Artículos

Esta obra está bajo una Licencia Creative Commons Atribución-SinDerivar 4.0 Internacional.
Recepción: 28 Junio 2021
Aprobación: 15 Agosto 2021
Publicación: 30 Agosto 2021
DOI: https://doi.org/10.5281/zenodo.5791081
Abstract: With the rapid development of medicine (the creation of new medical technologies: medicines, medical equipment, and novel treatments for various diseases) and limited healthcare resources, it is important to choose the best treatment that would be not only medically but also cost-effective. This study's primary objective is to evaluate the cost-effectiveness of various treatment modalities for microbial Eczema in children. To satisfy that objective, a single-center open comparative retrospective/prospective clinical study is conducted. This survey incorporated pediatric patients (n=108) with microbial Eczema and the disease duration of more than six months who had been admitted to the Department of Dermatology of the Russian Children's Clinical Hospital. Based on the study results, it can be concluded that the introduction of CAP (Community-Acquired Pneumonia) into clinical practice is cost-effective (viable) and can promote the availability of effective modern methods of microbial eczema treatment, particularly in children.
Keywords: medical technologies, treatment, microbial Eczema, children, modern effective methods.
Resumen: Con el rápido desarrollo de la medicina (la creación de nuevas tecnologías médicas: medicamentos, equipos médicos y tratamientos novedosos para diversas enfermedades) y los recursos sanitarios limitados, es importante elegir el mejor tratamiento que sea no solo desde el punto de vista médico sino también rentable. El objetivo principal de este estudio es evaluar la rentabilidad de diversas modalidades de tratamiento para el eccema microbiano en niños. Para satisfacer ese objetivo, se lleva a cabo un estudio clínico prospectivo / retrospectivo comparativo abierto de un solo centro. Esta encuesta incorporó pacientes pediátricos (n = 108) con eccema microbiano y la duración de la enfermedad de más de 6 meses que habían sido ingresados en el Departamento de Dermatología del Hospital Clínico Infantil Ruso. Sobre la base de los resultados del estudio, se puede concluir que la introducción de la NAC (neumonía adquirida en la comunidad) en la práctica clínica es rentable (viable) y tiene la capacidad de promover la disponibilidad de métodos modernos y eficaces de tratamiento del eccema microbiano. particularmente en los niños.
Palabras clave: tecnologías médicas, tratamiento, eccema microbiano, niños, métodos modernos eficaces.
Introduction
The assessment of the effectiveness of various treatments includes both the analysis of patient satisfaction and healthcare service quality and the analysis of treatment safety and financial viability1-3. Over the past years, much attention has been paid to the economic analysis of different methods and technologies in medicine4-6.
Microbial Eczema (ME) has a chronic relapsing course and is often accompanied by antibiotic resistance and fungal infections7,8, which necessitates the development of new methods (strategies) of ME treatment9,10.
Thereby, our study aimed to perform a clinical and economic evaluation of a new treatment for children with ME in comparison with alternative treatment options. We hypothesized that the addition of cold atmospheric plasma to conventional treatment approaches would be cost-effective. To achieve the aim of the study, we fulfilled the following tasks:
- assessed the direct medical costs in a cohort of children with ME treated with alternative treatment methods;
- performed clinical and economic evaluation of alternative treatment strategies for ME in a pediatric cohort;
- performed a budget impact analysis of alternative treatment strategies.
Materials and Methods
An assessment of the economic impact of a new treatment method involving the use of cold atmospheric plasma (CAP) in the management of children with ME was based on the results of a single-center open comparative retrospective/prospective clinical study. The Local Ethics Committee approved the clinical study of the Russian Children's Clinical Hospital of the N.I. Pirogov Russian National Research Medical University and the Scientific Council of the N.I. Pirogov Russian National Research Medical University.
The study included pediatric patients (n=108) with microbial Eczema and the disease duration of more than six months who had been admitted to the Department of Dermatology of the Russian Children's Clinical Hospital. The inclusion criteria were as follows: an established diagnosis of ME; the absence of atopic dermatitis and/or atopic asthma; no less than two relapses within a year; written informed consent from the patients' parents for the participation in the study and for the use of personal data in scientific publications (Table 1).
Table 1. The characteristics of patients with microbial Eczema enrolled in the study.
The characteristics of patients with microbial Eczema enrolled in the study
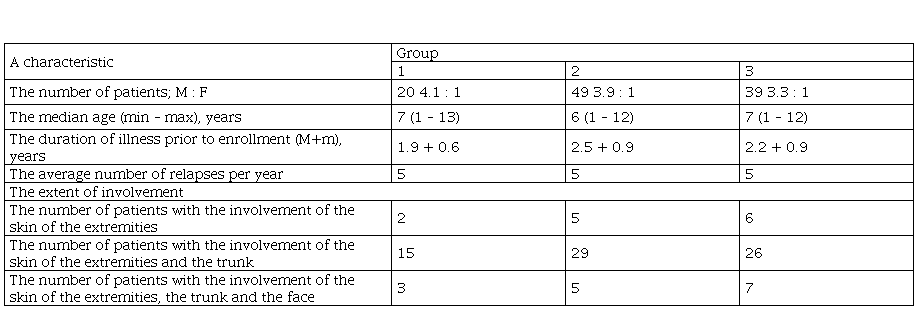
A retrospective group (Group 1 and a part of Group 2) included 20 patients aged between 1 and 13 years (the median age was nine years old) who had been treated at the Russian Children's Clinical Hospital in 2016 - 2017 and had been given topical treatment with hydrocortisone in combination with antibiotics (hydrocortisone + neomycin + natamycin; Trade name: Pimafucort.) together with a first-generation antihistamine drug (Suprastin at an age-adjusted dose) over 14 days – a standard treatment (Strategy 1) and ten patients aged between 1 and 13 years (the median age was seven years old) who had been treated at the Russian Children's Clinical Hospital in 2016 - 2017 and had been given the standard treatment in combination with laser therapy (transcutaneous laser blood irradiation with low-level helium-neon laser No.5) (Strategy 2).
In the prospective part of the study, the patients were randomized to two treatment groups in a 1:1 ratio. Group 2 patients (n=39) received the standard treatment in combination with laser therapy (transcutaneous laser blood irradiation with low-level helium-neon laser No. 5) (Strategy 2). Transcutaneous laser blood irradiation with low-level helium-neon laser (laser intensity: 1 mW/cm., wavelength: 633 nm) was carried out at the Department of Cryo- and Laser Surgery of the Russian Children's Clinical Hospital (headed by I.N. Kuzetchenko). Group 3 patients (n=39) were given the standard treatment and cold atmospheric plasma (CAP) treatment (5 procedures) (Strategy 3). As a CAP source, HELIOS device (PLAZMA Scientific Production Center, Russia; Roszdravnadzor license No. РЗН 2016/4374) was employed. Microbial eczema lesions were exposed to the plasma jet (externally, without contact with the skin) generated by gas with a flow rate of 1.5 L/min on the rotameter scale; the plasma jet intensity was 70%. The exposure time was 2 minutes per square centimeter.
The patients were followed up for a year, which enabled us to analyze the rate of ME relapses in each group.
The effectiveness of treatment was evaluated by the time for the resolution of skin inflammation and the number of relapses during a 1-year follow-up (a relapse therapy was the same as that previously used in the study).
The severity of microbial Eczema was assessed using Microbial Eczema Severity Index (MESI), where mild is defined as ⩽ 15 points, moderate as 16 to 25 points, and severe as 26 points or more11.
Itch intensity was assessed using the following categories: 0 points for no itch, 1 point for the low itch, 2 points for the mild itch, 3 points for the moderate itch, and 4 points for severe itch 12-16.
The effectiveness of ME treatment was measured using the following clinical criteria: clinical recovery - the total clearance of ME skin symptoms; significant improvement - the clearance of the majority of lesions, the disappearance of pustules, 4-fold improvement of the MESI scores; improvement - slow positive changes, 2-fold improvement of the MESI scores; no response - no changes in skin symptoms.
We also analyzed the number of relapses that occurred during a 1-year follow-up (a relapse therapy was the same as that previously used in the study). The number and intensity of adverse events assessed the safety of the therapy.
The mathematical computations were performed on a personal computer with Microsoft Office Professional Plus 2019. The calculations of descriptive statistics and the comparison of groups were performed using SPSS Statistics 20.0 (IBM Corporation, USA).
Descriptive statistics. Categorical variables were presented as frequencies (percentages). The median and the interquartile range were used to characterize continuous variables (for non-normal distribution). The normality of distribution was tested using the Shapiro-Wilk test. We used the Mann-Whitney U-test (when comparing 2 groups) and the Kruskal-Wallis test (when comparing 3 and more groups) to compare independent samples of ordinal and continuous data.
Depending on the shapes of distributions, we used various types of statistical tests (parametric and non-parametric ones) because of significant fluctuations in the values of ordered samples which are typical of biological objects. For normally distributed variables, parametric tests are usually more precise than non-parametric tests. The .-test was used to detect differences between the means of two samples.
The groups were comparable for sex, age, the duration and number of ME relapses, the severity of skin involvement, and itch intensity. The results of the retrospective/prospective study showed a significant difference between study groups receiving the standard treatment in combination with CAP, standard treatment only, and standard treatment in combination with laser therapy (Table 2):
In Group 1, only 5% of the patients achieved a total ME resolution; a significant improvement was observed in 30% of cases. In Group 2, 6% of the children achieved a total ME resolution; a significant improvement was observed in 74% of patients. In Group 3, 67% of the patients achieved a total ME resolution; a significant improvement was observed in the remaining children (33%).
The mean time to next ME relapse was 2.5 months, four months and eight months in Group 1, Group 2, and Group 3, respectively. The patients from Group 2 and Group 3 had no adverse events.
The mean duration of hospital stay for patients with moderate/severe ME was 14.5 bed-days, 11 bed-days, and 6 bed-days in Group 1, Group 2, and Group 3, respectively.
For subsequent clinical and economic analysis as well as a budget impact analysis, we developed an analytical model using MS Office Excel 2019. In our calculations, we took into account only direct medical costs: drug treatment costs, accompanying costs related to the management of the patients (consumable materials, laboratory diagnostic tests), the costs of laser therapy and CAP procedures.
The calculation of medical costs was performed in full compliance with the Order of the Ministry of Healthcare of the Russian Federation dated 29 December 2012 No.1631н "On the Approval of the Procedure of Price Setting for Medical Services Provided by Public Medical Institutions under the supervision of the Ministry of Healthcare of the Russian Federation" (registered in the Ministry of Justice of the Russian Federation on 18 April 2013 under No.281186). The costs of other procedures correspond to the Russian Children's Clinical Hospital of the N.I. Pirogov Russian National Research Medical University as of 1 May 2021. The cost of therapy per day for one patient with ME was as follows:
- Strategy 1: 11 855.11 rubles;
- Strategy 2: 12 536.44 rubles;
- Strategy 3: 14 315.88 rubles.
Direct medical costs of each Strategy with respect to the duration of treatment are provided in Table 3.
Table 2. The results of different treatment strategies for microbial Eczema
The results of different treatment strategies for microbial Eczema
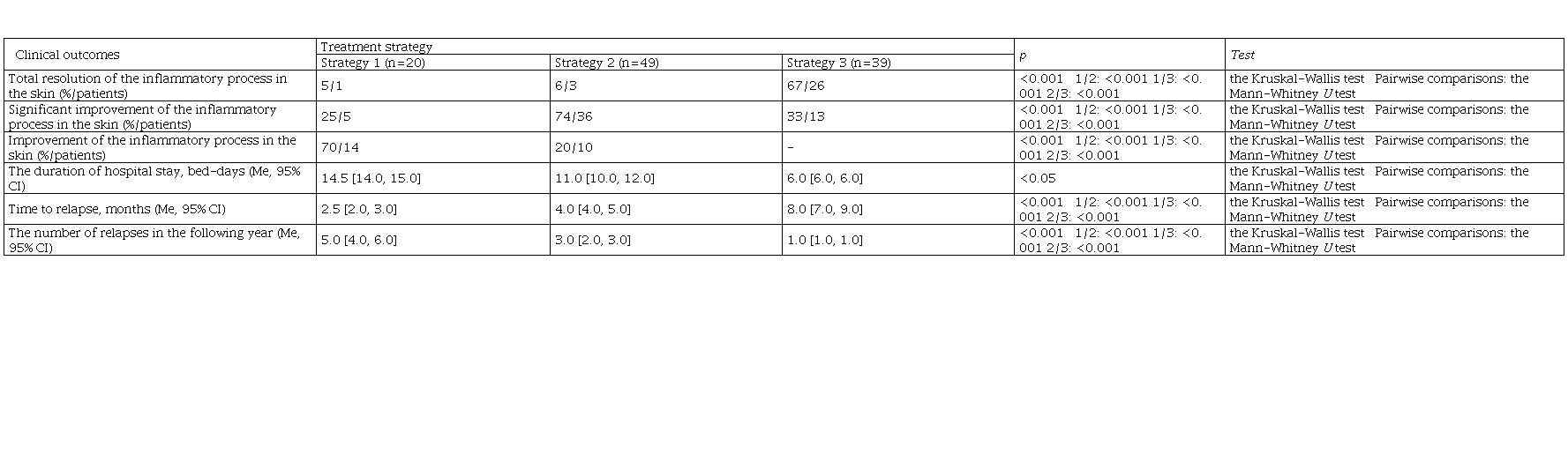
Direct medical costs of alternative treatment strategies for the management of microbial Eczema in children admitted to a 24-hour inpatient facility, per 1 patient, rubles
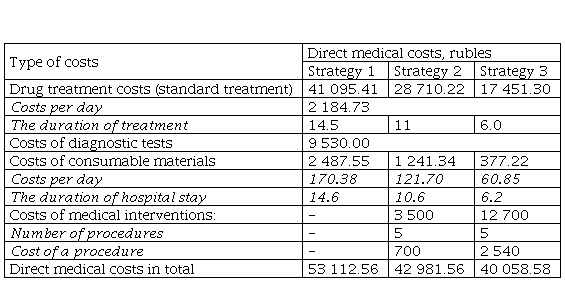
Table 4 provides information on the total costs of treatment in the cohort of patients included in the study depending on the treatment strategy and taking into account the distribution of the patients according to clinical outcome.
Direct medical costs of alternative treatment strategies for the management of microbial Eczema in children admitted to a 24-hour inpatient facility, per 1 patient, rubles.
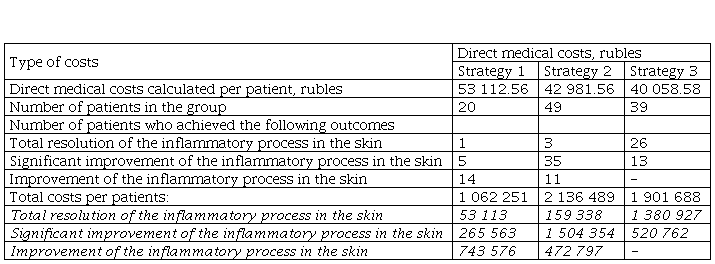
Taking into account greater clinical effectiveness and higher costs of medical interventions in case of using a new treatment method compared to the standard treatment in a subgroup of patients, we used a cost-effectiveness method in our clinical and economic analysis.
The сost-effectiveness analysis allows for a comparative assessment of medical technologies with different clinical efficacy and cost. The results of this analysis show the cost per unit of clinical outcome. Cost and effectiveness measures were calculated using a generally accepted method.
The cost-effectiveness ratio was calculated using the following formula1-3.
CER = Cost/Ef
Where CER is the cost-effectiveness ratio;
Сost is the cost of pharmacotherapy per 1 patient for the i-th treatment strategy, in rubles;
Ef is the effectiveness of the i-th treatment strategy.
In a subgroup of patients demonstrating significant improvement of the inflammatory process in the skin, the standard treatment combined with CAP dominates. It shows more effectiveness but requires lower costs than the standard treatment combined with laser therapy.
In order to assess the economic viability of the CAP method, we also carried out a budget impact analysis. This analysis allows us to compare the budget costs before and after introducing new technology (or a combination of technologies) for a specific disease. Using this treatment method demonstrates possible changes in the budget costs, allowing us to assess the acceptability of these changes for the budget and the consequences for health system financing.
While carrying out the budget impact analysis, we also assumed that the patients were treated in inpatient settings. We considered the changes in the budget holder costs in case of relapse and re-hospitalization of patients. According to the clinical study data (which we used as a basis for economic feasibility analysis), the time horizon of the study was 14.6 days, 11 days, and 6.2 days from the initiation of treatment for Strategy 1, Strategy 2 and Strategy 3, respectively. The calculations were made in a hypothetical cohort of 100 patients. While carrying out the budget impact analysis, we considered different ratios of the numbers of children with ME (Table 5).
Table 5. The ratio of the numbers of patients in whom alternative medical technologies were applied for the treatment of microbial Eczema in children.
The ratio of the numbers of patients in whom alternative medical technologies were applied for the treatment of microbial Eczema in children.
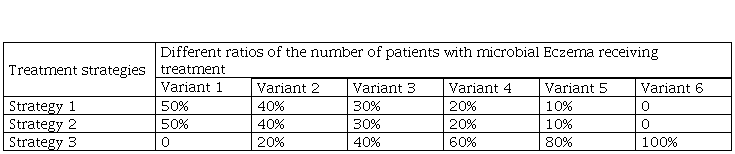
In order to assess the stability of the obtained results with respect to the change of the initial parameters, we carried out a sensitivity analysis: the evaluation of economic consequences with comparable treatment costs amounting to 53 112.56 rubles.
While carrying out the budget impact analysis, the following assumptions were made:
- in case of relapse and re-hospitalization, all patients are prescribed treatment corresponding to the strategy applied at the previous stage of their treatment.
The study's time horizon was one year starting from the moment of the patients' discharge from an in-patient facility, where they received treatment according to the three regimens.
Results and discussion
The results of our clinical study showed the advantages in the effectiveness of CAP in combination with the standard treatment as regards the rate of total and significant resolution of the inflammatory processes in the skin and, as a consequence, the duration of treatment in a 24-hour in-patient facility. In comparison with the standard treatment, the cost of 1 day of treatment in a 24-hour in-patient facility was 14 315.58 rubles, which is 651.32 rubles higher than the sum for the standard treatment combined with laser therapy and 2430.47 rubles higher compared to the sum for the standard treatment alone. The obtained results showed that total costs of medical care provided for children with ME in an-inpatient setting treated with various strategies calculated per 1 patient were as follows:
- in case of the standard treatment (Strategy 1) – 53 112.56 rubles.
- in case of the standard treatment combined with laser therapy (Strategy 2) – 42 981.56 rubles.
- in case of the standard treatment combined with CAP (Strategy 3) – 40 058.58 rubles.
The clinical and economic assessment results of the alternative strategy for microbial eczema treatment in children are presented in Table 6.
The cost-effectiveness ratio for different strategies for microbial eczema treatment in children
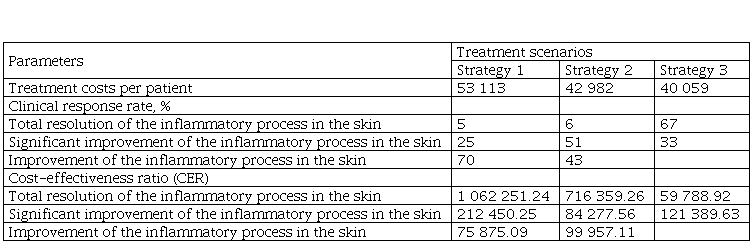

The obtained results showed that the costs per effectively treated patient who achieved total resolution of the inflammatory process in the skin were as follows: 1 062.25 thsd (Strategy 1), 716.35 thsd (Strategy 2), and 59.79 thsd (Strategy 3). In comparison with the standard treatment, the cost-effectiveness ratio is also lower when using combined treatment: 84.28 thsd (in combination with standard therapy and laser therapy) and 121.38 thsd (in combination with standard therapy and CAP).
The sensitivity analysis results assessing the impact of changes in the treatment costs on the obtained results are presented in Table 7.
The results of the sensitivity analysis of the costs for alternative treatment strategies of microbial Eczema.
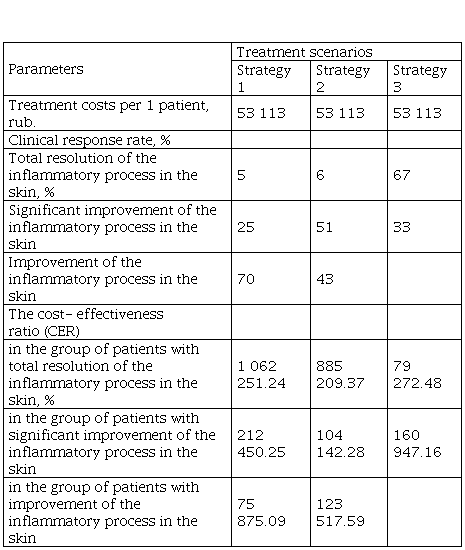
Considering the comparable cost of alternative treatment options, the use of CAP remains cost-effective.
The budget impact analysis results also showed the cost-effectiveness of using CAP for ME treatment in children (Table 8).
The introduction of a new medical technology into clinical practice: the budget impact analysis results
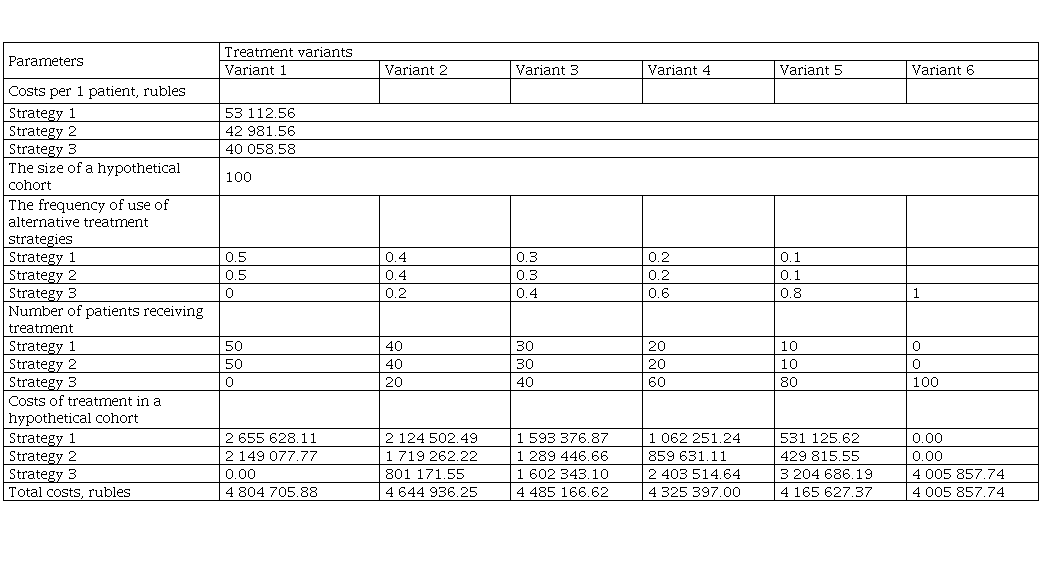
The obtained results showed that the introduction of CPA into routine clinical practice would not increase treatment costs. Even in the case of a 100% transition to new technology, the treatment costs are lower compared to the use of the standard treatment alone and the standard treatment combined with laser therapy.
Thus, the present study results showed the clinical and economic advantages of a new medical strategy - a combination of CAP with the standard treatment. The introduction of CAP into clinical practice allows to reduce the recurrence rate by 65.52% in comparison with the standard treatment and by 27.29% compared to the standard treatment in combination with laser therapy. Even though the introduction of CAP into clinical practice leads to an increase in the cost of one day of treatment, the use of CAP in routine practice will not lead to an increase in the costs due to the reduction in the length of stay. The cost-effectiveness ratio in the group of patients treated with CAP who showed total resolution of inflammatory skin processes is lower than in the group of patients receiving standard therapy and the group of patients receiving standard therapy combined with laser therapy: 59.79 vs 1 062.25 thsd and 716.35 thsd, respectively. In the group of patients with the inflammatory processes in the skin who achieved significant improvement, the standard treatment combined with CAP is superior to the standard treatment alone: 84.28 thsd and 121.38 thsd, respectively. The results of the clinical and economic assessment are stable to the changes in the costs of alternative treatment options: with a comparable cost of treatment using alternative therapy scenarios, the standard treatment combined with CAP dominates.
Conclusion
The results of budget impact analysis also showed the cost-effectiveness of CAP. Even a complete replacement of traditional treatment methods with a complete transition to new technology does not increase the costs of medical care. The results of the sensitivity analysis confirmed the reliability of the obtained data. Based on the results obtained, we can conclude that the introduction of CAP into clinical practice is cost-effective (viable) and can increase the availability of effective modern methods of microbial eczema treatment in children, which do not require high additional costs.
Ethical approval and consent to participation: patients' parents or legal guardians gave their informed consent for the inclusion of their child into the study, anonymized processing of their personal data and publication of materials.
Financing: The authors received no financial support for the research and preparation of the manuscript for publication.
Conflict of interest: The authors declare that there is no conflict of interest.
References
1. Plutnitsky A. N. Comparative assessment of the effectiveness of medical care technologies. Autoref. diss. ... candidate of Medical Sciences, Moscow, 2007 (State Research Institute of Public Health of the Russian Academy of Medical Sciences)
2. Orlov E. M., Sokolova O. N. Efficiency category in public health services system. Fundamental research. 2010; 4: 70-75. URL: http://www.fundamental-research.ru/ru/article/view?id=6762 (accessed: 16.04.2021)
3. " GOST R 57525-2017. The national standard of the Russian Federation. Clinical and economic research. General requirements" (approved and put into effect by the Order of Rosstandart dated 06.07.2017 N 655-st)
4. Russell LВ, Gold MR, Siegel JE, Daniels N, Weinstein MС, for the Panel on Cost-Effectiveness in Health and Medicine. The role of cost-effectiveness analysis in health and medicine. JAMA, 1996; 276: 1172-7
5. Greenwell TJ, Castle C, Andrich, MacDonald JT, Nicol DL, Mundy AR. Repeat urethrotomy and dilation for the treatment of urethral stricture are neither clinically effective nor cost-effective. J Urol. 2004; 172(1): 275-277.
6. Plutnitsky A. N., Malakhova L. A., Lazuk V. A. High medical technologies in ophthalmology application and evaluation of economic efficiency. Bulletin of the National Research Institute of Public Health of the Russian Academy of Medical Sciences. 2006; 2: 136-138.
7. Orkin V. F., Olekhnovich N. M. Microbial eczema: clinic, pathogenesis, treatment. Saratov, 2002.
8. Yamany T, Schwartz RA. Infectious eczematoid dermatitis: a comprehensive review. JEADV, 2015; 29(2): 203-208
9. Sokolova T.V., Malyarchuk A.P., Safonova L.A. The Strategy of Selecting Topical Therapy for Microbial Eczema. Klinicheskaya Dermatologiya i Venerologiya. 2017; 16(3):46-63 https://doi.org/10.17116/klinderma201716346-63
10. Reztsova P.A., Raznatovskiy K.I., Vashkevich A.A., Kotrekhova L.P., Elishakova L.I., Bukiya M.T. Phototherapy Efficacy Evaluation for the Patients’ Treatment with Microbial Eczema. Klinicheskaya Dermatologiya i Venerologiya. 2020;19(5):655-660. https://doi.org/10.17116/klinderma202019051655
11. Nadyrchenko N. A., Hismatullina Z. R., Nadyrchenko R. M., Mustafina G. R., Gareev E. M. The index of assessing the severity of microbial Eczema in assessing the clinical effectiveness of therapy for nummular microbial Eczema. Ufa, 2017.
12. Adaskevich V. P. Diagnostic indexes in dermatology. - M.: Panfilov publishing house: BINOM. Laboratory of Knowledge, 2014 – - 352 p
13. Zambrano AM, Córdova MV, Hidrobo AM, Pico DP, Yamunaque YT, Uzhca BS, Cantos GY, Cardona DA. Implicaciones de lacuarentena por COVID-19 en la regulación del metabolismo de la glucosa. Diabetes Internacional. 2020;12(1):1-5.
14. Cordero PM, Crespo DO, Cáceres WS, Choez KM, Nauñay DC, Dávila CS, Carrillo AO, Morocho GC, Calero JR. Lesión pancreática causada por Covid-19:¿ es la diabetes una secuela de la infección?. Diabetes Internacional. 2020;12(1):34-8. DOI:10.5281/zenodo.4381011
15. Albdairi AA, Al-Shalah MA. Study of the association between the congenital uterine septum and polycystic ovarian syndrome in infertility tertiary center in Iraq. Archivos Venezolanos de Farmacologia y Terapéutica. 2021;40(4):384-8. http://doi.org/10.5281/zenodo.5225145
16. Tatyana S, Raisovna IV. Efficacy and safety of the indirect anticoagulant warfarin in its dosage based on the results of pharmacogenetic testing. Archivos Venezolanos de Farmacologia y Terapéutica. 2021;40(4):451-4.
