Review article
Received: 25 July 2023
Revised document received: 24 September 2023
Accepted: 16 December 2023
Published: 30 December 2023
DOI: https://doi.org/10.25100/cm.v54i4.5709
Funding
Funding source: Directorate General of Research (Dirección General de Investigaciones) of the Universidad Santiago de Cali
Contract number: No. 02-2023
Funding statement: This research has been funded by the Directorate General of Research (Dirección General de Investigaciones) of the Universidad Santiago de Cali under call No. 02-2023
Abstract
Background: The proprioceptive approach can effectively improve strength, mobility, edema reduction, and pain reduction, which in turn has a positive impact on functionality.
Objective: To identify proprioceptive rehabilitation strategies reported in the literature in adults with traumatic wrist injuries.
Methods: A scoping review was performed following the parameters of the Prisma ScR strategy. We included research with adult patients diagnosed with posttraumatic wrist injuries who used proprioceptive rehabilitation. Pain, functionality, strength, joint mobility ranges, and edema were evaluated.
Results: After removing duplicates and applying the exclusion criteria, a total of 123 articles were found, which left six articles, including 125 patients. Rehabilitation protocols based on proprioceptive neuromuscular facilitation and using sensorimotor tools that promote wrist recovery have been generated. In addition, other approaches have been established, such as motor imagery, which generates a work of identification and organization of movement, improving pain and manual function. However, longer follow-ups, standardization of the instruments used during proprioceptive intervention, and increasing the observed population are needed to generate a recommendation for early intervention and cost-benefit estimates.
Conclusion: Proprioceptive rehabilitation has demonstrated benefits in the recovery of the lower limb and hip or back. However, for the rehabilitation of traumatic wrist injuries, it is research pending. Well-described data and good quality designs are needed to routinely propose this strategy in the clinic.
Key words: Hand injuries, wrist injuries, proprioception, physical therapy modalities, rehabilitation.
Resumen
Antecedentes: El enfoque propioceptivo puede mejorar de manera efectiva la fuerza, la movilidad, la reducción del edema y la disminución del dolor; lo que a su vez tiene un impacto positivo en la funcionalidad.
Objetivo: Identificar las estrategias de rehabilitación propioceptiva reportadas en la literatura, en adultos con lesiones traumáticas de muñeca.
Metódos: Se efectuó una revisión de alcance siguiendo los parámetros de la estrategia Prisma ScR. Se incluyeron investigaciones con pacientes adultos, diagnóstico de lesión postraumática de muñeca, que utilizaron rehabilitación propioceptiva. Se evaluó el dolor, la funcionalidad, la fuerza, los rangos de movilidad articular y el edema.
Resultados: Se incluyeron seis artículos, que involucraron 125 pacientes al aplicar los criterios de exclusión. Se han generado protocolos de rehabilitación basados en facilitación neuromuscular propioceptiva y el uso de herramientas sensoriomotoras que promueven la recuperación de la muñeca. Además, se han establecido otros abordajes como la imaginería motora, que genera un trabajo de identificación y organización del movimiento, mejorando el dolor y la función manual. Faltan seguimientos de mayor tiempo, estandarización de los instrumentos utilizados durante la intervención propioceptiva y aumentar la población observada para generar una recomendación de intervención temprana y estimaciones entre el costo y el beneficio.
Conclusión: La rehabilitación propioceptiva ha demostrado beneficios en la recuperación del miembro inferior y la cadera o espalda. Para la rehabilitación de las lesiones traumáticas de muñeca, es un pendiente de la investigación. La información bien descrita y los diseños de buena calidad son necesarios para proponer rutinariamente esta estrategia en la clínica.
Palabras clave: Lesiones en las manos, lesiones en la muñeca, propiocepción, modalidades de fisioterapia, rehabilitación.
Remark

Introduction
Traumatic injuries of the wrist are frequent; out of 436 traumatic injuries of the upper extremity, 77.0 % are of the wrist, and of these, 38.6 % are fractures of the distal third of the radius, which can generate functional, proprioceptive, and occupational limitations 1,2. Proprioceptive impairment has gained importance in recent years, and proprioceptive re-education practices have been postulated as the primary strategy to improve function in this type of injury 3, which makes it necessary to initiate medical and therapeutic treatment 4 to reduce associated complications such as pain, edema, limitation of joint mobility, and loss of strength 5-7.
Proprioception is a sensory function with receptors in the skin, muscles, tendons, and joints that carry information to the central nervous system for conscious and unconscious control of position sense, joint movement, muscle strength, and balance 3,8,9 (Figure 1).
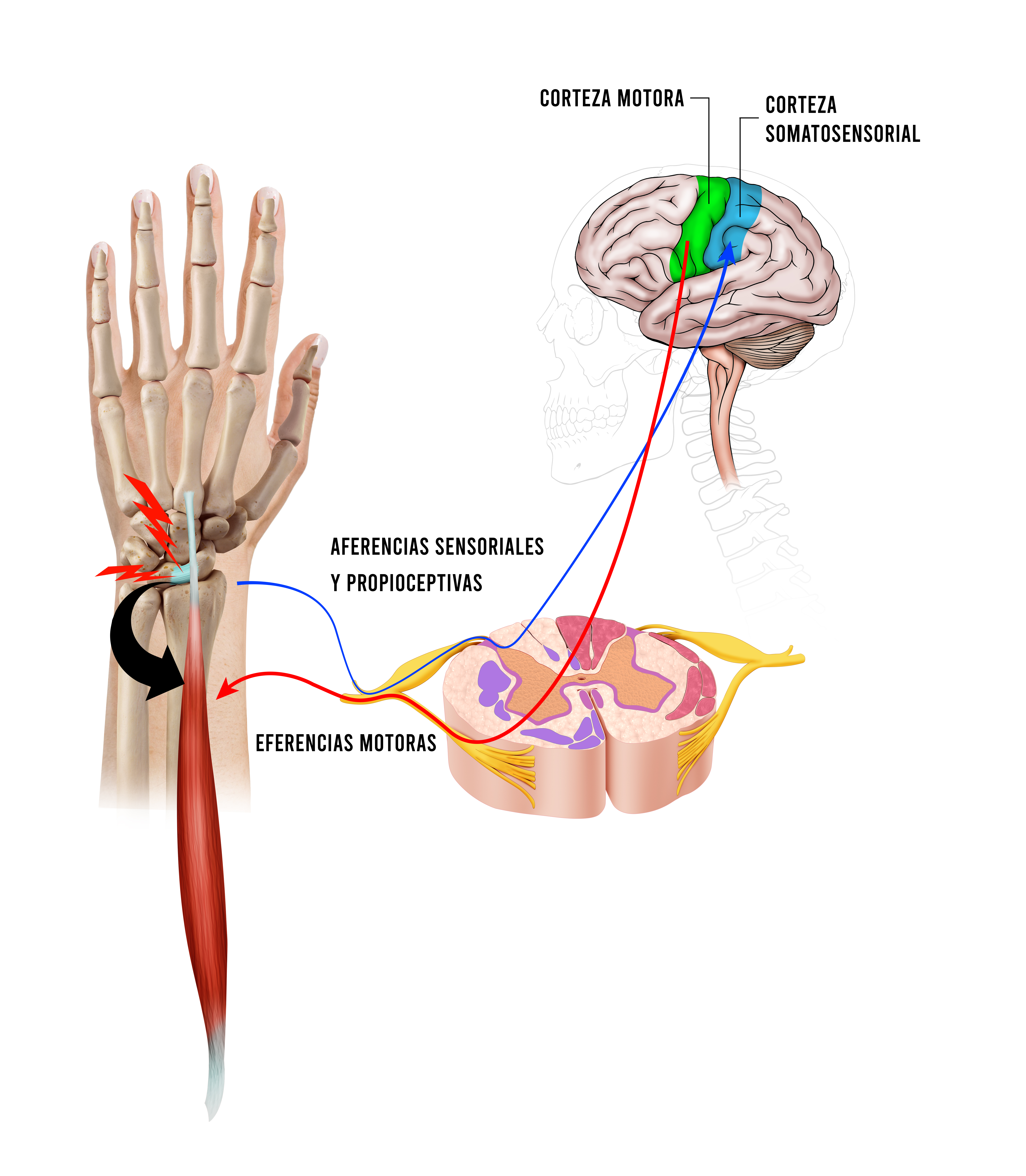
Figure 1
Principles of the wrist proprioceptive pathway. Certain anatomical and physiological criteria must be met for a joint to have a proprioceptive function. In the joints there are mechanoreceptors, which respond to stimuli (pressure, movement, and speed), sending afferent information through the dorsal horn of the spinal cord, information that will be processed in the somatosensory cortex and derived to the motor cortex to finally send the motor response that travels along the efferent pathway, reaching the anterior horn of the spinal cord, and from there the motor neurons will synapse at the neuromuscular junction to cause motor action.
Proprioceptive rehabilitation has been studied in lower limbs since the last century with positive results, and these have been extrapolated to upper limb rehabilitation. Only since 2009 has proprioceptive rehabilitation been investigated in the treatment of hand and wrist injuries of traumatic origin 9,10.
This review aims to identify proprioceptive rehabilitation strategies for recovering traumatic wrist injuries without neurological injury and their effects on pain, functionality, strength, joint mobility ranges, and edema.
Materials and Methods
A scoping review was carried out following the Prisma ScR 11 methodology for scoping review and the Joanna Briggs Institute Manual 12.
Inclusion and exclusion criteria
A search was conducted for scientific articles describing the use and outcomes of proprioceptive rehabilitation in adults with traumatic wrist injuries. Articles of clinical trials, cohort studies, and case studies were considered, and published in English, Spanish and Portuguese, with no restriction on publication date. The filters of title, abstract and content were applied, and the date of collection or search for information was made with a cut-off date of November 2023. The following research question (PICO) was established:
Participants: adult patients over 18 years of age with a diagnosis of posttraumatic wrist injury.
Interventions: proprioceptive rehabilitation in posttraumatic wrist injury.
Comparison: none, other intervention, or conventional management.
Results: pain, function, strength, joint mobility ranges and wrist edema.
Narrative articles, cross-sectional studies, editorials, and letters to the editor were excluded. Investigations with patients with neurological and adjacent joint lesions were excluded to better appreciate the effect of proprioceptive rehabilitation.
Search methods for study identification
The search process and identification of studies were performed using the following terms: Rehabilitation, Hand Injuries, Wrist Injuries, Proprioception, Physical Therapy Modalities, establishing the following combinations, (Rehabilitation) AND (Hand Injuries)) AND (Proprioception), rehabilitation [MeSH Terms]) AND (Wrist Injuries [MeSH Terms]) AND (Proprioception [MeSH Terms]), (Hand Injuries) AND (Proprioception), (Wrist Injuries) AND (Proprioception), ((Rehabilitation) AND (Proprioception)) AND (Wrist Joint). For the search of articles in Spanish and Portuguese, the translation of the term was performed with the thesaurus of structured and multilingual vocabulary, DeCS.
Searches were performed in PubMed, Embase, LILACS, PEDro, and Google Scholar databases.
After removing duplicate articles, two authors independently reviewed the selected articles to verify the study typology. Subsequently, the full text was reviewed to define the articles considered in the review. When there was a discrepancy between the authors, it was discussed, and consensus was reached with the third author. The following data were extracted from the selected articles: authors, country, study population, type of study, intervention performed, and main results, as well as the advantages and limitations of the study.
Results
A total of 1,085 articles were identified in the databases. There were no meta-analysis articles. We removed 436 duplicate articles. The authors excluded 526 articles by abstract. A total of 123 full-text articles were retrieved, of which 94 were excluded because they did not meet the population criteria, and 23 articles were excluded because the description of the proprioceptive intervention was not explicit. The analysis for the review was performed on six articles (Figure 2).
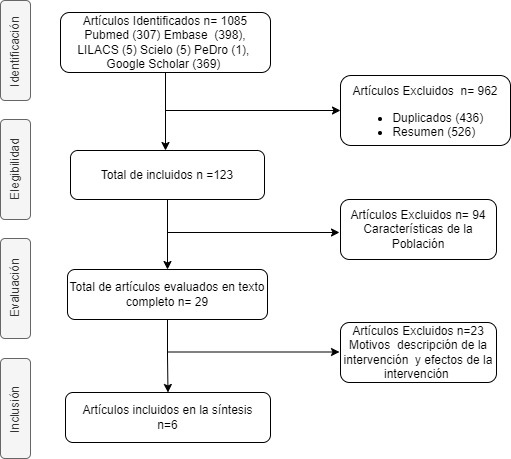
Figure 2
Flowchart of the review.
Characteristics of the included articles
The six selected articles included 125 subjects, with female gender and right-handed dominance predominating. The most frequent diagnoses were distal radius fracture and triangular fibrocartilage injury. Table 1 shows the characteristics of the population and the type of study.
Population, injury, and study type characteristics of the articles on proprioceptive wrist rehabilitation.

QuickDASH = Quick Disabilities of the Arm, Shoulder, and Hand; PRWE = patient-rated wrist evaluation JPS= joint position sense measurement
The articles describe the following techniques: graded motor imagery, sensorimotor home protocol, proprioceptive neuromuscular facilitation (PNF), motor work through dart coactivation, and mirror therapy.
In a randomized controlled trial in patients with surgically treated fractures of the distal third of the radius (19 patients), the graded motor imagery technique was used for eight weeks with image recognition and mirror therapy; it was compared with conventional therapy (14 patients), and progress was evaluated at the second, fifth and, eighth weeks with the visual analog pain scale (VAS), Jamar dynamometer, QuickDASH score (Quick Disabilities of the Arm, Shoulder, and Hand) and the Michigan Hand Questionnaire (MHQ). The intervention group showed improvement in pain intensity at rest and joint mobility ranges compared to the control group, and follow-up upper limb function was equivalent in the control and intervention groups.
The graded motor imagery technique was combined with sensorimotor strategies in patients with distal radius fractures (29 patients) compared to a conventional therapy group (31 patients). The progression of graded motor imagery is not detailed; sensory stimulation was performed by recognizing textures with eyes open and closed. The intervention was performed daily at home, and the evaluation was done in the third week and three months after the intervention. The sensory deficit was evaluated with sensorimotor tests with Semmes-Weinstein monofilaments, static and dynamic 2-point discrimination, vibration tests, temperature, Moberg detection in a timed manner, stereognosis, and proprioception tests 14. The investigation demonstrated sensory improvement; however, no differences were found in pain sensitivity, functionality, strength, or mobility.
In a case study, mirror therapy was the primary strategy for a patient with a triangular fibrocartilage lesion. This technique was used in the first weeks of intervention, promoting movement awareness exercises through the mirror; from the fifth week on, active muscle strengthening exercises were included with manual resistance in wrist stabilizing muscles and exercises with a gyroscope, which is a device that generates forces in multiple directions, thus stimulating proprioception. In the ninth week, active exercises with external resistance were started 17. After the intervention, significant changes were achieved in palmar pressure strength, pain, and functionality for the initial assessment.
The other three articles used the proprioceptive rehabilitation technique (PRT) 3,15,16. Chen et al., applied a protocol to a patient with a triangular fibrocartilage lesion consisting of dart throwing motion (DTM) work to organize manual restoration, adding closed kinetic chain exercises with attachments such as balls and generating weight load as well as bilateral upper limb patterns; then, weight and band work were added, and the load was organized according to the patient's response 15. The patient's pain and functional limitations decreased. Subsequently, he applied this protocol to ten patients with the same injury with similar results 16. In the last study, in 33 patients with fractures of the distal third of the radius (20 post-surgical and 13 without previous surgery), proprioceptive therapy was added to conventional rehabilitation without describing the technique or dose. They did not find significant changes concerning the control group 3.
Discussion
The term "proprioception" derives from the Latin "proprius" ("belonging to oneself") and "-ception" ("to perceive"). It allows to perceive body parts' location, movement, and action. For this purpose, it considers all central and peripheral structures; therefore, proprioceptive rehabilitation should integrate three principles: kinesthesia, joint position sense, and neuromuscular control, to reduce pain and edema, improve mobility, joint stability, and muscle strength, which translates into greater functionality of the involved segment. These principles are fundamental to optimizing the results of the interventional process. Kinesthesia, by focusing on movement awareness, improves control and coordination, strength, and stability. Work provides improved functionality and establishes a solid foundation for movement, thus enhancing functional capacity and reducing vulnerability to injury. Body awareness, essential for understanding position and movement in space, should be integrated into the rehabilitation process for this purpose as well; for its progression, the recovery times of the tissues involved should be considered 9,18.
Currently, several approaches work in isolation on the principles of proprioceptive rehabilitation; its applicability has been reported in joints such as the knee and ankle and neurological injuries 19,20. The risk associated with proprioceptive interventions is low due to the non-invasive nature of these techniques. In terms of economic efficiency, they are cost-effective compared to other therapeutic options since they do not require the purchase of specialized equipment, presenting an economical alternative to improve motor function and quality of life 8,9,21,22. These advantages of proprioceptive rehabilitation are similar when implemented for traumatic wrist injuries. However, there are limitations such as the number of subjects included in the studies, follow-up during treatment with low rigor and diversity of evaluation instruments.
Therefore, its clinical relevance and effectiveness are necessary for current and future practice in wrist rehabilitation, improving follow-up processes that include proprioceptive principles and integrating the neuromuscular, sensory, and musculoskeletal systems. Likewise, standardization processes should be generated that adjust the intensity and duration of the sessions according to the patient's condition and capabilities, thus reducing potential risk.
Other studies were excluded due to the lack of clarity regarding the interventions' dosage, frequency, and follow-up. The absence of detailed information on these critical elements makes it difficult to assess the effectiveness of the interventions studied effectiveness accurately 5,8,9,19-38.
Conclusions
Proprioceptive rehabilitation has demonstrated benefits in lower limb and hip or back recovery; however, rehabilitation of traumatic wrist injuries it is research pending. Well-described data and good-quality designs are needed to routinely propose this strategy in the clinic today.
References
Ferree S, van der Vliet QMJ, van Heijl M, Houwert RM, Leenen LPH, Hietbrink F. Fractures and dislocations of the hand in polytrauma patients: Incidence, injury pattern and functional outcome. Injury. 2017; 48(4): 930-935. Doi: 10.1016/j.injury.2017.02.034.
Luo Z, Zhu W, Jiang C, He W, Zuo H. Characteristics of distal radius fractures in east China-an observational cohort study of 1954 individual fractures. BMC Musculoskelet Disord. 2023; 24(1): 627. Doi: 10.1186/s12891-023-06742-x
Karagiannopoulos C, Sitler M, Michlovitz S, Tucker C, Tierney R. Responsiveness of the active wrist joint position sense test after distal radius fracture intervention. J Hand Ther. 2016; 29(4): 474-482. Doi: 10.1016/j.jht.2016.06.009
Luk MLM, Chan ACM, Cho JSY, Ng DMT, Lam ICY, Yau ELK, Miller T, Pang MYC. Predictors of chronic pain and disability in patients treated conservatively after distal radius fracture: a prospective cohort study. Int Orthop. 2023; 47(6): 1535-1543. Doi: 10.1007/s00264-023-05785-y
Lluch A, Salvà G, Esplugas M, Llusá M, Hagert E, Garcia-Elias M. El papel de la propiocepción y el control neuromuscular en las inestabilidades del carpo. Rev Iberoam Cir Mano. 2015; 43(1): 70-8. Doi: 10.1016/j.ricma.2015.06.012
Sánchez L, Osorio D, Quiñones Y. Guía de tratamiento terapéutico en fracturas de tercio distal de radio. Santiago de Cali: Universidad Santiago De Cali, Sello Editorial; 2022. 54 p. disponible https://libros.usc.edu.co/index.php/usc/catalog/book/452
Karagiannopoulos C, Michlovitz S. Rehabilitation strategies for wrist sensorimotor control impairment: From theory to practice. J Hand Ther. 2016; 29(2):154-65. Doi: 10.1016/j.jht.2015.12.003
Hagert E. Proprioception of the wrist joint: a review of current concepts and possible implications on the rehabilitation of the wrist. J Hand Ther. 2010; 23(1): 2-17. Doi: 10.1016/j.jht.2009.09.008
Hagert E, Susanne R. Wrist proprioception-An update on scientific insights and clinical implications in rehabilitation of the wrist. J Hand Ther. 2023; Doi: 10.1016/j.jht.2023.09.010
Ucuzoglu ME, Unver B, Sarac DC, Cilga G. Similar effects of two different external supports on wrist joint position sense in healthy subjects: A randomized clinical trial. Hand Surg Rehabil. 2020; 39(2):96-101. Doi: 10.1016/j.hansur.2019.11.006
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021; 372: n71. Doi: 10.1136/bmj.n71
Aromataris E, Munn Z (Editors). JBI Manual for Evidence Synthesis. JBI, 2020. Available from https://synthesismanual.jbi.global. Doi: 10.46658/JBIMES-20-01
Dilek B, Ayhan C, Yagci G, Yakut Y. Effectiveness of the graded motor imagery to improve hand function in patients with distal radius fracture: A randomized controlled trial. J Hand Ther. 2018; 31(1): 2-9.e1. Doi: 10.1016/j.jht.2017.09.004
Wollstein R, Harel H, Lavi I, Allon R, Michael D. Postoperative treatment of distal radius fractures using sensorimotor rehabilitation. J Wrist Surg. 2019; 8(1): 2-9. Doi: 10.1055/s-0038-1672151
Chen Z. A novel staged wrist sensorimotor rehabilitation program for a patient with triangular fibrocartilage complex injury: A case report. J Hand Ther. 2019; 32(4): 525-534. Doi: 10.1016/j.jht.2018.04.003
Chen Z. Clinical evaluation of a wrist sensorimotor rehabilitation program for triangular fibrocartilage complex injuries. Hand Ther. 2021; 26(4): 123-133. Doi: 10.1177/17589983211033313
Hincapie OL, Elkins JS, Vasquez-Welsh L. Proprioception retraining for a patient with chronic wrist pain secondary to ligament injury with no structural instability. J Hand Ther. 2016; 29(2): 183-90. Doi: 10.1016/j.jht.2016.03.008
Laskowski ER, Newcomer-Aney K, Smith J. Proprioception. Phys Med Rehabil Clin N Am. 2000; 11(2): 323-40.
Gurudut P, Godse AN. Effectiveness of graded motor imagery in subjects with frozen shoulder: a pilot randomized controlled trial. Korean J Pain. 2022; 35(2): 152-159. Doi: 10.3344/kjp.2022.35.2.152
Johnson S, Hall J, Barnett S, Draper M, Derbyshire G, Haynes L, et al. Using graded motor imagery for complex regional pain syndrome in clinical practice: failure to improve pain. Eur J Pain. 2012; 16(4): 550-61. Doi: 10.1002/j.1532-2149.2011.00064.x
Hagert E, Persson JK, Werner M, Ljung BO. Evidence of wrist proprioceptive reflexes elicited after stimulation of the scapholunate interosseous ligament. J Hand Surg Am. 2009; 34(4): 642-51. Doi: 10.1016/j.jhsa.2008.12.001
León-López MM, García-Elías M, Salvà-Coll G, Llusá-Perez M, Lluch-Bergadà A. Control muscular de la inestabilidad escafolunar. Estudio experimental. Rev Esp Cir Ortopédica Traumatol. 2013;57(2):11-8. Doi: 10.1016/j.recot.2013.10.002
Baldursdottir B, Whitney SL, Ramel A, Jonsson PV, Mogensen B, Petersen H, et al. Multi-sensory training and wrist fractures: a randomized, controlled trial. Aging Clin Exp Res. 2020; 32(1): 29-40. Doi: 10.1007/s40520-019-01143-4
Byl N, Wilson F, Merzenich M, Melnick M, Scott P, Oakes A, McKenzie A. Sensory dysfunction associated with repetitive strain injuries of tendinitis and focal hand dystonia: a comparative study. J Orthop Sports Phys Ther. 1996; 23(4): 234-44. Doi: 10.2519/jospt.1996.23.4.234
Khamwong P, Pirunsan U, Paungmali A. A prophylactic effect of proprioceptive neuromuscular facilitation (PNF) stretching on symptoms of muscle damage induced by eccentric exercise of the wrist extensors. J Bodyw Mov Ther. 2011; 15(4):507-16 Doi: 10.1016/j.jbmt.2010.07.006
Marini F, Ferrantino M, Zenzeri J. Proprioceptive identification of joint position versus kinaesthetic movement reproduction. Hum Mov Sci. 2018; 62: 1-13. Doi: 10.1016/j.humov.2018.08.006
Gay A, Parratte S, Salazard B, Guinard D, Pham T, Legré R, et al. Proprioceptive feedback enhancement induced by vibratory stimulation in complex regional pain syndrome type I: an open comparative pilot study in 11 patients. Joint Bone Spine. 2007; 74(5):461-6 Doi: 10.1016/j.jbspin.2006.10.010
Cantero-Téllez R, Medina Porqueres I. Practical exercises for thumb proprioception. J Hand Ther. 2021; 34(3): 488-492. Doi: 10.1016/j.jht.2020.03.005
Wolff AL, Wolfe SW. Rehabilitation for scapholunate injury: Application of scientific and clinical evidence to practice. J Hand Ther. 2016; 29(2): 146-53. Doi: 10.1016/j.jht.2016.03.010
Hartzell TL, Rubinstein R, Herman M. Therapeutic modalities--an updated review for the hand surgeon. J Hand Surg Am. 2012; 37(3): 597-621. Doi: 10.1016/j.jhsa.2011.12.042
Guisasola LE, Carratalá BV, Calduch SF, Lucas GF. El papel de la rehabilitación tras las reparaciones de las inestabilidades de muñeca. Rev Iberoam Cir Mano. 2016; 44(2): 131-42. Doi: :10.1016/j.ricma.2016.09.001
Valdes K, Naughton N, Algar L. Sensorimotor interventions and assessments for the hand and wrist: a scoping review. J Hand Ther. 2014; 27(4): 272-85; Doi: 10.1016/j.jht.2014.07.002
Miyahara Y, Naito H, Ogura Y, Katamoto S, Aoki J. Effects of proprioceptive neuromuscular facilitation stretching and static stretching on maximal voluntary contraction. J Strength Cond Res. 2013; 27(1): 195-201. Doi: 10.1519/JSC.0b013e3182510856
Pelletier R, Paquette É, Bourbonnais D, Higgins J, Harris PG, Danino MA. Bilateral sensory and motor as well as cognitive differences between persons with and without musculoskeletal disorders of the wrist and hand. Musculoskelet Sci Pract. 2019; 44: 102058. Doi: 10.1016/j.msksp.2019.102058
Babaei-Mobarakeh M, Letafatkar A, Barati AH, Khosrokiani Z. Effects of eight-week »,» ®,® §,§ ­, ¹,¹ ²,² ³,³ ß,ß Þ,Þ þ,þ ×,× Ú,Ú ú,ú Û,Û û,û Ù,Ù ù,ù ¨,¨ Ü,Ü ü,ü Ý,Ý ý,ý ¥,¥ ÿ,ÿ ¶,¶ gyroscopic device »,» ®,® §,§ ­, ¹,¹ ²,² ³,³ ß,ß Þ,Þ þ,þ ×,× Ú,Ú ú,ú Û,Û û,û Ù,Ù ù,ù ¨,¨ Ü,Ü ü,ü Ý,Ý ý,ý ¥,¥ ÿ,ÿ ¶,¶ mediated resistance training exercise on participants with impingement syndrome or tennis elbow. J Bodyw Mov Ther. 2018; 22(4): 1013-1021. Doi: 10.1016/j.jbmt.2017.12.002
Clark NC, Röijezon U, Treleaven J. Proprioception in musculoskeletal rehabilitation. Part 2: Clinical assessment and intervention. Man Ther. 2015; 20(3): 378-87. Doi: 10.1016/j.math.2015.01.009
McCormick K, Zalucki N, Hudson M, Moseley GL. Faulty proprioceptive information disrupts motor imagery: an experimental study. Aust J Physiother. 2007; 53(1): 41-5. Doi: 10.1016/s0004-9514(07)70060-0
Sharman MJ, Cresswell AG, Riek S. Proprioceptive neuromuscular facilitation stretching : mechanisms and clinical implications. Sports Med. 2006; 36(11): 929-39. Doi: 10.2165/00007256-200636110-00002
Notes
