, also inquiring about the mechanisms of neuroplasticity and cortical reorganization.
(Farreny et al., 2012) carried out an investigation titled Play for health (P4H): a new tool in telerehabilitation. P4H is a low-cost, open telerehabilitation system based on the use of video games and interaction methods to improve physical and cognitive deficits. The objective of the research was to present P4H, identify itsacceptance and describe the organizational repercussions of its introduction into the rehabilitation service.
In recent years, it has been seen how the emergence of new emerging virtual reality technologies are used as telerehabilitation tools to improve alternatives and options for new treatments. (Fonseca et al., 2020; Yeh et al., 2019) in their research propose systems that allow people with disabilities to perform exercises in the comfort of their homes and regardless of restrictions. They use the Kinect to acquire the body models of the patients, and through image processing they analyze the different situations. An investigation carried out by (Casanova et al., 2015), proposes a system for the physical rehabilitation of patients with multiple pathologies, through dynamics with video games, and the movements of the patients are analyzed using specific software. They relied on the use of the Kinect sensor, designed to entertain the patient in her therapy through quotesgames and at the same time provide the therapist with data capture and analysis with motion capture (MoCap).
(Couto Soares et al., 2013) in their research they propose a home rehabilitation program based on video games, using the Kinect sensor. Rehabilitation treatments are aimed at cardiovascular diseases (CVD), whichcontribute greatly to mortality and morbidity worldwide. The proposal includes exercise-based programs, tailored to each patient, that aim to restore and improve cardiac function, decrease disability, reduce mortality, improve quality of life, and reduce treatment costs.
(Pachoulakis et al., 2017) investigate and implement a Kinect-based physiotherapy platform that is tailored to each patient with Parkinson's disease (PD) and employ the Kinect sensor to extract 3D skeletal data in real time.
This article shows the SmartRehab telerehabilitation system, which allows the application of rehabilitation protocols specially designed for patients with cerebral palsy, taking into account the characteristics of the patients and a simple programming that allows the configuration according to the progress of the patients.
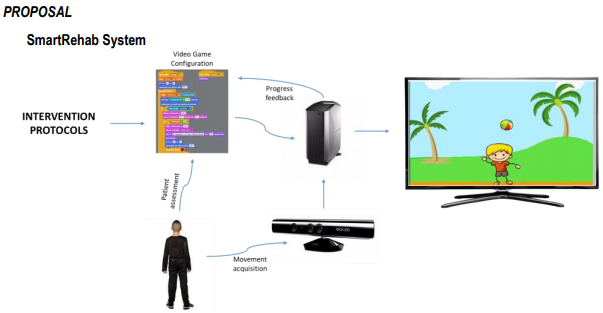
Figure 1. SmartRehab System (Intervention Protocols, Video Game Configuration, Progress Feedback, Movement Acquisition, Patient Assessment)
The developed remote rehabilitation system in virtual reality environment "SmartRehab", is shown in Figure 1, where the main elements can be observed. The system starts from the intervention protocols design considering the patient characteristics, after having made an assessment. The assessment establishes the intervention protocol allowing to adjust the challenges that the patient would have to face in the video game. The patient's movements are received through the Kinect, which sends the data to the software developed by using Scratch. The software, through internal coding connecting to the Kinect SDK, performs image processing for decision-making. One of the video games’ code is shown in Figure 2 (Frog). It allows easy configuration, so that therapists can change and adjust the challenges of each therapeutic intervention in an interactive, friendly and fun way, according to progress and motivating the patient to continue with his evolution.
The platform has a collection of 4 video games (Frog, Basket, Basketball, Volleyball) considering rehabilitation protocols designed especially for patients with cerebral palsy. Each exercise uses a movement pattern with very light processing demands for real-time calculations. Results are saved to be used to improve the rehabilitation protocol and video games.
Platform Development
Scratch® is a visual programming language developed by the Lifelong Kindergarten Group at the MIT Media Lab (Scratch, 2018). It manly allows to develop mental skills by learning programming without having deep code knowledge. Its characteristics linked to the easy understanding of computational thinking have made it widely used in education for children, adolescents and adults. Scratch allows users to use event-driven programming with multiple active objects called sprites. The sprites can be painted as vector graphics or bitmaps, from the Scratch website itself by using a simple editor that is part of the project, or they can also be imported from external sources including "webcamera". Scratch 1.x source code is under GPLv2 and "ScratchSource Code License".
Figure 2. Videogame Frog Code
RESULTS
Tests were carried out with children with cerebral palsy for validation of the developed system. The research was carried out within the facilities of the neurorehabilitation laboratory of the Antonio José de Sucre University Corporation, in children with limitations in upper limb movement due to cerebral palsy sequelae, whose parents voluntarily accepted, through informed consent, that their children participated in the study. The sample is non- probabilistic, and depended on the number of children who attended the facilities and who meet the following criteria:
Inclusion criteria:
-
Age between 5 and 12 years.
-
Cognitively high children
-
Socioeconomic stratum 1 and 2
-
Gross motor level 1 and 2. Exclusion criteria:
-
Patients with hearing and visual injuries.
-
Patients with ataxias.
-
Patients with unresolved traumatic injuries.
Initially, the disability condition in which children were found with cerebral palsy sequelae with alterations of upper extremities, was evaluated to determine the disability level they were in, and thus, be able to specify their intervention plan through videogame. The Gross Motor test was applied to assess the child's condition.

Figure 3. Patient 1 with cerebral palsy using SmartRehab.
Twenty work sessions were carried out with each patient, conducting pilot tests with the virtual and interactive biomedical platform of the upper limb protocol aimed at patients who meet the inclusion criteria. Tests were carried out under the supervision of trained professionals, physiotherapists previously trained in video games for the total satisfaction of the carried-out interventions.
After sessions were over, the child's condition was re-assessed to see the level of evolution in postural control through video games in children with cerebral palsy sequelae in upper extremities. Figure 3 shows the platform use, consisting of a computer, a television, a Kinect and the virtual reality system. Three children diagnosed with cerebral palsy participated in the research. From 10 to 15 years old, meeting the gross motor I and II inclusion criteria. Two were male and one female.
Figure 4 shows the results of the initial assessment, where the score in patient #1 in lying and rolling (dimension A) is observed to reach up to 90%; sitting (dimension B) 91%; crawling and kneeling (dimension C) 64%; standing (dimension D) 66%; along with walking, running and jumping (dimension E) with a score of 36%. In patient # 2, when lying down and rolling, the child reaches 80%; in sitting 93%; in crawling and kneeling, a score of 88%; in standing the child gave a score of 79%; along with walking, running and jumping with a percentage of 86%. In patient # 3, in lying and rolled position, the child achieved a score of 96%; in sitting the child has a score of 98%; in crawling and kneeling 80%; in standing the child gave a score corresponding to 64%; whereas in walking, running and jumping a percentage of 29%. This indicates that patients #1 and #2 present great difficulties for standing dimensions; and for walking, running and jumping.
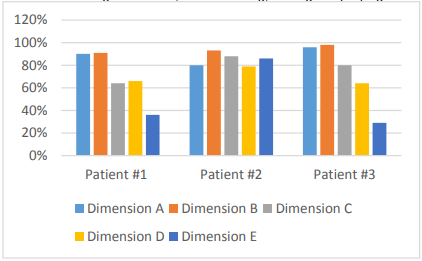
Figure 4. Initial assessment, gross motor
Figure 5 shows the result of the final gross motor assessment. In patient # 1, when lying down and rolling, the child reaches a percentage of 100%; 96% sitting; in crawling and on knees 66%; in standing the child gave a percentage of 76%; and in walking, running, and jumping 55%. In patient #2, in lying and rolling the child reaches a percentage of 92%; 95% sitting; in crawling and kneeling 90%; in standing, a percentage of 100%; and in walking, running and jumping 100%. In patient # 3, when lying and rolling the child reaches a percentage of 96%; in sitting the child has 100%; in crawling and on knees 92%; standing, 74%; whereas in walking, running and jumping with a percentage of 40%. After the pilot test, the patients improved in all the gross motor dimensions, especially in the standing position.
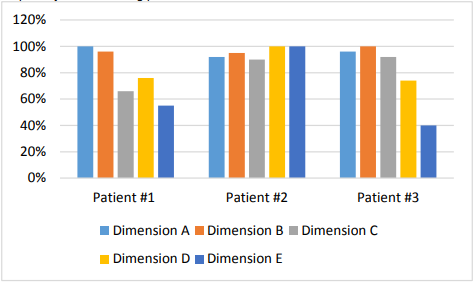
Figure 5. Final assessment, gross motor.
It can be observed when comparing the tests before and after, that the video game-based intervention protocol improves limitations in the upper extremities and in postural control. All the patients showed evolution in each scale and evaluation item, indicating that there were satisfactory results and, therefore, the intervention combination strategy was beneficial.
CONCLUSIONS
The video game developed from this research, called SmartRehab, facilitates therapeutic intervention using telerehabilitation, since it has an interface that allows therapists to change and adjust the challenges of each intervention in an interactive, friendly and funny way, according to progress and motivating the patient to continue with its evolution. Through the experience carried out during the intervention, it was possible to conclude that the virtual rehabilitation modality by means of video games with the Kinect sensor is an intervention alternative to patients with cerebral palsy sequelae, implemented with the application of the different neurorehabilitation techniques, since they are a good complement for the patient rehabilitation.
BIODATA
Liliana RODRÍGUEZ TOVAR: Physiotherapist, specialist and master's degree in Neurorehabilitation, research teacher. Antonio José de Sucre University Corporation. Faculty of Health Sciences.
Javier E. SIERRA: Electronic Engineer, Master in Engineering, Doctor in Telecommunication, Research Professor. University of Sucre. Faculty of Engineering.
Claudia PACHÓN FLÓREZ: Physiotherapist, Master in Occupational Risk Prevention, Research Professor, Antonio José de Sucre University Corporation. Faculty of Health Sciences.
Meryene BARRIOS BARRETO: Physiotherapist, Master of Education, research professor, Antonio José de Sucre University Corporation. Faculty of Health Sciences.
BIBLIOGRAPHY
ARLATI, S., KEIJSERS, N., FERRIGNO, G., & SACCO, M. (2020). A protocol for the comparison of reaching gesture kinematics in physical versus immersive virtual reality. 2020 IEEE International Symposium on Medical Measurements and Applications (MeMeA), 1–6. https://doi.org/10.1109/MeMeA49120.2020.9137117
BARRIOS, M., RODRIGUEZ, L., PACHÓN, C., MEDINA, B., & SIERRA, J. E. (2019). Functionaltelerehabilitation based on interactive virtual environments as a rehabilitation proposal for patients with disabilities. Espacios, 40(25), 1–14. https://www.revistaespacios.com/a19v40n25/a19v40n25p01.pdf
BENRACHOU, D. E., MASMOUDI, M., DJEKOUNE, O., ZENATI, N., & OUSMER, M. (2020). Avatar-Facilitated Therapy and Virtual Reality: Next-Generation of Functional Rehabilitation Methods. 020 1st International Conference on Communications, Control Systems and Signal Processing (CCSSP), 298–304. https://doi.org/10.1109/CCSSP49278.2020.9151528
CASANOVA, M., MUÑOZ, J., HENAO, O., & DAVID, L. (2015). Exergames como herramienta para la evaluación del equilibrio postural en un paciente con esclerosis múltiple. IEEE. https://www.researchgate.net/profile/John_Munoz4/publication/283546834_Exergames_as_a_tool_for_the_ assessment_of_postural_balance_in_a_patient_with_multiple_sclerosis_The_role_of_biomechanical_analys is_in_the_quantification_of_movement/links/57964ba708aeb
COUTO SOARES, J., VIEIRA, A., & GABRIEL, J. (2013). Assisted living: Home physiotherapy demo. 2013 2nd Experiment@ International Conference (Exp.at’13), 162–163.https://doi.org/10.1109/ExpAt.2013.6703054
DE ARAUJO, F. M. A., VIANA FILHO, P. R. F., ADAD FILHO, J. A., FONSECA FERREIRA, N. M., VALENTE,A., & SOARES, S. F. S. P. (2019, August 1). A new approach of developing games for motor rehabilitation using Microsoft Kinect. 2019 IEEE 7th International Conference on Serious Games and Applications for Health, SeGAH 2019. https://doi.org/10.1109/SeGAH.2019.8882457
DOCKX, K., BEKKERS, E. M. J., VAN DEN BERGH, V., GINIS, P., ROCHESTER, L., HAUSDORFF, J. M.,MIRELMAN, A., & NIEUWBOER, A. (2016). Virtual reality for rehabilitation in Parkinson’s disease. In Cochrane Database of Systematic Reviews (Vol. 2016, Issue 12). John Wiley and Sons Ltd. https://doi.org/10.1002/14651858.CD010760.pub2
DULAU, E., BOTHA-RAVYSE, C. R., & LUIMULA, M. (2019). Virtual reality for physical rehabilitation: A Pilot study How will virtual reality change physical therapy? 10th IEEE International Conference on Cognitive Infocommunications, CogInfoCom 2019 - Proceedings, 277–282.https://doi.org/10.1109/CogInfoCom47531.2019.9089980
ENG, K., SIEKIERKA, E., CAMEIRAO, M., ZIMMERLI, L., PYK, P., DUFF, A., EROL, F., SCHUSTER, C.,BASSETTI, C., KIPER, D., & VERSCHURE, P. (2007). Cognitive virtual-reality based stroke rehabilitation.IFMBE Proceedings, 14(1), 2839–2843. https://doi.org/10.1007/978-3-540-36841-0_718
FARRENY, M. A., BUEN, M. C., AGUIRREZABAL, A., FERRIOL, P., TOUS, F., & ALCALDE, M. A. (2012).Play for health (P4H): una nueva herramienta en telerehabilitación. Rehabilitación, 46(2), 135–140. https://doi.org/10.1016/j.rh.2012.01.001
FENG, H., LI, C., LIU, J., WANG, L., MA, J., LI, G., GAN, L., SHANG, X., & WU, Z. (2019). Virtual realityrehabilitation versus conventional physical therapy for improving balance and gait in parkinson’s disease patients: A randomized controlled trial. Medical Science Monitor, 25, 4186–4192. https://doi.org/10.12659/MSM.916455
FERENCIK, N., BUNDZEL, M., HRUSKA, L., & CIK, I. (2020). Patient assessment using computer games in rehabilitation. SAMI 2020 - IEEE 18th World Symposium on Applied Machine Intelligence and Informatics, Proceedings, 51–55. https://doi.org/10.1109/SAMI48414.2020.9108758
FONSECA, A., ALULEMA, D., PINEDA, F., & MOROCHO, D. (2020). Auxiliar Prototype for Physiotherapy Using Kinect. 2020 Seventh International Conference on EDemocracy & EGovernment (ICEDEG), 269–274. https://doi.org/10.1109/ICEDEG48599.2020.9096782
GLEGG, S. (2017). Virtual Rehabilitation with Children: Challenges for Clinical Adoption [From the Field]. IEEE Pulse, 8(6), 3–5. https://doi.org/10.1109/MPUL.2017.2750858
HUKIC, A., DOLINSEK, I., ZAJC, D., VESEL, M., KRIZMANIC, T., POTISK, K. P., BLAZICA, B., BIASIZZO,A., & NOVAK, F. (2017). Telerehabilitation of upper extremities with target based games for persons with Parkinson’s disease. International Conference on Virtual Rehabilitation, ICVR, 2017-June. https://doi.org/10.1109/ICVR.2017.8007466
LEVAC, D. E., TAYLOR, M. M., PAYNE, B., & WARD, N. (2019). Influence of virtual environment complexity on motor learning in typically developing children and children with cerebral palsy. International Conference on Virtual Rehabilitation, ICVR, 2019-July. https://doi.org/10.1109/ICVR46560.2019.8994487
PACHOULAKIS, I., XILOURGOS, N., PAPADOPOULOS, N., & ANALYTI, A. (2017). Enrichment of a Kinect-based Physiotherapy and Assessment Platform for Parkinson’s disease Patients. Advances in Image and Video Processing, 5(1), 31. https://doi.org/10.14738/aivp.51.2750
QUADRADO, V. H., SILVA, T. D. DA, FAVERO, F. M., TONKS, J., MASSETTI, T., & MONTEIRO, C. B. DEM. (2019). Motor learning from virtual reality to natural environments in individuals with Duchenne muscular dystrophy. Disability and Rehabilitation: Assistive Technology, 14(1), 12–20. https://doi.org/10.1080/17483107.2017.1389998
RAMÍREZ, E., MORENO, F., OJEDA, J., MENA, C., RODRÍGUEZ, O., RANGEL, J., & ÁLVAREZ, S. (2014).Un Framework para la Rehabilitación Física en Miembros Superiores con Realidad Virtual. Revista Venezolana de Computación, 1(1), 8–16. http://saber.ucv.ve/ojs/index.php/rev_vcomp/article/view/6931/6671
SCHEIDEMAN-MILLER, C., CLARK, P. G., MOORAD, A., POST, M. L., HODGE, B. G., & SMELTZER, S.(2003). Efficacy and sustainability of a telerehabilitation program. Proceedings of the 36th Annual Hawaii International Conference on System Sciences, HICSS 2003. https://doi.org/10.1109/HICSS.2003.1174380
SCRATCH, F. (2018). Scratch - Imagine, Program, Share. MIT Media Lab. https://scratch.mit.edu/
SHAHAB, M., RAISI, M., HEJRATI, M., TAHERI, A. R., & MEGHDARI, A. (2019). Virtual Reality Robot forRehabilitation of Children with Cerebral Palsy (CP). ICRoM 2019 - 7th International Conference on Robotics and Mechatronics, 63–68. https://doi.org/10.1109/ICRoM48714.2019.9071878
VIÑAS-DIZ, S., & SOBRIDO-PRIETO, M. (2016). Virtual reality for therapeutic purposes in stroke: A systematic review. Neurología (English Edition), 31(4), 255–277. https://doi.org/10.1016/j.nrleng.2015.06.007
YAGÜE, S., LEKUONA, A., & SANZ, R. (2016). Los videojuegos en el tratamiento fisioterápico de la parálisis CEREBRAL. FISIOTERAPIA, 38(6), 295–302. HTTPS://DOI.ORG/10.1016/J.FT.2015.11.005
YEH, S. C., LEE, S. H., CHAN, R. C., & CHEN, S. (2019). A kinect-based system for stroke rehabilitation. Proceedings - 2019 12th International Conference on Ubi-Media Computing, Ubi-Media 2019, 192–198. https://doi.org/10.1109/Ubi-Media.2019.00045
