Ciências Sociais
Consumption, risk factors, and the impact of psychoactive substances in road transport by professional drivers: a review
Consumption, risk factors, and the impact of psychoactive substances in road transport by professional drivers: a review
Acta Scientiarum. Human and Social Sciences, vol. 43, núm. 2, e58057, 2021
Universidade Estadual de Maringá

Esta obra está bajo una Licencia Creative Commons Atribución 4.0 Internacional.
Recepción: 03 Marzo 2021
Aprobación: 31 Mayo 2021
Abstract: Traffic accidents are a serious public health problem, especially in developing countries. Driving under the influence of psychoactive substances, such as illicit drugs, can significantly increase the risk of motor vehicle accidents. This fact potentiates the probability of serious traffic accidents occurring, making it necessary to combat them with seriousness and urgency. Many road traffic crashes are related to sleepiness and/or fatigue. In addition to long driving hours, important contributors to fatigue among professional drivers are insufficient night-time sleep and insufficient rest breaks. Research data on the topic show that several psychoactive drugs alter the motor and cognitive capacity of users, however, most of these studies pointed out such outcomes based on the prevalence of illicit drug use in professional hospitalized drivers. Despite the existence of laws against driving doped, the effectiveness of these laws in controlling the problem is questionable. For this research, the study was conducted to highlight and discuss, by a descriptive review, the consumption of psychoactive substances among professional drivers, and the role of working conditions in the prediction of such use. Data about drug use were obtained in this review aims to contribute for the development of preventive measures, especially public policies on the risks of driving while under the influence of psychoactive drugs.
Keywords: working conditions, risk factors, drug addiction, human rights, public health.
Resumo:
. Os acidentes de trânsito são um grave problema de saúde pública, principalmente nos países em desenvolvimento. Dirigir sob a influência de substâncias psicoativas, como drogas ilícitas, pode aumentar significativamente o risco de acidentes com veículos motorizados. Esse fato potencializa a probabilidade de ocorrência de acidentes graves de trânsito, sendo necessário combatê-los com seriedade e urgência. Muitos acidentes de trânsito estão relacionados à sonolência e/ou fadiga. Além das longas horas de condução, contribuintes importantes para a fadiga entre os motoristas profissionais são o sono noturno e as pausas para descanso insuficientes. Dados de pesquisas sobre o tema mostram que diversas drogas psicoativas alteram a capacidade motora e cognitiva dos usuários, porém, a maioria desses estudos apontou tais desfechos a partir da prevalência do uso de drogas ilícitas em motoristas profissionais hospitalizados. Apesar da existência de leis contra dirigir dopado, a eficácia dessas leis no controle do problema é questionável. Para esta pesquisa, o estudo foi realizado com o objetivo de evidenciar e discutir, por meio de revisão descritiva, o consumo de substâncias psicoativas entre os motoristas profissionais e o papel das condições de trabalho na predição desse uso. Os dados sobre o uso de drogas foram obtidos nesta revisão busca contribuir para o desenvolvimento de medidas preventivas, sobretudo políticas públicas sobre os riscos de dirigir sob o efeito de drogas psicoativas.
Palavras-chave: condições de trabalho, fatores de risco, dependência de drogas, direitos humanos, saúde pública.
Introduction
Long-distance professional drivers are considered a special interest group in terms of drug driving research and policy due to high rates of use, the involvement of drugs in truck accidents, and the link between drug use and work-related fatigue (Apostolopoulos, Sönmez, Shattell, Gonzales, & Fehrenbacher, 2013). Whilst drink driving has long been considered a social problem worthy of substantial research and campaign efforts, it is only relatively recently that increasing attention has been given to the issue of drug driving. Statistics are emerging which demonstrate the extent of the problem of drug driving including the types of drugs used whilst driving, and how these affect performances (Riva, Marchett, Giupponi, & Mosconi, 2010).
To avoid drowsiness and tiredness caused by work, many professional drivers use illicit drugs (cannabinoids, stimulants, and amphetamines) and psychoactive drugs belonging to the classes of antihistamines, muscle relaxants, benzodiazepines, and anorexigenic, which leads them to stay awake for many hours straight (Knauth, Pilecco, Leal, Seffner, & Teixeira, 2012). Additionally, they usually work in stressful conditions that favour unhealthy lifestyles and medical disorders. Their overall health, and especially their mental health, is very often worse than the general population because of long driving shifts, disrupted sleep patterns, chronic fatigue, compelling service duties, delivery urgency, job strain, low rewards, stress, lonely life, distance from the family, and unsystematic medical control (Thiese et al., 2015). The physical dependence is developed during the use of drugs, due to the phenomenon of tolerance, which is characterized by a decrease in the effect of the drug resulting from its continuous use, leading the user to use larger doses to obtain the effect of before. With the interruption of the substance may occur signs and physical symptoms (abstinence syndrome), usually contrary to the effects produced by drugs (Ahlm, Bjornstig, & Ostrom, 2009).
Data from the literature explicit some studies in different countries the influence of working conditions on the use of psychoactive substances by professional drivers or pointed the main cause for road accidents, in general traumatic (Anderson et al., 2012). There is considerable evidence of high rates of both illicit and licit substance use among professional drivers both in Brazil and internationally, which generate a consensus that drug-taking for professional drivers is a means of alleviating work-related fatigue (Gjerde et al., 2014).
Whether or not this is the case, this behaviour has been linked to accident culpability and consequently, several legislative measures to combat the problem have been enforced. A detailed scenario would also help to identify preventive strategies for the health and well-being of professional drivers and develop countermeasures to control the potential risks inherent in this group.
For this research, the study was conducted to highlight and discuss, by a descriptive review, the consumption of psychoactive substances among professional drivers, and the role of working conditions in the prediction of such use.
Literature review
In general, the drugs used by professional drivers have their primary effects on the brain, and it is through these effects that physiological and psychological functions are modified. A fundamental tenet of pharmacology states that drug molecules exert some chemical influence on one or more constituents of cells to produce a pharmacological response. To produce its effects, a drug must be present in adequate concentrations at its site(s) of action (Nascimento, Nascimento, & Silva, 2007). This is largely dependent on the amount of drug administered initially and the extent and rate of the processes by which the body responds to the drug (the pharmacokinetics). The first factor relates to the route of the administration itself. A drug can be administered in several different ways: orally, by injection, by inhalation, or by application to mucous membranes such as the mouth and nose. The chosen route will affect the speed with which symptoms appear and their duration of action. For example, a drug that is injected directly into the bloodstream will have a more rapid onset of action than a drug that is taken orally, although the duration of action will be shorter, that is, the effects will not persist as long. If a drug is administered orally, it does not move immediately to the brain but is eventually absorbed into the bloodstream. Thus, the time taken for the drug to produce its effects is also dependent on the rate of absorption. The drug is then distributed throughout the body via the bloodstream until it reaches the brain. This is a passive process and the amount of the drug that reaches the brain will determine the subsequent effects. All drugs have a limited time-course of action, so eventually, the drug is eliminated from the body. This occurs by two main processes: biotransformation, which involves the chemical transformation of the drug into a different compound or metabolite, and excretion of the drug, primarily via the renal system (Gjerde et al., 2012).
Alcohol
Alcohol is a depressant that acts on the central nervous system. Although it has no known specific receptor system, it has been found to affect a variety of neurotransmitters. Alcohol is administered orally and is absorbed in the stomach and small intestine. It is evenly distributed throughout the body and is largely metabolized in the liver by the enzyme alcohol dehydrogenase. Above extremely low concentrations, the rate of metabolism of alcohol is not believed to be dose dependent. Thus, a fall in blood alcohol concentration occurs at a linear rate over time (Mir, Khan, Ahmed, & Abdul Razzak, 2012). Alcohol can produce adverse effects on driving performance in several ways. Some impairment in psychomotor performance occurs at relatively low blood alcohol concentration but will be substantially higher at concentrations that induce sedation. There are also behavioural changes such as risk taking, disinhibition and impulsiveness that are produced by alcohol. Any such change may result in impaired driving performance.
Marijuana
Marijuana is derived from the hemp plant Cannabis sativa. The principal cannabinoids are cannabidiol, cannabinol and Δ9tetrahydrocannabinol (THC). The acute effects of marijuana include feelings of euphoria, relaxation and sedation, some loss of inhibitions, spatial and temporal distortions and increased heart rate and appetite (Labat et al., 2008). There is also evidence of confusion, loss of concentration and general impairment of cognitive and motor skills. Higher concentrations can lead to hallucinations, delusions, anxiety, disorientation, and paranoia, although these reactions are infrequent and tend to be associated with long-term use and high doses (Laraqui et al., 2011). This changed with the finding that chronic administration of high doses of THC results in the development of tolerance to its cardiovascular effects and a reduction in the subjective 'high' experienced by marijuana users. There is also evidence that abrupt cessation of marijuana produces withdrawal, with symptoms including irritability, insomnia, restlessness, and a decrease in appetite (Okpataku, 2015).
Benzodiazepines
The benzodiazepine class includes many individual drugs. Diazepam ('Valium') was at one time the highest selling pharmaceutical drug in the world and other commonly prescribed drugs within this group include oxazepam, nitrazepam and temazepam (Leyton et al., 2012).
Benzodiazepines are administered orally and are absorbed into the blood from the gastrointestinal tract. They are highly fat-soluble and are readily distributed throughout the body. Prolonged and regular use of benzodiazepines can lead to the development of tolerance. This has implications when assessing potential drug-induced impairment. Persons who have been taking the drug for an extended period of time may become less sensitive to its effects and consequently their driving may not be impaired, even at high doses (Wendler, Busato, & Miyoshi, 2003; Oliveira et al., 2015). Crouch et al. (1993) report that tolerance to the effects of diazepam on psychomotor performance occurs very quickly, and it is difficult to correlate plasma concentrations of the drug with impairment. In addition, persons using the drug to treat a specific condition may be less impaired after taking it.
Stimulants
The stimulants act on neurotransmitters in the central nervous system by inhibiting the re-uptake of noradrenaline, serotonin, and dopamine, and they also increase neurotransmitter release (Mabbott & Hartley, 1999). Several 'designer drugs' have been developed from modifications of the amphetamine molecule. The most common derivative of amphetamine currently used for recreational purposes was synthesised in 1914. Methylenedioxymethamphetamine (MDMA), known commonly as 'Ecstasy' may produce hallucinations in some users, but is like the parent compound in its central stimulatory effects (Mongkolsirichaikul, Mokkhavesa, & Ratanabanangkoon, 1988). Cocaine is the main active ingredient of the plant Erythroxylon coca, although synthetic derivatives are also available. Is generally available in powder form, which is administered orally or intranasally, or in crystalline form (known as 'crack'), which is vaporised and then inhaled.
The main effect of stimulants on driving performance may be an improvement through reversal of fatigue. However, impairment of driving can also come about for several reasons. For example, exceedingly high doses may induce a state that leads to erratic driving behaviour. Prolonged use of stimulants may also result in sleep deprivation and rebound increases in fatigue that could produce marked impairment in driving performance, with drivers potentially falling asleep at the wheel (Mieczkowski, 2010).
Methodology
As a method, the research took place through a systematic review, which is a way of synthesizing the information available in a given moment, about a specific problem, in an objective and reproducible way, using the scientific method. Thus, an ordered set of criteria was adopted that determine the scientificity of a systematic literature review, starting with the construction of a protocol, whose function was to guarantee the rigour of the research process. For this, the protocol had the following components: review question, inclusion and exclusion criteria, strategies for searching the universe of research, guidance for the selection of material, analysis, and synthesis of data. Therefore, the review is guided by the following questions What is the consumption of psychoactive substances by professional drivers in road transport and the associated risk factors?
Systematic review
The current systematic review of the literature with meta-analysis and meta-regression is reported according to the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines (Liberati et al., 2009). Studies were selected if they were original and with quantitative results specifically on the use of psychoactive substances by professional truck drivers. No restrictions were made regarding language and year of publication.
Search strategies and information sources
The studies were identified by consulting the following scholarly databases: Virtual Health Library, Brazil (MEDLINE, LILACS, SciELO, IBECS, and BDENF), PubMed, PsycNET and Cochrane. The MEDLINE and PubMed search was carried out by combining the following keywords in the title or abstract: ‘truck’, ‘lorry’, ‘lorries’, ‘heavy vehicle’, ‘heavy transport’, ‘motorist’, ‘driver’, ‘conductor’, ‘worker’, ‘job’, ‘professional’, ‘drug’, ‘stimulant’, ‘substance’, ‘medicine’, ‘medication’, ‘psychoactive’, ‘amphetamine’, ‘cocaine’, ‘marijuana’ and ‘crack’ (the search strategy can be found in the online supplemental material). For the LILACS, SciELO, IBECS, BDENF, and PsycNET database searches, the terms ‘truck’, ‘truck drivers’ or ‘load transport’ were used, while in the Cochrane database the studies selected included the terms ‘truck’, ‘lorry’, ‘lorries’, ‘heavy vehicle’ or ‘heavy transport’. The search strategy was based on language and syntax adequate to each database.
Methodological appraisal of studies quality
Inclusion criteria were based on the PECO criteria (Morgan, Whaley, Thayer, & Schünemann, 2018). Articles were included if: 1) focused on professional drivers (P = truck-drivers); 2) investigating drug consumption (E = exposure to abuse substances); 3) stratifying according to parameters such as age, gender, marital status, experience years, mean distance travelled (per trip), work-load, night-shift or educational level, in terms of primary schooling level (C = any comparison); and 4) reporting prevalence rate of drug consumption (O = drug consumption rate). Concerning the study design, articles were selected if devised as prevalence studies. Articles were excluded if they did not meet the PECO criteria mentioned above and if designed as editorials, notes, letters, abstracts, case reports, comments, duplicate articles, and studies of obscure or dubious methodology.
An Excel spreadsheet was structured (https://products.office.com/) containing the following terms: authors, year of publication, country of study, study design/methodology, number of people investigated, objectives, population studied, and main results.
The methodological quality of observational studies was assessed according to STROBE (Strengthening the reporting of observational studies in epidemiology) statement (Vandenbroucke et al., 2007), consisting of a checklist of 22 items that should be addressed in articles. The version translated and validated for use in Brazil (Malta, Cardoso, Bastos, Magnanini, & Silva, 2010) establishes article quality categories. Articles that meet at least 80% of the items are classified as category ‘A’ (Vandenbroucke et al., 2007; Malta et al., 2010). Qualitative studies were assessed using the Standards for Reporting Qualitative Research (SRQR) (O’Brien, Harris, Beckman, Reed, & Cook, 2014). Studies that used both quantitative and qualitative methodologies were assessed using both instruments and included if they met at least 80% or higher of the items of one of the instruments. One independent reviewer assessed methodological quality and two reviewers evaluated thematic eligibility.
Results and discussion
Investigations were carried out between 1983 and 2020. The searches yielded 11,009 articles, 2,671 of which were excluded because they were duplicates. A total of 8,338 articles were excluded after the analysis of the titles and abstracts because they failed to meet the study eligibility criteria. The full texts of the remaining citations were then examined, resulting in the exclusion of 216 articles because they failed to meet the study inclusion criteria. The remaining articles were then assessed against the STROBE and SRQR checklists. A total of 183 publications were excluded because they failed to meet at least 80% of the items, resulting in a final sample of 33 articles (Figure 1).
In Figure 2 is shown an instrument that synthesize the main data extracted from each study in a descriptive way, containing the following components: the distribution of works according to the year of publication, the geographic region where they were carried out, the methodological path, sample, and objective.
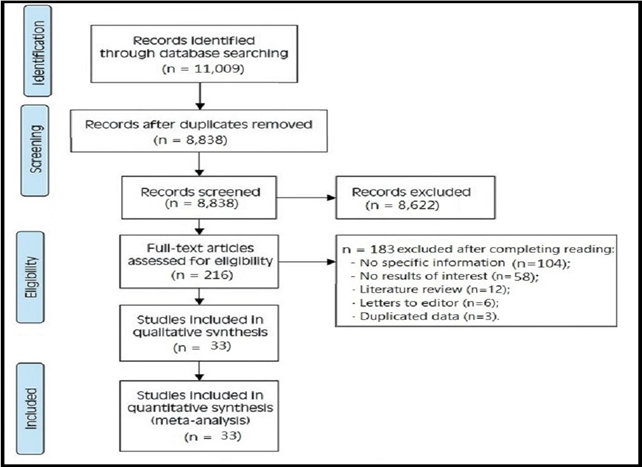
Figure 1. Flow diagram for selecting papers included in the present systematic review (Research, (2021).
The main substances consumed or identified in the studies were alcohol (n=23), marijuana (n=18), amphetamines (n=14), and cocaine (n=12). The average frequency of self-reported alcohol consumption was 54.3%, ranging from a minimum of 9.9% (Pakistan) (Mir et al., 2012) to a maximum of 91.0% (Brazil) (Nascimento et al., 2007). The identification of alcohol in biological samples was, on average, 3.6% (Gjerde et al., 2012), and a maximum of 12.5% (USA) (Crouch et al., 1993). The average frequency of self-reported amphetamine intake was 29.5%, ranging from 0.9% (Italy) (Riva et al., 2010) to 58.0% (Brazil) (Oliveira et al., 2015).
Of all eligible studies, one was conducted in countries with large land areas, Brazil (n=20), the USA (n=3), and Australia (n=2) being those with the highest number of investigations. Most papers were published starting in the year 2003 (n=28). About 84.8% of the studies only researched male drivers. Among the 33 investigations, 18 assessed the intake of substances only through truckers’ self-reporting, 10 only through biological samples, and two through both (Leyton et al., 2012; Yonamine et al., 2013).
Knauth et al. (2012) pointed that by using multiple regression analysis to identify factors associated with the use of amphetamines, found that younger age, higher income, longer trips, and alcohol consumption were positively associated with self-reported amphetamine intake, even after controlling for socio-demographic characteristics and religion. Williamson (2007) found that, in Australia, the use of stimulating medication was associated with less driver experience, work in medium and small-sized companies, income below levels defined by union agreements, productivity-based earnings and fatigue.
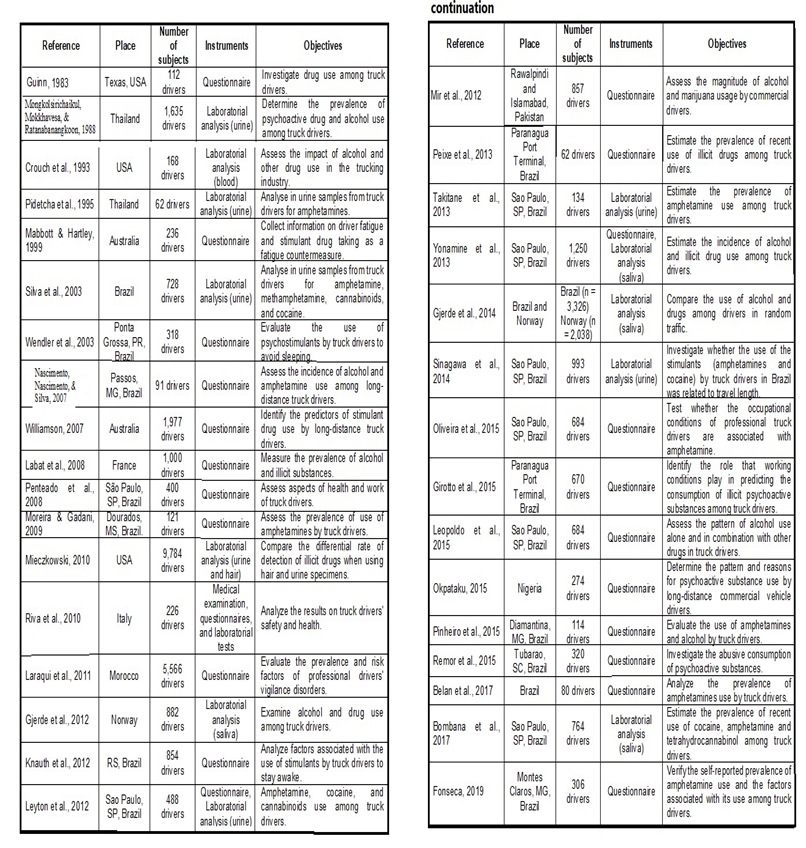
Figure 2. Critical appraisal of studies on the consumption of psychotropic substances among truck drivers (Research, 2021).
Traffic-related issues influence society, whether it be the movement of people, products, or services. We live in a time when access to places and goods has a relevant value for social, economic, and personal development. With this importance of road transport, the occurrence of accidents among those involved is enhanced, with traffic accidents being one of the main causes of truck driver deaths. Studies on psychoactive substance use biological samples are shown in Table 1, and on a self-reported psychoactive substance in Table 2.
Amphetamine, marijuana, and cocaine self-reported intake had frequencies of 68.75, 29.9, and 5.3%, respectively. In the biological samples, averages of 11.15% for amphetamine, 1.87% for marijuana, and 1.31% for cocaine were found. Amphetamine use ranged from 0.14% (Mieczkowski, 2010) to 82.5% (Mongkolsirichaikul et al., 1988). Marijuana use ranged from 0.21% (Mieczkowski, 2010) to 12.5% (Crouch et al., 1993), while cocaine ranged from 0.27% (Silva et al., 2003; Mieczkowski, 2010) to 8.3% (Crouch et al., 1993). Besides these substances, others were occasionally analyzed, such as opioids (Crouch et al., 1993; Labat et al., 2008; Mieczkowski, 2010; Riva et al., 2010), phentermine (Mabbott & Hartley, 1999), codeine (Crouch et al., 1993); Gjerde et al., 2012), pure coffee and energy drinks (Penteado, Gonçalves, Costa, & Marques, 2008; Leopoldo, Leyton, & Oliveira, 2015), and benzodiazepines (Labat et al., 2008).
| Study | Amphetamine Methamphetamine | Cannabinoids | Cocaine metabolites | Alcohol |
| Mongkolsirichaikul et al. (1988) | 82.5%*** | NA | NA | NA |
| Crouch et al. (1993) | 7.1%** | 12.5%** | 8.3%** | 12.5%** |
| Pidetcha et al. (1995) | 25.8%*** | NA | NA | NA |
| Silva, Greve, Yonamine, & Leyton (2003) | 4.8%*** | 0.27%*** | 0.27%*** | NA |
| Mieczkowski (2010) | 0.14%* | 0.21%*** | 0.27%*** | NA |
| Riva et al. (2010) | NA | 0.44%*** | 0.44%***NA | NA |
| Gjerde et al. (2012) | 0.2%**** | 0.7%**** | 0.8%**** | 0.1% |
| Leyton et al. (2012) | 6.0%*** | 1.1%*** | 2.2%*** | NA |
| Takitane et al. (2014) | 10.8%*** | NA | NA | NA |
| Yonamine et al. (2013) | 0.6%**** | 0.4%**** | 0.6%**** | 1.4%**** |
| Gjerde et al. (2014) | 1%****(Brazil) 0.3%****(Norway) | 0.5%****(Brazil) 1%****(Norway) | 1%****(Brazil) 0.3%****(Norway) | 2.7%****(Brazil) 0.2%****(Norway) |
| Sinagawa et al. (2014) | 5.7%*** | 0.7%*** | 0.3%*** | NA |
| Bombana et al. (2017) | NA | 2.75%**** | NA | NA |
| Study | Description of substances |
| Guinn (1983) | Drug use while trucking: 80.4% |
| Mabbott & Hartley (1999) | Illicit and prescribed stimulant: 8.9%, Illicit or prescribed stimulant: 11.9%, Over-the-counter stimulants: 6.8% |
| Wendler et al. (2003) | Medicines without medical control: 65.39% |
| Nascimento et al. (2007) | Alcohol: 91.0%; Amphetamine: 66.0% |
| Williamson (2007) | Stimulant drug use: 31.1% |
| Labat et al. (2008) | Benzodiazepines: 0.4%, Buprenorphine: 1.8%, Opiates: 4.1%, Methadone: 0.5% |
| Penteado et al. (2008) | Alcohol: 43.5%, Stimulants: 7.5%, Coffee: 85.75%, Energy drinks: 19.5%, Illicit drugs: 2.0% |
| Moreira & Gadani (2009) | Amphetamine: 65.0% |
| Riva et al. (2010) | Alcohol: 49.2%, Amphetamine: 0.9%, Marijuana: 15.9%, Cocaine: 5.3% |
| Laraqui et al. (2011) | Alcohol: 11.8%, Marijuana: 12.0%, Coffee: 71.8%, Psychotropic medicines: 3.9% |
| Leyton et al. (2012) | Amphetamine: 16.6% |
| Knauth et al. (2012) | Alcohol: 73.1%, Amphetamine: 12.4%, Caffeine: 14.8%, Guarana powder: 2.7%, Energy drinks: 3.9%, Cocaine: 0.4% |
| Mir et al. (2012) | Alcohol: 9.9%, Marijuana: 29.9% |
| Peixe, Almeida, Girotto, Andrade, & Mesas (2013) | Cocaine: 4.8%, Amphetamine: 1.6% |
| Yonamine et al. (2013) | Alcohol: 25.9%, Drugs: 1.2% |
| Oliveira et al. (2015) | Amphetamine: 29.0% |
| Girotto, Andrade, Mesas, González, & Guidoni (2015) | Amphetamine: 10.9% |
| Leopoldo et al. (2015) | Alcohol: 67.3% (9.2% were at risk of developing alcohol addiction), Heavy drinking: 34.6%, Binge drinking: 26%, Multiple drug use: 54.6% (alcohol with tobacco and energy drinks). |
| Okpataku (2015) | Alcohol: 26.6%, Cannabis: 9.4%, Opioids: 4.3%, Anxiolytics: 2.1%, Solvents: 1.1%, Cocaine: 0.3%, Caffeinated substances: 51.4% |
| Pinheiro, Muniz, Silva, Resill, & Filho (2015) | Amphetamine: 15.0%, Alcohol: 2,0% |
| Remor et al. (2015) | Amphetamine: 48.8% |
| Belan et al. (2017) | Amphetamine: 68.75% |
| Fonseca, Viana, Souza, & Rossi-Barbosa (2019) | Amphetamine: 22.2% |
The use of amphetamines was associated with driving during the night shift and with longer time in the profession (Nascimento et al., 2007). Additional identified data showed that drug intake was associated with male sex (Gjerde et al., 2012), inadequate work, stealing merchandise, failure to report the damage to goods transported, driving on interstate routes, and short or long sleep times (Mabbott & Hartley, 1999), age less than 35 years (Leyton et al., 2012).
Table 3 presents data on the acquisition, frequency, and problems regarding the use of amphetamines among professional drivers, identified within this review by consolidating data of Table 1 and Table 2. It was found that most use when they start to feel sleepy; meantime, even knowing the problems regarding the use (arrhythmia, dizziness, headache, trembling of limbs, chest pain), forced by the characteristics of their jobs, they consume.

Source: Research data (2021)
The main effects caused by amphetamine lead to dependence and forced behaviour to ingest the drug (Remor et al., 2015; Belan et al., 2017). Besides, there are contraindications for patients with hypertension, hyperthyroidism, or glaucoma (Belan et al., 2017). It is important to detach that the main reason for lethal accidents of truck drivers on the roads is related to the fact that they sleep at the wheel since they are obliged to use these substances to deliver the cargoes within the established deadline (Fonseca et al., 2019).
Data found by Fonseca (2019) are more consistent and will be more highlighted. The average age of the 306 respondents was 41 years old, (SD ± 10.5) with a minimum age of 22 and a maximum age of 77 years. The most prevalent age group was from 30 to 39 years old. Most have elementary education, but it is observed that there are individuals with higher education in this profession. Most of them work between 11 and 14 hours and have been working for less than 10 years as truck drivers, with 22.9% reporting working between six and ten years.
Studies carried out in several countries have shown that the number of deaths and injuries is increasing, due to car accidents that occurred with drivers of different ages, under the influence of drugs that are not allowed and sometimes combined with alcohol (Guinn, 1983; Nascimento et al., 2007; Riva et al., 2010; Knauth et al., 2012; Leopoldo et al., 2015). According to Okpataku (2015), injury and deaths due to road traffic accidents are a major public health problem in developing countries where more than 85% of all deaths and 90% of disability-adjusted life years were lost from road traffic injuries.
Despite the important findings, the results of the present study must be interpreted considering some limitations. One aspect to be highlighted concerns the detection of the use of amphetamines when obtained through self-report. The response rate may have been underestimated as to the actual number of users. Another limitation relates to the fact of not having researched on other illegal drugs, such as crack.
Final considerations
Because of the data presented in this article, it is worrying that drivers are encouraged to use indiscriminate substances that may artificially increase the period of work, for the most part, to beat the competition and meet goals. The longer the time spent driving, the greater the profits obtained with transportation.
Testimonials given by professional drivers reveal that the sensation caused after the consumption of amphetamines is a vitality, as if the individual woke up from a long night of sleep, making the driver willing to face a long workday; but besides that, there are also hallucinations. Normally, the health risks are not considered, as well as the dangers that a driver under the influence of drugs poses to other road users.
The combination of psychoactive substances and traffic must be combated seriously and urgently. After the establishment of adequate laws, the next step, the main combat mechanism, is the routine inspection by responsible institutions. For this, it becomes essential to operationalize the use of instruments capable of providing immediate and practical detection of the use of psychoactive substances that cause addiction. Some forms of detection exist and are efficient, such as those treated throughout this work, such as laboratory tests using biological agents such as hair, blood, urine or sweat. It can also be detected by analyzing the symptoms and signs performed by an expert doctor. However, after reflection, it is concluded that the most effective and efficient form of inspection would be using saliva test equipment, which is an instrument that has the convenience of being able to be used at the site of the inspection, in addition to having a low-invasive examination technique with results fast and reliable.
The life and health of drivers, as well as of all traffic participants, must be protected and preserved. This must be the foundation of public policies and the implementation of laws, providing the right to safer traffic for all citizens.
Acknowledgement
The study was funded by the National Council for Scientific and Technological Development (CNPq).
References
Ahlm, K., Bjornstig, U., & Ostrom, M. (2009). Alcohol and drugs in fatally and non-fatally injured motor vehicle drivers in northern Sweden. Accident Analysis and Prevention, 41(1), 129-136. DOI: https://doi.org/10.1016/j.aap.2008.10.002
Anderson, J. E., Govada, M., Steffen, T. K., Thorne, C. P., Varvarigou, V., Kales, S. N., & Burks, S. V. (2012). Obesity is associated with the future risk of heavy truck crashes among newly recruited commercial drivers. Accident Analysis & Prevention, 49(1), 378-384. DOI: https://doi.org/10.1016/j.aap.2012.02.018
Apostolopoulos, Y., Sönmez, S., Shattell, M. M., Gonzales, C., & Fehrenbacher, C. (2013). Health survey of US long-haul truck drivers: work environment, physical health, and healthcare access. Work, 46(1), 113-123. DOI: https://doi.org/10.3233/WOR-121553
Belan, T. O., Oliveira, C. G. A., Machado, S. H. M., Brandão, O. S., & Silva, J. R. G. (2017). Prevalência do uso de anfetaminas por caminhoneiros. Acta Biomédica Brasiliensia, 8(2), 71-82.
Bombana, H. S., Gjerde, H., Santos, M. F., Jamt, R. E. G, Yonamine, M., Rohlfs, W. J. C., … Leyton, V. (2017). Prevalence of drugs in oral fluid from truck drivers in Brazilian highways. Forensic Science International, 273(1), 140-143. DOI: https://doi.org/10.1016/j.forsciint.2017.02.023
Crouch, D. J., Birky, M. M., Gust, S. W., Rollins, D. E., Walsh, J. M., Moulden, J. V., … Beckel, R W. (1993). The prevalence of drugs and alcohol in fatally injured truck drivers. Forensic Science International, 38(6), 1342-1353.
Fonseca, J. G., Viana, G. M., Souza, J. E. M., & Rossi-Barbosa, L. A. R. (2019). Fatores associados ao uso de anfetaminas entre caminhoneiros. RIES: Revista Interdisciplinar de Estudos em Saúde, 8(1), 116-125.
Gjerde, H., Christophersen, A. S., Normann, P. T., Pettersen, B. S., Sabaredzovic, A., Samuelsen, S. O., & Mørland, J. (2012). Analysis of alcohol and drugs in oral fluid from truck drivers in Norway. Traffic Injury Prevention, 13(1), 43-48. DOI: https://doi.org/10.1080/15389588.2011.627957
Gjerde, H., Sousa, T. R., Boni, R., Christophersen, A. S., Limberger, R. P., Zancanaro, I., … Pechansky F. (2014). A comparison of alcohol and drug use by random motor vehicle drivers in Brazil and Norway. International Journal of Drug Policy, 25(3), 393-400. DOI: https://doi.org/10.1016/j.drugpo.2014.01.019
Guinn, B. (1983). Job satisfaction, counterproductive behavior and circumstantial drug use among long-distance truckers. Psychoactive Drugs, 15(3), 185-188.
Knauth, D. R., Pilecco, F. B., Leal, A. F., Seffner, F., & Teixeira, A. M. (2012). Staying awake: truck drivers’ vulnerability in Rio Grande do Sul, Southern Brazil. Revista de Saúde Pública, 46(5), 886-893. DOI: https://doi.org/10.1590/S0034-89102012000500016
Labat, L., Fontaine, B., Delzenne, C., Doublet, A., Marek, M. C., Tellier, D., … Frimat, P. (2008). Prevalence of psychoactive substances in truck drivers in the Nord-Pas-de-Calais region (France). Forensic Science International, 174(2-3), 90-94. DOI: https://doi.org/10.1016/j.forsciint.2007.03.004
Laraqui, S., Laraqui, O., Tripodi, D., Manar, N., Aoudi, Y. E., Caubet, A., … Laraqui, C. H. (2011). Prevalence and risk factors of alertness disorders of professional drivers in Morocco. Sante Publique, 23(2), 89-100.
Leopoldo, K., Leyton, V., & Oliveira, L. G. (2015). Alcohol use alone and in combination with other drugs among truck drivers on highways in São Paulo State, Brazil: a cross-sectional study. Cadernos de Saúde Pública, 31(9), 1916-1928. DOI: http://dx.doi.org/10.1590/0102-311X00047214
Leyton, V., Sinagawa, D. M., Oliveira, K., Schmitz, W., Andreuccetti, G., & Martinis, B.S. (2012). Amphetamine, cocaine and cannabinoids use among truck drivers on the roads in the State of Sao Paulo, Brazil. Forensic Science International, 215(1-3), 25-27. DOI: https://doi.org/10.1016/j.forsciint.2011.03.032
Liberati, A., Altman, D. G., Tetzlaff, J., Mulrow, C., Gøtzsche, P. C., Ioannidis, J. P. A., … Moher, D. (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ, 339(1), 1-27. DOI: https://doi.org/10.1136/bmj.b2700
Mabbott, N. A., & Hartley, L. R. (1999). Patterns of stimulant drug use on Western Australian heavy transport routes. Traffic Psychology & Behaviour, 2(2), 115-130. DOI: https://doi.org/10.1016/S1369-8478(99)00012-1
Malta, M., Cardoso, L. O., Bastos, F. I., Magnanini, M. M., & Silva, C. M. (2010). STROBE initiative: guidelines on reporting observational studies. Revista de Saúde Pública, 44(3), 559-565. DOI: https://doi.org/10.1590/S0034-89102010000300021
Mieczkowski, T. (2010). Urinalysis and hair analysis for illicit drugs of driver applicants and drivers in the trucking industry. Journal of Forensic and Legal Medicine, 17(5), 254-260. DOI: https://doi.org/10.1016/j.jflm.2010.02.014
Mir, M. U., Khan, I., Ahmed, B., & Abdul Razzak, J. (2012). Alcohol and marijuana use while driving - an unexpected crash risk in Pakistani commercial drivers: a cross-sectional survey. BMC Public Health, 12(1), p. 1-7. DOI: https://doi.org/10.1186/1471-2458-12-145
Mongkolsirichaikul, D., Mokkhavesa, C., & Ratanabanangkoon, K. (1988). The incidence of amphetamine use among truck drivers from various regions of Thailand. Journal of the Medical Association of Thailand, 71(9), 471-474.
Moreira, R. S., & Gadani, J. A. A. B. (2009). A prevalência do uso de anfetaminas por caminhoneiros que passam pela cidade de Dourados-MS. Interbio, 3(2), 27-34.
Morgan, R. L., Whaley, P., Thayer, K. A., & Schünemann, H. J. (2018). Identifying the PECO: A framework for formulating good questions to explore the association of environmental and other exposures with health outcomes. Environment International, 121(Pt 1), 1027-1031. DOI: https://doi.org/10.1016/j.envint.2018.07.015
Nascimento, E. C., Nascimento, E., & Silva, J. P. (2007). Uso de álcool e anfetaminas entre caminhoneiros de estrada. Revista de Saúde Pública, 41(2), 290-293. DOI: http://dx.doi.org/10.1590/S0034-89102007000200017
O’Brien, B. C., Harris, I. B., Beckman, T. J., Reed, D. A., & Cook, D. A. (2014). Standards for reporting qualitative research: a synthesis of recommendations. Academic Medicine, 89(9), 1245-1251.
Okpataku, C. I. (2015). Pattern and reasons for substance use among long-distance commercial drivers in a Nigerian city. Indian Journal of Public Health, 59(4), 259-263. DOI: https://doi.org/10.4103/0019-557X.169649
Oliveira, L. G., Souza, L. M., Barroso, L. P., Gouvêa, M. J., Almeida, C. V., Muñoz, D. R., & Leyton, V. (2015). Occupational conditions and the risk of the use of amphetamines by truck drivers. Revista de Saúde Pública, 49(1), 1-9. DOI: https://doi.org/10.1590/S0034-8910.2015049005944
Peixe, T. S., Almeida, R. M., Girotto, E., Andrade, S. M., & Mesas, A. E. (2013). Use of illicit drugs by truck drivers arriving at Paranaguá port terminal, Brazil. Traffic Injury Prevention, 15(7), 673-677. DOI: https://doi.org/10.1080/15389588.2013.868893
Penteado, R. Z., Gonçalves, C. G. O., Costa, D. D., & Marques, J. M. (2008). Trabalho e saúde em motoristas de caminhão no interior de São Paulo. Saúde & Sociedade, 17(4), 35-45.
Pidetcha, P., Congpuong, P., Putriprawan, T., Rekakanakul, R., Suwanton, L., & Tantrarongroj, S. (1995). Screening for urinary amphetamine in truck drivers and drug addicts. Journal of the Medical Association of Thailand, 78(10), 554-558.
Pinheiro, M. P., Muniz, L. F., Silva, M. C. V., Resill, D. P., & Filho, P. C. P. T. (2015). Amphetamines consumption and alcohol for truck drivers. Revista de Enfermagem UFPE, 9(7), 8519-8525.
Remor, K. V. T., Monteiro, M. T. M., Rosa, V. D., Iacovski, R. B., Sakae, T. M., & Galato, D. (2016). Abusive consumption of psychoactive substances by truck drivers. Medical & Clinical Reviews, 2(1), 1-6. DOI: https://doi.org/10.21767/2471-299X.1000010
Riva, M. M., Marchett, F. A., Giupponi, V., & Mosconi, G. (2010). Health surveillance of truck drivers: it is not just a question of drugs. Description of a one-year experience. La Medicina del lavoro, 101(3), 207-217.
Silva, O. A., Greve, J. M. D., Yonamine, M., & Leyton, V. (2003). Drug use by truck drivers in Brazil. Drugs: Education, Prevention and Policy, 10(2), 135-139. DOI: https://doi.org/10.1080/0968763021000057727
Sinagawa, D. M., Carvalho, H. B., Andreuccetti, G., Prado, N. V., Oliveira, K. C., Yonamine, M., … Leyton V. (2014). Association between travel length and drug use among Brazilian truck drivers. Traffic Injury Prevention, 16(1), 5-9. DOI: https://doi.org/10.1080/15389588.2014.906589
Takitane, J., Oliveira, L. G., Endo, L. G., Oliveira, K. C., Muñoz, D. R., Yonamine, M., & Leyton, V. (2014). Uso de anfetaminas por motoristas de caminhão em rodovias do Estado de São Paulo: um risco à ocorrência de acidentes de trânsito? Ciência & Saúde Coletiva, 18(5), 1247-1254. DOI: https://doi.org/10.1590/S1413-81232013000500009
Thiese, M. S., Effiong, A. C., Ott, U., Passey, D. G., Arnold, Z. C., Ronna, B. B., … Murtaugh, M. A. (2015). A clinical trial on weight loss among truck drivers. International Journal of Occupational and Environmental Medicine, 6(2), 104-112. DOI: https://doi.org/10.15171/ijoem.2015.551
Vandenbroucke, J. P., Von Elm, E., Altman, D. G., Gotzsche, P. C., Mulrow, C. D., Pocock, S. J., … Egger, M. (2007). Strobe initiative. strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. PLoS Medicine, 4(10), p. 1500-1524.
Wendler, E. A., Busato, C. R., & Miyoshi, E. (2003). Uso de anfetaminas por motoristas de caminhão para reduzir o sono. Publicatio UEPG, 9(3), 7-14. DOI: https://doi.org/10.5212/publicatio%20uepg.v9i3.364
Williamson, A. (2007). Predictors of psychostimulant use by long-distance truck drivers. American Journal of Epidemiology, 166(11), 1320-1326. DOI: https://doi.org/10.1093/aje/kwm205
Yonamine, M., Sanches, L. R., Paranhos, B. A., Almeida, R. M., Andreuccetti, G., & Leyton, V. (2013). Detecting alcohol and illicit drugs in oral fluid samples collected from truck drivers in the state of São Paulo, Brazil. Traffic Injury Prevention, 14(2), 127-131. DOI: https://doi.org/10.1080/15389588.2012.696222
Girotto, E., Andrade, S. M., Mesas, A. E., González, A. D., & Guidoni, C. M. (2015). Working conditions and illicit psychoactive substance use among truck drivers in Brazil. Occupational and Environmental Medicine, 72(11), 764-769. DOI: https://doi.org/10.1136/oemed-2015-102868
Notas de autor
aldopachecoferreira@gmail.com