ABSTRACT
Introduction: N-terminal pro-brain natriuretic peptide (NT-proBNP) is a biomarker for heart stress and heart failure, with its production triggered by the stretching of cardiac fibers. This study investigates if elevated NT-proBNP levels can independently predict poor outcomes for patients undergoing heart surgery.
Methods: A systematic review was performed in the PubMed®, Latin American and Caribbean Health Sciences Literature (or LILACS), Physiotherapy Evidence Database (PEDro), Web of Science, and Embase databases, with the following descriptors: "NT-proBNP" OR "NTproBNP" OR "N- terminal pro-B-type natriuretic peptide" OR "N- terminal pro brain natriuretic peptide" OR "amino terminal pro brain natriuretic peptide" AND "Cardiovascular Surgical Procedures" NOT "Pediatric" OR "children" NOT "cancer" OR "oncology" NOT "animal*". Articles that evaluated NT-proBNP and adverse outcomes in cardiac surgical patients were chosen. The levels of evidence and the strength of recommendation were assessed considering the Grading of Recommendations, Assessment, Development and Evaluation (or GRADE) system and validity by the PEDro scale. For systematic review, the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (or PRISMA) criteria and the Population, Intervention, Comparison, Outcome (or PICO) strategy were followed.
Results: Forty-seven articles were included, of which 17 were related to serious complications, including mortality.
Conclusion: Preoperative NT-proBNP is a prognostic marker for mortality, length of stay in the postoperative intensive care unit, postoperative acute kidney injury, postoperative atrial fibrillation, postoperative low cardiac output, postoperative prolonged mechanical ventilation time, prolonged hospitalization time, unscheduled hospital readmission related to heart problems, and postoperative heart failure.
Keywords: Biomarkers, Cardiac Surgery, Prognosis, Systematic Review.
REVIEW ARTICLE
N-terminal Pro-brain Natriuretic Peptide as a Prognostic Biomarker for Cardiac Surgeries: A Systematic Review
Received: 05 December 2024
Revised document received: 09 March 2025
Accepted: 03 April 2025
The cerebral N-terminal pro-brain natriuretic peptide (NT-proBNP) is a precursor of brain natriuretic peptide (BNP) hormone, which is produced and released by ventricular cardiomyocytes in response to myocardial wall stress and ischemia[1-4]. Elevations in NT-proBNP levels have been associated with poor outcomes in a variety of settings, including acute coronary syndrome, congestive heart failure (HF), and major noncardiac surgery[5-7]. In patients with asymptomatic and symptomatic aortic stenosis (AS), NT-proBNP is independently associated with outcomes[8]. NT-proBNP is also a predictor of outcomes after valve replacement surgery in AS[8,9]. Several studies have recently investigated associations of NT-proBNP with outcomes after transcatheter aortic valve replacement[10].
Preoperative assessment systems in cardiac surgery patients like the European System for Cardiac Operative Risk Evaluation (or EuroSCORE) have been widely used to predict the risk of postoperative mortality. However, these systems are limited by their complexity, subjectivity in calculation, and suboptimal performance in predicting worse postoperative morbidity. In addition, they may not apply to all patient cohorts[11,12].
With the increasing number of patients undergoing high-risk cardiac surgeries, accurate risk assessment becomes crucial for clinical management and the implementation of preventive measures[13,14]. We assume that NT pro-BNP is an independent predictor of adverse outcomes. To investigate this hypothesis, we conducted a systematic review.
A systematic literature review relating to NT-proBNP and cardiac surgical patients was conducted. The PubMed®, Latin American and Caribbean Health Sciences Literature (or LILACS), Physiotherapy Evidence Database (PEDro), Web of Science, and Embase databases were used. The descriptors used to search all databases were: "NT-proBNP" OR "NTproBNP" OR "N- terminal pro-B-type natriuretic peptide" OR "N- terminal pro brain natriuretic peptide" OR "amino terminal pro brain natriuretic peptide" AND "Cardiovascular Surgical Procedures" NOT "Pediatric" OR "children" NOT "cancer" OR "oncology" NOT "animal*".
The final PubMed® search strategy used as a basis for the other databases was: ((((((((((NT-proBNP) OR (NTproBNP)) OR (N- terminal pro-B-type natriuretic peptide)) OR (N- terminal pro brain natriuretic peptide)) OR (amino terminal pro brain natriuretic peptide))) AND (Cardiovascular Surgical Procedures)) NOT ((Pediatric) OR (children))) NOT ((cancer) OR (oncology))) NOT (animal*)).
The parameters adopted for inclusion and exclusion in this research were addressing a theme appropriate to the one presented here, reporting a study on human beings, containing clear, objective principles consistent with the title of the research, observational studies, and retrospective and prospective cohorts that investigated the association between preoperative NT-proBNP and postoperative complications, including death, in adults and elderly patients who underwent cardiac surgeries such as myocardial coronary artery bypass grafting (CABG), valve replacements or repairs, as well as tumor resections and heart transplantation. Articles that did not meet these criteria were not selected, such as studies with percutaneous coronary intervention or angioplasty, large-vessel surgeries, noncardiac surgeries, randomized studies, and reviews. Initially, the studies were selected by title and abstract; only when there was not enough information in the title and abstract to allow a clear decision, the studies were obtained in full.
All selected studies were evaluated in full to obtain essential information. Levels of evidence and strength of the recommendation were assessed considering the Grading of Recommendations, Assessment, Development and Evaluation (GRADE) system and validity by the PEDro scale. A systematic review was conducted following Preferred Reporting Items for Systematic Reviews and Meta-Analyses (or PRISMA) guidelines and a Population, Intervention, Comparison, Outcome (or PICO) strategy. No time filter was applied; however, data extraction took place up to January 2023. This review was registered on the PROSPERO platform under registration number CRD42023435271.
Data were extracted from the selected articles, including the first author's last name, publication year, study period, number of cases and participants, primary and secondary outcomes, objectives, and key results. A comparison across databases was conducted to identify and eliminate any duplicate studies.
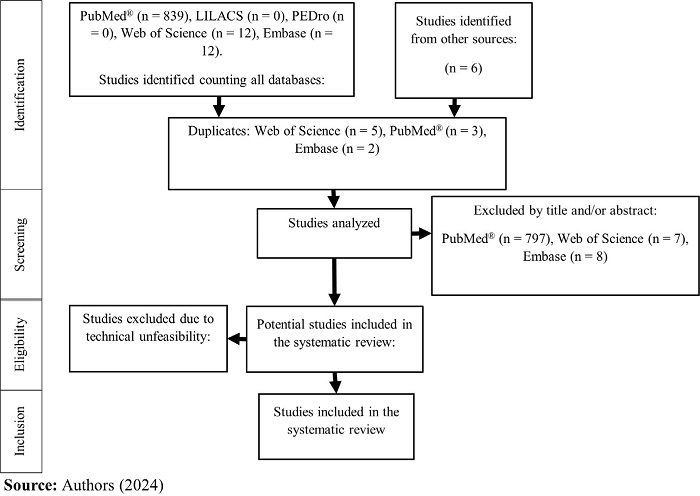
An initial literature search identified 869 records. After screening and abstract review, 52 studies were selected for full-text evaluation. Following a thorough assessment, three studies were excluded due to technical infeasibility, and six were excluded as they originated from sources other than peer-reviewed journals (Figure 1). Ultimately, 47 studies met the predefined inclusion criteria and were included in this systematic review.
In total, 58,743 patients underwent heart surgeries in our survey, of which 29.8% had only CABG[15-28], 21.3% had only had valve surgeries[29-38], 4.3% only had ventricular remodeling[39,40], 2.1% had a heart transplant[41], 2.1% had septal myectomy[42], and 40.4% had more than one modality of cardiac surgery[3,43–60].
Mortality was the most frequent outcome, reported in 33 studies[3,15,17,19,22-24,28-34,36-42,44,45,48-54,56,58,60]; other outcomes were prolonged postoperative intensive care unit (ICU) stay (16 studies[15,19,22,23,28,31,34,43,44,48,50–52,54,58,60]), postoperative acute kidney injury (AKI) (14 studies[3,22,23,28,34,43–45,50,54,57–60]), postoperative low cardiac debit (14 studies[3,15,18,22,23,43,44,48,50,52,54,55,58,60]), postoperative new atrial fibrillation (AF) (14 studies[3,15,16,19–21,23,25,27,28,34,36,48,52]), prolonged postoperative duration of mechanical ventilation (MV) (nine studies[15,22,28,43,44,48,51,52,54]), postoperative cerebrovascular events (nine studies[3,22,23,28,36,40,44,51,58]), prolonged length of hospital stay (eight studies[15,19,21,31,42,48,54,60]), unscheduled hospital readmission related to heart problems (four studies[19,37,38,58]), emergency reoperation for bleeding (four studies[3,28,44,58]), postoperative acute myocardial infarction (AMI) (three studies[15,22,28]), postoperative HF (three studies[37,39,51]), postoperative infection (three studies[3,28,58]), and presence of postoperative delirium (two studies[22,46]) (Tables 1 and 2).


Additionally, one study assessed the association of preoperative NT-proBNP with postoperative circulating endothelial progenitor cells[47], postoperative cardiac pump function[35], and left ventricular diastolic dysfunction[26] (Tables 1 and 2).
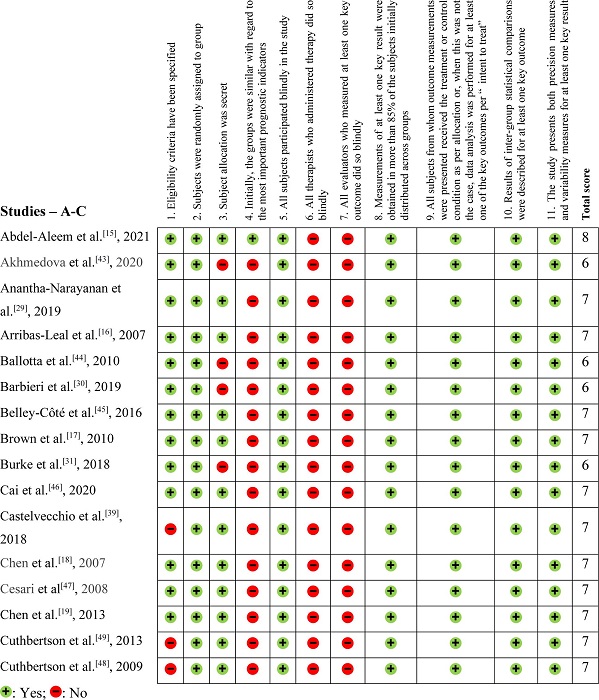
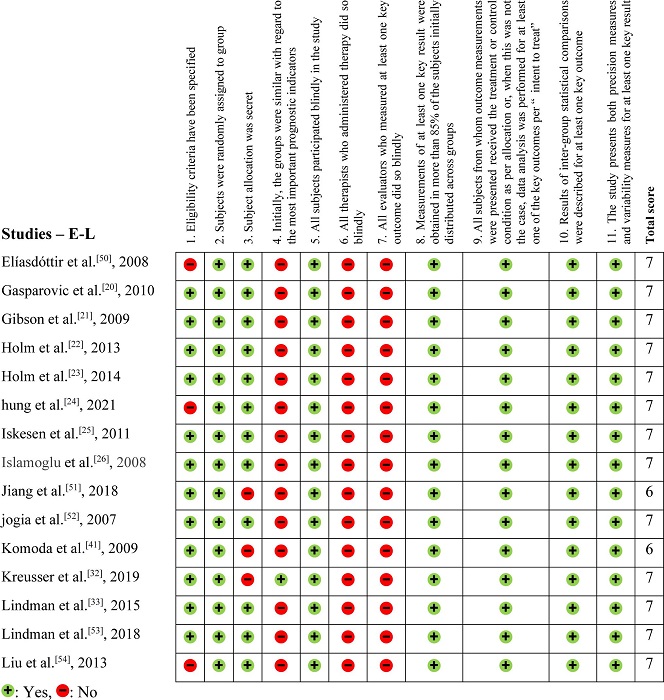
The methodological evaluation, demonstrated in Figures 2, 3, and 4, exposed that eight articles[24,35,39,40,48–50,54] had problems with external validity according to the Physiotherapy Evidence Database (PEDro) scale (they did not present the inclusion or exclusion factors of their studies). According to the PEDro scale, 15 studies were negative for Question 3[27,30-32,34,37,38,40-44,51,58,59], only two were positive for Question 4[15,32], and none were positive for Questions 6 and 7.
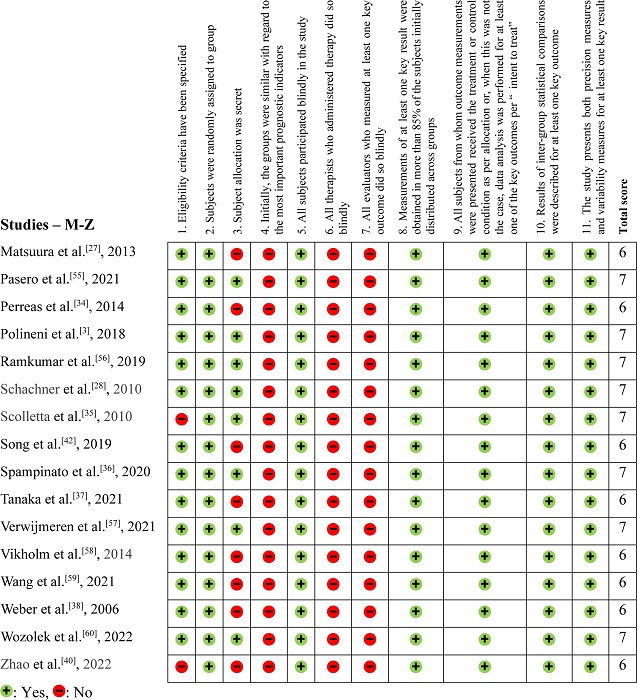
The assessment of the risk of bias, inconsistency, indirectness, and imprecision using the PEDro and GRADE tools revealed that the overall quality of the evidence was generally not serious (Table 3). For new-onset AF, we observed a large association (odds ratio [OR] > 2.0 in at least two studies) and a very large effect on mortality (OR > 5.0). Additionally, a direct correlation was observed between NT-proBNP levels and mortality rates, as well as other adverse outcomes, including prolonged ICU stay, AKI, low cardiac output (LCO), new-onset AF, prolonged MV, cerebrovascular events, prolonged hospitalization, emergency reoperation, postoperative HF, and postoperative delirium.
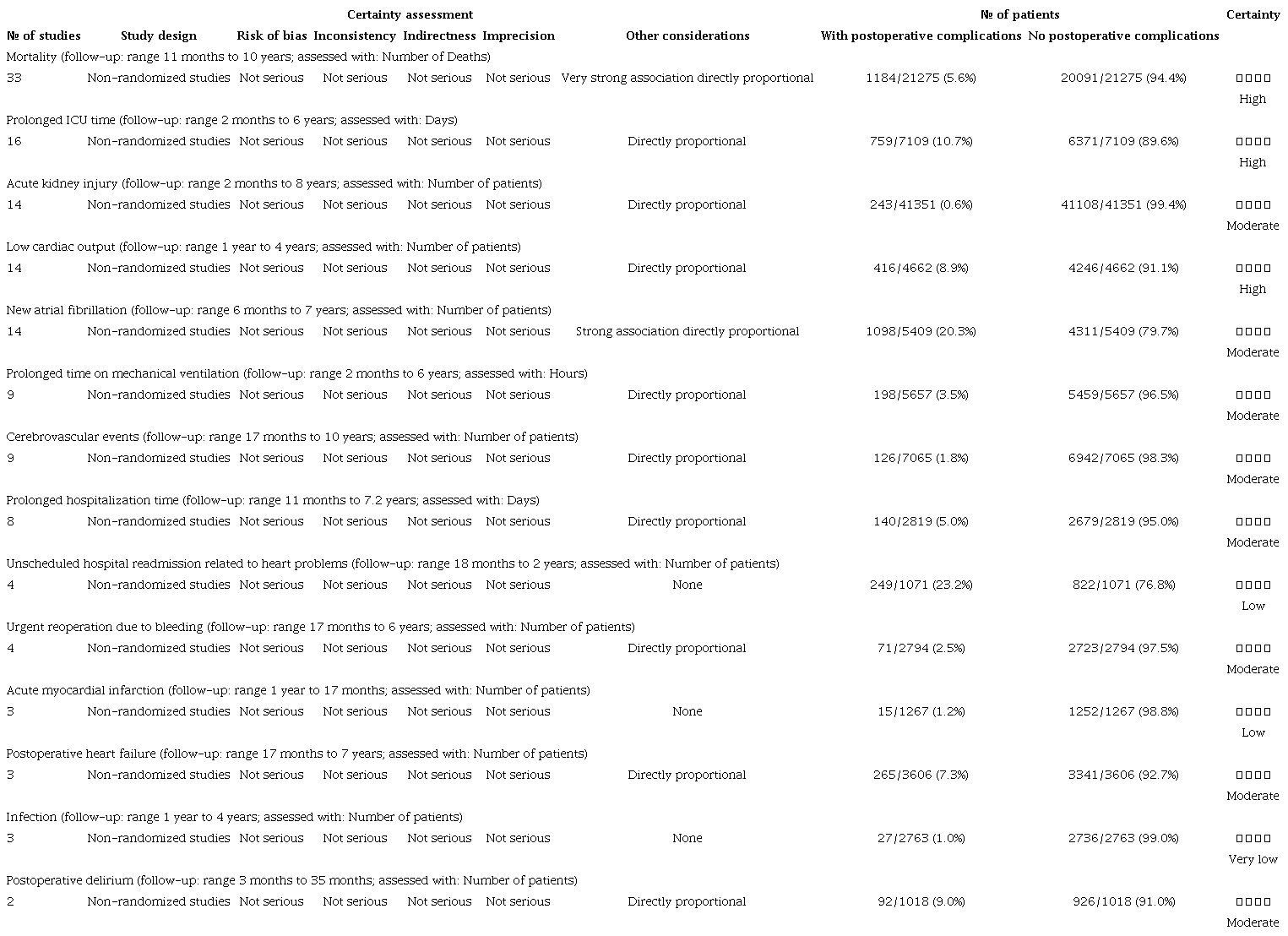
For mortality and prolonged ICU stay, we found high-certainty evidence, suggesting that future research is unlikely to substantially impact our confidence in the effect estimate. For nine outcomes (AKI, LCO, new AF, prolonged MV time, cerebrovascular events, prolonged hospital stay, emergency reoperation for bleeding, postoperative HF, and postoperative delirium), the certainty of the evidence was moderate, suggesting that future research may significantly impact our confidence in the estimated effects. For unscheduled hospital readmission for cardiac reasons and new AMI, the certainty of the evidence was low or very low, indicating that future research is likely to substantially change our understanding of the effects. And there was one outcome (infection) with a very low level of evidence suggesting that any estimate of effect is very uncertain.
In our review, we observed that, in those studies that evaluated mortality, approximately 7% of the patients died, which is a critical outcome for this patient profile. Twenty-five of the articles that assessed mortality[3,17,22–24,28–30,32,34,36,37,39–42,44,45,48,50,51,53,54,56,58] agreed that high levels of preoperative NT-proBNP were related to higher mortality rates in cardiac surgical patients.
Holm et al.[23] (2014), in their research, showed that patients with high preoperative levels of NT-proBNP were 9.94 times more likely (95% confidence interval [CI]: 1.01 – 98.9; P = 0.049) to die when compared to the group with low levels. This is in line with the work of Spampinato et al.[36] (2020) who demonstrated that the same patient profile had a 7.26-fold increased risk (95% CI: 2.52 – 20.93; P < 0.001) of having this outcome. Polineni et al.[3] (2018) reported that this patient profile was 5.43 times more likely (95% CI: 1.21 – 24.44; P = 0.027) of not surviving. This association was confirmed by all 16 studies[17,22,28,30,32,33,37,39,40,42,45,48,51,54,56,58] that demonstrated an independent association between mortality and high NT-proBNP levels. Additionally, six other studies[24,29,34,41,49,50] showed a significant association between these parameters.
On the other hand, Abdel-Aleem et al.[15] (2021), Ballotta et al.[44] (2010), Burke et al.[31] (2018), Chen et al.[19] (2013), Jogia et al.[52] (2007), Weber et al.[38] (2006), Lindiman et al.[53] (2018), and Wozolek et al.[60] (2022) failed to demonstrate this association. However, all these studies were developed with < 150 patients, except the last two, with 665 patients and 250 patients, respectively. Furthermore, none of the studies included a sample size calculation to ensure adequate statistical power. This omission raises concerns about the potential lack of representativeness of the study participants.
Another well-studied outcome was prolonged ICU stay, of which 16 of the studies included[15,19,22,23,28,31,34,43,44,48,50–52,54,58,60] explained. Jiang et al.[51] (2018) demonstrated a large-scale effect in their research, patients who had the highest NT-proBNP preoperatively were 2.87 times more likely (95% CI: 1.56 – 5.30; P = 0.001) to have long-term ICU stays. This was found also by Cuthbertson et al.[48] (2009), who reported that higher levels of NT-proBNP at the preoperative time were independently associated with 1.03 more chances (95% CI: 1.01 – 1.05; P = 0.003) of longer than one day in the ICU. And it was corroborated by Liu et al.[54] (2013) in their study of various cardiac surgeries, where they also showed an independent association of (P = 0.004) between NT-proBNP and this complication. Other six items[23,28,31,44,50,58] followed this reasoning, demonstrating a significant association between the biomarker studied and this outcome, but they performed only univariate analyses in their studies, reducing the strength of the evidence.
The third most studied outcome was AKI, which 14 articles[3,22,23,28,34,43–45,50,54,57–60] approached. Of the included studies, nine[3,22,23,28,34,43,50,54,58] demonstrated a significant association between NT-proBNP levels and the development of postoperative AKI in univariate analysis. Belley-Côté et al.[45] (2016) in their prospective cohort also showed an independent association between high pre-surgical levels of NT-proBNP and severe AKI (P = 0.030), which similarly occurred in the studies by Verwijmeren et al.[57] (2021) e Wang et al.[59] (2021).
The studies by Holm et al. (2013[22], 2014[23]) revealed a very strong association between preoperative NT-proBNP levels and the development of LCO in multivariate analyses, with OR of 24.9 (95% CI: 2.9 - 214; P = 0.004) and 9.94 (95% CI: 1.01 - 98.9; P = 0.049), respectively. These findings underscore the high predictive power of preoperative NT-proBNP for this outcome, which may be attributed to its role as a biomarker of myocardial involvement. Of the other 12 articles[3,15,18,43,44,48,50,52,54,55,58,60], ten studies[3,18,43,44,48,50,52,54,55,58] agreed with this information.
Gibson et al.[21] (2009) demonstrated an independent association between preoperative NT-proBNP and AF, bringing an increase of 3.12 times more chances (95% CI: 1.48 - 6.59; P=0.003) of developing new AF at the postoperative time when NT-proBNP levels were the highest preoperatively. Other six items[3,20,25,27,34,48], of the 14 evaluated[3,15,16,19–21,23,25,27,28,34,36,48,52], corroborated this association in their univariate analyses.
Nine studies[15,22,28,43,44,48,51,52,54] evaluated the association between prolonged MV time and NT-proBNP, while seven[22,28,44,48,51,52,54] agreed with the association between these parameters, but none of them performed a multivariate analysis to evaluate the possible confounding parameters of these associations, reducing the value of the evidence.
Regarding cerebrovascular events, five articles[3,22,23,40,58] of nine[3,22,23,28,36,40,44,51,58] agreed with the association between NT-proBNP and the aforementioned outcome. Of these, only Zhao et al.[40] (2022) performed a multivariate analysis, demonstrating that high preoperative NT-proBNP levels were associated with 1,017 times more chances of developing them at the postoperative time.
The study of Cuthbertson et al.[48] (2009) presented NT-proBNP levels as independent predictors of a hospital stay > 1 week (OR 1.070, P < 0.001), and this can be explained by the fact that the population evaluated was significantly higher. Liu et al.[54] (2013) also found an independent association (P = 0.019) between these parameters. These findings were corroborated by the study by Song et al.[42] (2019), which demonstrated in its univariate analysis that postoperative hospital stay was significantly longer in patients with NT-proBNP > 2080 pg/mL (P ≤ 0.001). These findings are supported by Wozolek et al.[60] (2022) which also, in univariate analysis, presents a similar association (P = 0.010).
Tanaka et al.[37] (2021) showed in their study that high levels of pre-surgical NT-proBNP were associated with rates of hospital readmission for cardiac causes, which were 1.5 times (95% CI: 1.03 – 2.17; P = 0.030) more likely to be readmitted to the hospital. The other three studies[19,38,58] that evaluated this outcome did not find a statistically significant association.
None of the studies[3,28,44,58] that evaluated emergency reoperation was able to express a statistically significant association, suggesting that preoperative NT-proBNP is not a good biomarker to predict this outcome.
AMI was a complication addressed in three articles in this review[15,22,28]. In the study by Abdel-Aleem et al.[15] (2021), although 6% of the patients developed AMI in the postoperative period, there were no significant differences in preoperative NT-proBNP levels between patients with and without this complication (P = 0.397). The studies by Schachner et al.[28] (2010) and Holm et al.[22] (2013) also did not show a statistically significant association (P = 0.458 and P = 0.130, respectively).
The study by Tanaka et al.[37] (2021) identified that the group with reduced NT-proBNP biomarker independently had a 1.5-fold lower risk of developing the composite outcome, including rehospitalization due to worsening HF (95% CI: 1.03 – 2.17; P = 0.03). Also, the study by Jiang et al.[51] (2018) evaluated 2,978 patients and identified that preoperative NT-proBNP demonstrated an independent and significant association with postoperative severe heart failure (PSHF) in patients with coronary artery disease (CAD) and mitral regurgitation (P < 0.0001) and also with mitral stenosis (P = 0.047). In the multivariate analysis, NT-proBNP 855 ng/L emerged as an independent risk factor for PSHF in patients with CAD (adjusted OR 2.87; 95% CI: 1.56 – 5.30; P = 0.001).
Three articles[3,28,58] evaluated the relationship between NT-proBNP and infections, from which only the study by Polineni et al.[3] (2018), with a sample of 1,544 patients divided into tertiles and two groups based on the mean NT-proBNP value, demonstrated in the univariate analysis of the data an association between NT-proBNP and pneumonia (95% CI = 1,070 – 1,250); however, in the multivariate analysis, the association was not confirmed. Therefore, in none of the studies a relevant association was found between preoperative NT-proBNP values and the occurrence of infection in patients undergoing cardiac surgery.
Regarding postoperative delirium, only two articles studied the topic. Of these, only the study by Cai et al.[46] (2020) demonstrated a significant and independent association (OR 1.240, 95% CI 1.010 – 1.520; P = 0.033) between preoperative NT-proBNP and the occurrence of this outcome.
In five studies, no association was found between pre-surgical NT-proBNP and any of the outcomes studied, those are: Abdel-Aleem et al.[15] (2021), Lindiman et al.[53] (2018), Arribas-Leal et al.[16] (2007), Weber et al.[38] (2006), and Chen et al.[19] (2013). It is important to note that the absence of an association in certain studies underscores the heterogeneity of the surgical population and the potential influence of various factors on the relationship between NT-proBNP and postoperative outcomes. In addition, most studies evaluated surgeries used in different cardiac anatomical sites, which affects their recovery and complications, justifying possible disparities found. Another point worth noting was the scarcity of sample calculations to validate the representativeness of the studies.
In this systematic review, we found that the PEDro score was lower than expected due to the nature of the articles. Retrospective articles could not score positively on Question 3, for example. Likewise, these are not randomized studies, blinding patients and evaluators became unfeasible. Furthermore, the significant variability in NT-proBNP levels observed between the case and control groups made it challenging to achieve homogeneity among the study populations. This variability may have contributed to the high proportion of negative responses for Question 3 of the PEDro scale, which assesses the use of appropriate control groups.
There were no limitations to the current study.
Pre-surgical NT-proBNP is a good independent biomarker to predict mortality, prolonged ICU stay, and LCO. Further studies are needed to evaluate its efficacy to independently predict postoperative AKI, new AF, cerebrovascular events, length of hospital stay, hospital readmission for cardiac causes, and postoperative delirium.
Correspondence Address: Barbara Giovanna Souza Silva Queiroz, Programa de Pós-Graduação em Ciências da Saúde, Faculdade de Ciências Médicas, Universidade de Pernambuco, Av. Gov. Agamenon Magalhães, Santo Amaro, Recife, PE, Brasil, Zip Code: 50100-010, E-mail: barbara.squeiroz@upe.br







