Artigo Original
Hand hygiene knowledge among nursing professionals during a pandemic: insights from a cross-sectional study in Brazil
Conhecimento sobre higiene das mãos entre profissionais de enfermagem durante uma pandemia: insights de um estudo transversal no Brasil
Conocimiento de higiene de manos entre profesionales de enfermería durante una pandemia: perspectivas de un estudio transversal en Brasil
Hand hygiene knowledge among nursing professionals during a pandemic: insights from a cross-sectional study in Brazil
Revista de Epidemiologia e Controle de Infecção, vol. 14, núm. 1, pp. 46-57, 2024
Universidade de Santa Cruz do Sul

Esta obra está bajo una Licencia Creative Commons Atribución 4.0 Internacional.
Recepción: 17 Julio 2023
Aprobación: 22 Diciembre 2023
Abstract: Background and Objectives: hand hygiene (HH) is a crucial safety practice, but lack of knowledge can hinder compliance. The objective was to measure and assess the knowledge of nursing professionals who provided care during the COVID-19 pandemic regarding HH and to verify the association between HH knowledge and professional category and regions in Brazil. Methods: an observational study was conducted from November 2020 to December 2021 involving 493 nursing professionals from all regions of Brazil. Data collection was caried out using Google Forms® and social media platforms. The Hand Hygiene Knowledge Test for Healthcare Professionals was used, and results were analyzed descriptively. Pearson’s chi-square test (X2) and Fisher’s exact test were employed to assess associations. Results: among the participants, the majority (74.7%) had limited or subpar knowledge of HH. Nurses had a higher level of knowledge compared to nursing assistants and licensed practical nurses. Associations were found between professional category and correct answers regarding microorganism destruction time and the type of HH to be used. Conclusion: Brazilian nursing professionals had limited knowledge of HH, with nurses displaying a higher level of knowledge compared to nursing assistants and licensed practical nurse. Continuous education and guidance are necessary to improve HH practices among the nursing staff.
Keywords: SARS-CoV-2, Hand Hygiene, Nursing staff, Infection Control, Continuous Education.
Resumo: Justificativas e Objetivos: a higiene das mãos (HM) é uma prática crucial para a segurança, mas a falta de conhecimento pode prejudicar a adesão. Este estudo avaliou o conhecimento dos profissionais de enfermagem que prestaram cuidados durante a pandemia de Covid-19 em relação à HM e explorou a associação entre o conhecimento de HM, categoria profissional e regiões no Brasil. Métodos: um estudo observacional foi conduzido de novembro de 2020 a dezembro de 2021 envolvendo 493 profissionais de enfermagem de todas as regiões do Brasil. A coleta de dados foi realizada usando o Google Forms® e plataformas de mídia social. Foi utilizado o Teste de Conhecimento de Higiene das Mãos para Profissionais de Saúde, e os resultados foram analisados descritivamente. O teste qui-quadrado de Pearson (X2) e o teste exato de Fisher foram empregados para avaliar as associações. Resultados: entre os participantes, a maioria (74,7%) tinha conhecimento limitado ou insuficiente sobre HM. Os enfermeiros apresentaram um nível mais elevado de conhecimento em comparação com os auxiliares e técnicos de enfermagem. Foram encontradas associações entre a categoria profissional e respostas corretas sobre o tempo de destruição de microrganismos e o tipo de HM a ser utilizado. Conclusão: os profissionais de enfermagem brasileiros possuíam conhecimento limitado sobre HM, sendo que os enfermeiros apresentaram um nível mais elevado de conhecimento em comparação com os auxiliares e técnicos de enfermagem. Educação contínua e orientação são necessárias para melhorar as práticas de HM entre a equipe de enfermagem.
Palavras-chave: SARS-CoV-2, Higiene das Mãos, Equipe de Enfermagem, Controle de Infecções, Educação Contínua.
Resumen: Justificación e Objetivos: la higiene de manos (HM) es una práctica de seguridad crucial, pero la falta de conocimiento puede dificultar el cumplimiento. Este estudio evaluó el conocimiento de los profesionales de enfermería que brindaron atención durante la pandemia de Covid-19 en relación con la HM y exploró la asociación entre el conocimiento de HM, la categoría profesional y las regiones en Brasil. Métodos: se realizó un estudio observacional desde noviembre de 2020 hasta diciembre de 2021 que incluyó a 493 profesionales de enfermería de todas las regiones de Brasil. La recopilación de datos se realizó utilizando Google Forms® y plataformas de redes sociales. Se utilizó el Test de Conocimiento de Higiene de Manos para Profesionales de la Salud, y los resultados se analizaron de manera descriptiva. Se emplearon la prueba chi-cuadrado de Pearson (X2) y la prueba exacta de Fisher para evaluar las asociaciones. Resultados: entre los participantes, la mayoría (74,7%) tenía conocimiento limitado o deficiente de HM. Las enfermeras tenían un nivel de conocimiento más alto en comparación con los auxiliares y técnicos de enfermería. Se encontraron asociaciones entre la categoría profesional y las respuestas correctas sobre el tiempo de destrucción de microorganismos y el tipo de HM que debía utilizarse. Conclusión: los profesionales de enfermería brasileños tenían un conocimiento limitado de HM, siendo que las enfermeras mostraban un nivel de conocimiento más alto en comparación con los auxiliares y técnicos de enfermería. Se requiere educación continua y orientación para mejorar las prácticas de HM entre el equipo de enfermería.
Palabras clave: SARS-CoV-2, Desinfección de Manos, Equipo de Enfermería, Control de Infecciones, Educación Continua.
INTRODUCTION
COVID-19 is a highly contagious illness caused by the SARS-CoV-2 virus, capable of causing acute respiratory infections, severe illness, and fatalities.1,2 The virus is mainly transmitted through respiratory droplets and aerosols,3 and can even be transmitted through fecal matter.4 Previous studies have demonstrated that the virus can contaminate a variety of surfaces, including chairs, tables, bed rails, stethoscopes, toilets, and floors.1,2,4 Environmental contamination can amplify the chain of transmission.1,2,4 Touching contaminated surfaces and subsequent contact with mucous membranes can increase the risk of contamination and virus transmission.5 Additionally, touching the face can serve as a potential vector for self-inoculation of various pathogens.6 The human face provides a favorable environment for the survival of enveloped viruses like influenza and coronaviruses,7 and the SARS-CoV-2 virus has been found to remain viable on human skin for approximately 9 hours.8
Considering the characteristics of SARS-CoV-2, as well as other viruses, nursing staff exposure during patient care is inevitable, as healthcare requires direct contact with patients using hands, which can serve as vehicles for microorganism transmission.9 Thirty percent of deaths among nursing professionals due to COVID-19 occur in Brazil.10 The nursing staff works on the frontlines of care in various sectors and has faced challenges such as a shortage of personal protective equipment, supplies, and work overload.11 Given the potential severity of COVID-19 and other diseases,1,2 patients often require intensive care that involves aerosol-generating procedures and secretion management, such as endotracheal suctioning performed by nurse.12
Hand hygiene (HH) is a critical safety measure designed to eliminate dirt and microorganisms.13 Properly conducted, HH has the ability to deactivate several viruses, including SARS-CoV-2, thus decreasing the risk of contact transmission.8 HH is effective in pre-venting the transmission of other pathogens and significantly reducing healthcare-associated infections (HAI) that worsen hospitalized patients’ condition.14 HAI transmission among patients depends largely on the contamination of healthcare professionals’ hands, despite there being various risk factors for the spread of infections among patients.15 HAI are preventable, but they remain one of the most common adverse effects of healthcare, leading to increased hospitalization time, mortality, and healthcare costs.16
Although care and safety have been compromised due to work overload, lack of resources, and knowledge,17 there is evidence that compliance with HH during the pandemic has shown significant improvement among healthcare professionals compared to previous years.18 This can be explained by the scientific race to manage the pandemic and its impacts, contributing to new discoveries and investments.19 However, improvements in HH compliance among healthcare professionals during the early stages of the pandemic were not sustained, leading to a significant decline in 2021.20 Therefore, it is important to assess the impact of the COVID-19 pandemic on nursing professionals’ knowledge regarding HH practice, as this practice is always valued in infection control. In light of the above, professionals’ knowledge, attitudes, and practice regarding this health-promoting behavior should be constantly reinforced.
HH is influenced by cultural aspects, which can affect human behavior.13 It is crucial to assess nursing professionals’ knowledge during the COVID-19 pandemic, given the importance of HH in mitigating the spread of SARS-CoV-2. However, it is important to take into consideration the cultural and regional differences in the study, which can impact the level of knowledge among professionals regarding HH. This study included nursing professionals from all levels of care because it is known that pre-symptomatic and asymptomatic patients can transmit SARS-CoV-2.21
Lack of knowledge is a barrier to HH compliance,7 which is why this study not only assessed sufficient knowledge but also identified knowledge gaps among professionals by regions in Brazil and professional categories. Thus, the research question was whether nursing professionals’ knowledge regarding HH during the COVID-19 pandemic is adequate or deficient. These initiatives will not only benefit healthcare professionals’ safety by reducing the spread of infections, including SARS-CoV-2, but also enhance the capacity to respond to future public health emergencies, minimizing the risks of pathogen transmission in healthcare settings. In light of this, the aim was to measure and assess the knowledge of nursing professionals who provided care during the COVID-19 pandemic regarding HH and to ascertain the association between HH knowledge and professional categories and regions in Brazil.
METHODS
Study Design
This is an observational cross-sectional study22 that followed the STrengthening the Reporting of OBservational studies in Epidemiology (STROBE) and the Checklist for Reporting Results of Internet E-Surveys (CHERRIES) presentation criteria.
Sample and Procedures
The sample for this study consisted of nursing professionals (nursing assistants, licensed practical nurse, and nurses) working in nursing care across five different regions of Brazil (South, Southeast, Midwest, North, and Northeast). Participant recruitment was voluntary and conducted online through social media platforms such as Facebook®, Instagram®, LinkedIn®, and WhatsApp® from November 23, 2020 to December 23, 2021. Invitations were extended to relevant nursing groups and involved collaboration with nursing organizations. The researcher identified themselves and provided details about the research, giving a brief account of the objectives, risks, and contributions to nursing practice. The invitation was posted weekly, reaching all five regions of Brazil. As an exclusion criterion, not being a nursing professional and not currently practicing nursing at the time of the research was adopted.
The sample size was determined by convenience, corresponding to the maximum number of nursing professionals who agreed to participate in the research during the 13-month recruitment period. Professionals involved in nursing care during the COVID-19 pandemic at the time of data collection, as self-declared by participants and who belonged to relevant nursing groups and collaborated with nursing organizations, were included. The snowball method was employed, in which the link was shared and forwarded among groups. Participants were informed about the research objectives and methods and were ensured the right to withdraw at any time. To avoid duplicate answers, participants provided their email addresses. There was no identification of nursing professionals, and anonymity was preserved.
Data Collection and Questionnaires
Data collection was conducted through a self-administered questionnaire provided online using the free platform Google Forms®. The questionnaire comprised two distinct sections. One section aimed to assess sociodemographic and work-related characterization, containing 12 objective multiple-choice questions. These questions encompassed information about gender, age, educational level, number of current employments, nature of the workplace (public or private), years of professional experience, and nursing category. The other section aimed to assess professionals’ technical and scientific knowledge regarding HH, comprising 47 multiple-choice, true or false, and yes or no questions. The instrument utilized to assess professionals’ knowledge was the Hand Hygiene Knowledge Test for Healthcare Professionals, which was developed and validated by the Brazilian Health Regulatory Agency (ANVISA - Agência Nacional de Vigilância Sanitária) and the Pan American Health Organization (PAHO) in 2008.
Data Analysis
The collected data were analyzed using Google Forms® and subjected to descriptive statistical analyses, presented as absolute and relative frequencies. Considering statistical significance when p-value ≤ 0.05, association tests (Pearson’s chi-square test (X²) and Fisher’s exact test) were performed between the number of correct answers for each question and the following variables of interest: professional category (nurses and nursing assistants and licensed practical nurses) and regions of Brazil (South, Southeast, Midwest, Northeast, and North). To assess knowledge of HH and calculate a total score, the Positivity Index (PI) was employed as an interpretive approach, considering the number of correct answers as indicators of positive outcomes. The PI was interpreted as follows: desirable (100% positivity); adequate (between 99% and 90% positivity); safe (between 89% and 80% positivity); borderline (between 79% and 71% positivity); and poor (70% or less positivity).23,24 Thus, one point was assigned for each correct question regarding professionals’ knowledge of HH; the final score was calculated by summing up the points obtained; and a percentage was assigned and categorized according to the PI. To examine the relationship between the positivity level and professional category, the Adequate and Safe indices were combined, while the Borderline and Poor indices were grouped together. Statistical analysis was performed using the Statistical Package for the Social Sciences (SPSS) version 23 software.
Ethical Aspects
This study received approval from the Research Ethics Committee of the Escola de Enfermagem de Ribeirão Preto, Universidade de São Paulo (REC-EERP/USP), with Certificate of Presentation for Ethical Consideration (CAAE - Certificado de Apresentação para Apreciação Ética) n° 38623520.6.0000.5393 and Protocol number 4381042 approved on November 5, 2020. All participants were informed about the purposes and methods used in the study, emphasizing their right to withdraw from the research at any time. The research was conducted following the ethical standards required - Resolutions 466/2012, 510/2016 and 580/2018 from the Ministry of Health.
RESULTS
Sociodemographic data were collected from 493 nursing professionals from all regions of Brazil who completed the Google Forms® questionnaire. The majority of the sample was from São Paulo state (330/66.8%), followed by Rio de Janeiro state (46/9.3%), representing predominantly the Southeast region (74.6%). Regarding institutional profiles, most professionals worked at general hospitals (219/44.3%), followed by home care services (47/9.5%), emergency units (45/9.1%), and university hospitals (44/8.9%). Concerning gender composition, the majority of participants were female (75.8%). Regarding employment status, most participants held a single job (392/79.4%), while 4% had three simultaneous nursing jobs. It was observed that only in the South and North regions were there more licensed practical nurse than nurses (Table 1).
| Variables | Generaln (%) | Professional category Regions of Brazil n ( %) n (%) | ||||||
| NURSE | TECH | South | Southeast | Midwest | Northeast | North | ||
| 1. Gender | ||||||||
| Female | 374 (75.8) | 267 (74.6) | 107 (79.3) | 20 (80) | 297 (74.6) | 22 (78.6) | 32 (86.5) | 3 (60) |
| Male | 119 (24.2) | 91 (25.4) | 28 (20.7) | 5 (20) | 101 (25.4) | 6 (21.4) | 5 (13.5) | 2 (40) |
| 2. Age group | ||||||||
| 18 to 24 | 105 (21.3) | 79 (22.1) | 26 (19.3) | 7 (28) | 89 (22.4) | 3 (10.7) | 5 (13.5) | 1 (20) |
| 25 to 29 | 109 (22.2) | 93 (26) | 16 (11.9) | 5 (20) | 82 (20.6) | 10 (35.7) | 12 (32.4) | 1 (20) |
| 30 to 39 | 157 (31.8) | 118 (33) | 39 (28.9) | 7(28) | 127 (31.9) | 11 (39.3) | 11 (29.7) | 2 (40) |
| 40 to 49 | 100 (20.2) | 57 (15.9) | 43 (31.9) | 5 (20) | 85 (21.4) | 3 (10.7) | 5 (13.5) | 1 (20) |
| 50 to 59 | 22 (4.5) | 11 (3.1) | 11 (8.1) | 1 (4) | 15 (3.8) | 1 (3.6) | 4 (10.8) | 1 (20) |
| 3- Level of education | ||||||||
| Elementary school (9th year) | 2 (0.4) | 0 | 2 (1.5) | 0 | 2 (0.5) | 0 | 0 | 0 |
| High school or secondary school | 94 (19) | 2 (0.6) | 92 (68.1) | 12 (48) | 71 (17.7) | 3 (10.7) | 6 (16.2) | 2 (40) |
| Higher education, teaching or bachelor’s degree | 148 (30) | 112 (31.3) | 36 (26.7) | 3 (12) | 128 (32.2) | 7 (25) | 9 (24.3) | 1 (20) |
| Graduate, masters or doctoratal degrees | 249 (50.4) | 244 (68.2) | 5 (3.7) | 10 (40) | 197 (49.5) | 18 (64.3) | 22 (59.5) | 2 (40) |
| 4- Number of workplaces | ||||||||
| 1 | 392 (79.4) | 289 (80.7) | 103 (76.3) | 20 (80) | 318 (19.9) | 22 (78.6) | 27 (73) | 5 (100) |
| 2 | 81 (16.4) | 55 (15.4) | 26 (19.3) | 4 (16) | 66 (16.6) | 5 (17.9) | 6 (16.2) | 0 |
| 3 | 20 (4) | 14 (3.9) | 6 (4.4) | 1 (4) | 14 (3.5) | 1 (3.6) | 4 (10.80 | 0 |
| 5. Nature of the institution | ||||||||
| Public | 195 (39.5) | 145 (40.5) | 50 (37) | 9 (36) | 156 (39.2) | 8 (28.6) | 19 (51.4) | 3 (60) |
| Private | 245 (49.6) | 182 (50.8) | 63 (46.7) | 9 (36) | 204 (51.3) | 17 (60.7) | 13 (35.1) | 2 (40) |
| Public, private | 53 (10.7) | 31 (8.7) | 22 (16.3) | 7 (28) | 38 (9.5) | 3 (10.7) | 5 (13.5) | 0 |
| 6. Length of service (in years) | ||||||||
| < 1 | 118 (23.9) | 97 (27.1) | 21 (15.6) | 1 (4) | 95 (23.9) | 9 (32.1) | 12 (32.4) | 1 (20) |
| Between 1 to 2 | 75 (15.2) | 52 (14.5) | 23 (17) | 4 (16) | 61 (15.3) | 4 (14.3) | 6 (16.2) | 0 |
| Between 3 to 4 | 60 (12.1) | 42 (11.7) | 18 (13.3) | 6 (24) | 44 (11.1) | 7 (25) | 3 (8.1) | 0 |
| Between 5 to 6 | 34 (6.9) | 29 (8.1) | 5 (3.7) | 2 (8) | 29 (7.3) | 0 | 3 (8.1) | 0 |
| Between 7 to 8 | 34 (6.9) | 23 (6.4) | 11 (8.1) | 2 (8) | 27 (6.8) | 3 (10.7) | 2 (5.4) | 0 |
| Between 9 to 10 | 43 (8.7) | 28 (7.8) | 15 (11.1) | 1 (4) | 38 (9.5) | 2 (7.1) | 1 (2.7) | 1 (20) |
| Between 11 to 15 | 45 (9.1) | 31 (8.7) | 14 (10.4) | 5 (20) | 35 (8.8) | 1 (3.6) | 3 (8.1) | 1 (20) |
| Between 16 to 20 | 42 (8.5) | 31 (8.7) | 11 (8.1) | 3 (12) | 36 (9) | 0 | 1 (2.7) | 2 (40 |
| Between 21 to 30 | 40 (8.1) | 25 (7) | 15 (11.1) | 1 (4) | 31 (7.8) | 2 (7.1) | 6 (16.2) | 0 |
| ≤ 31 | 2 (0.4) | 97 (27.1) | 2 (1.5) | 1 (4) | 2 (0.5) | 0 | 0 | 0 |
| 7. Profession | ||||||||
| Nurse | - | - | - | 10 (40) | 291 (73.1) | 24 (85.7) | 31 (83.8) | 2 (40) |
| Licensed practical nurse | 15 (60) | 82 (20.6) | 4 (14.3) | 6 (16.2) | 3 (60) | |||
| Nursing assistant | 0 | 25 (6.3) | 0 | 0 | 0 | |||
Table 2 presents the absolute frequency (n) and relative frequency (%) of correct answers to the HH knowledge questionnaire by nursing professionals in the five regions of Brazil, grouped by professional category, and Fisher’s exact test was performed to verify the association between correct answers and professional category. Regarding the minimum time to destroy microorganisms on hands, 65.6% of professionals answered correctly, and it is important to highlight that there was a significant difference between the correct answer and professional category, with 69.6% of nurses answering correctly compared to 55.6% of nursing assistants and licensed practical nurses. As for the regions of Brazil, when performing the chi-square test, no significant difference was found in professionals’ correct answers regarding HH knowledge. Of correct answers regarding the type of HH required in different situations by nursing professionals in the five regions of Brazil, grouped by professional category, and the association between correct answers and professional category. A difference was observed between nurses and nursing assistants and licensed practical nurses in their answers regarding the type of HH required before writing in patients’ medical records (p=0.004), before patient contact (p=0.018), upon returning to the unit after lunch (p=0.002), when leaving patients (p=0.004), and after visible blood exposure (p=0.006), which are highlighted in the table with an asterisk (*).
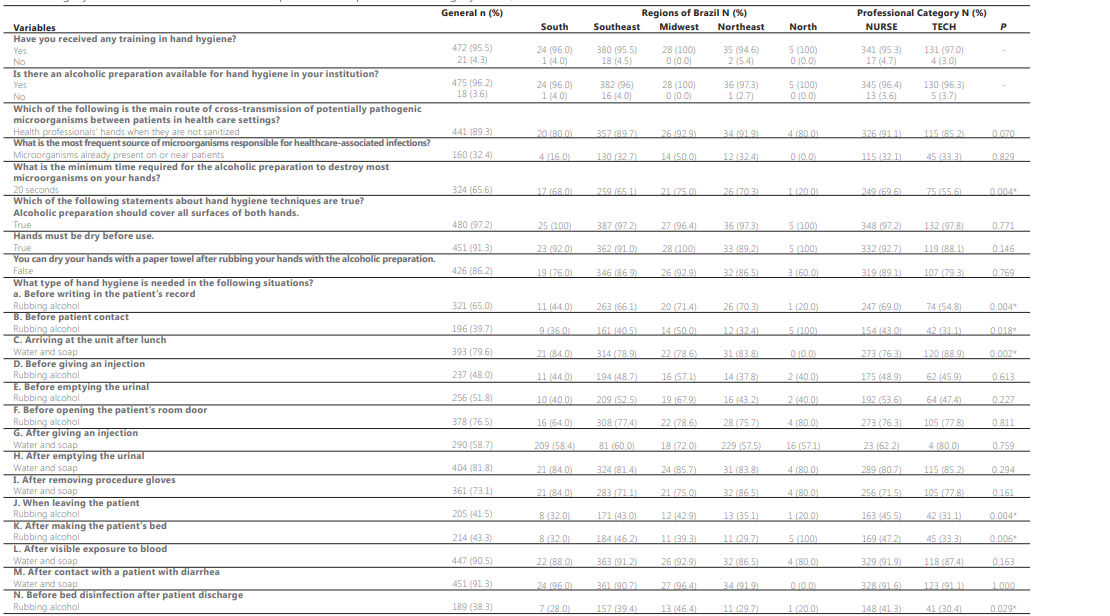
Source: authors’ data. TECH = Nursing Assistants and Licensed Practical Nurses; *significance level: p < 0.05.
In the chi-square test, there was only an association found between the correct answers and the different regions of Brazil regarding surfaces that can become contaminated with microorganisms and transfer them to patients if hands are not properly sanitized before contact. In the question regarding intact skin of another patient (p=0.029), 60% of professionals from the North region answered “no” while 88.2% of professionals from the Southeast region answered “yes”. In the question regarding the patients themselves (p=0.048), a significant difference was also observed as well as in the question about the bedside table of another patient (p=0.016). No significant difference was found between the correct answers and the different professional categories. Table 3 presents the correct answers of nursing professionals with the association between professional categories (nurses and nursing assistent/licensed practical nurse) regarding the use of alcohol-based hand rub and HH.
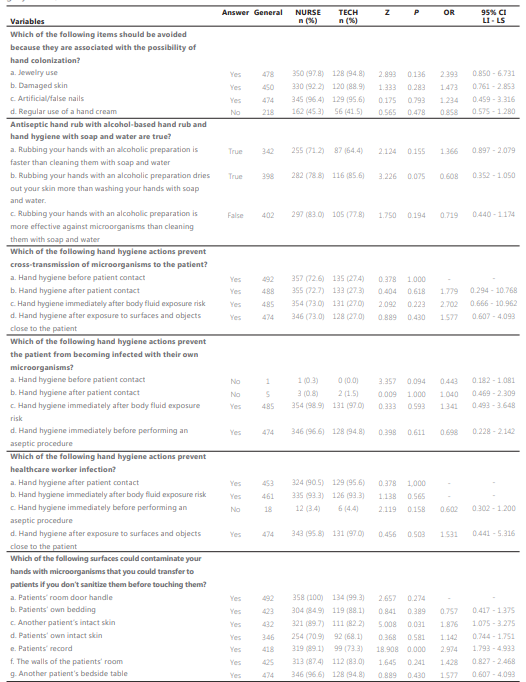
Source: authors’ data. TECH = nursing assistants and licensed practical nursea; *significance level: p < 0.05
In Figure 1, a total score of correct answers regarding knowledge of HH was assigned, and the correct answers were grouped by professional and classified according to the PI. No professional was classified as desirable (100%), while only 4 professionals were classified as adequate (between 99% and 90%). The majority of professionals (74.7%) were classified as borderline or poor in terms of knowledge of HH.
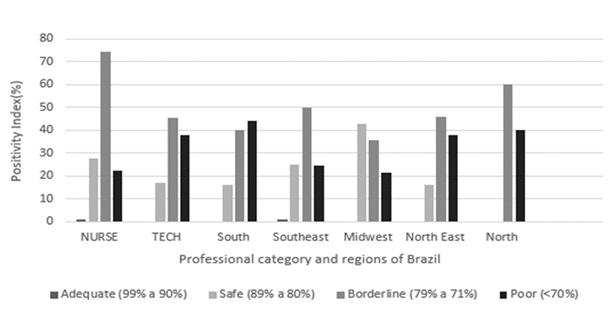
Figure 1
Positivity Index about knowledge about Hand Hygiene. Brazil, 2023
In Figure 2, adequate and safe PI (between 99% and 80%) were grouped together, while borderline and poor groups (<79%) were grouped separately to verify the association between professional categories and visualize where significant differences occurred. The graph reveals that nurses had a higher PI between adequate and safe compared to nursing assistents and licensed practical nurses, while the latter category had a higher index in borderline and poor groups. When checking the association between regions and grouping (adequate/safe and borderline/poor), only the Southeast region showed an association [X²=6.258 (1); p=0.014].
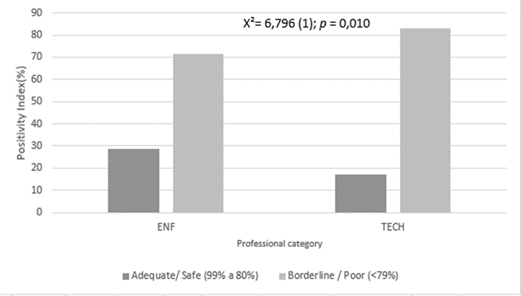
Figure 2
Positivity Index about knowledge about hand hygiene among professional categories (nurses/nursing assistants and licensed practical nurses (TECH)). Brazil, 2023.
DISCUSSION
Our aim was to assess nursing professionals’ knowledge regarding HH during the COVID-19 pandemic. These professionals reported receiving training on HH, and the institution provided hand sanitizer for practice. Although a minority correctly identified the most common source of infection-related microorganisms, the majority understood the minimum time required to eliminate these microorganisms from hands. When examining the association between this knowledge, professional categories, and regions in Brazil, significant differences were noted: nurses provided more correct answers compared to nursing assistants and licensed practical nurses. However, regions in Brazil showed no association with correct answers. While most professionals acknowledge the importance of HH, there were statistically significant differences in understanding the type of hygiene needed in different situations, especially before patient contact, upon arrival at the unit after lunch, before leaving the patient, and after visible blood exposure.
Regarding questions about contamination routes, there was no association between correct answers and professional categories. When analyzing the total score of correct answers on HH knowledge, scores were grouped using the PI. No professional was classified as desirable, and the majority fell into the borderline or poor categories. Although there were no significant differences between Brazilian regions, a notable association was observed among professional categories. Nurses demonstrated a higher adequate and safe PI compared to nursing assistants and licensed practical nurses, who showed higher ratings in borderline and poor categories. These outcomes highlight the need for nursing professionals to enhance their overall understanding of HH, including knowledge of common sources of HAI and appropriate HH practices in diverse scenarios. HH remains one of the most effective and cost-efficient strategies for controlling HAI, requiring correct application, especially during pandemics and at all times.3,13,25
HH is one of the key pillars in HAI prevention and control and crucial to prevent HAI and reduce their potential impact. Nursing professionals play a vital role in preventing the spread of infections through their compliance with HH practices.3,13,25 Therefore, it is essential for nursing professionals to have knowledge about infection prevention and control measures, especially regarding HH.26–28 However, despite the importance of this issue, many professionals still do not believe in the effectiveness of these measures, which can result in failures in implementing preventive practices. Therefore, it is important to invest in ongoing training for nursing professionals and promote a patient safety culture. Regarding the minimum time required for antiseptic hand rubbing, 65.6% of professionals answered correctly about the time needed to destroy the majority of microorganisms with alcohol-based preparations. Although a study reported that participants stated that one minute was necessary for this HH procedure,28 it is important to highlight that one minute is not the recommended minimum time. Additionally, a significant difference was found in the answers about the minimum rubbing time with alcohol-based preparations and whether hand drying can be done after rubbing with alcohol-based preparations between nurses and licensed practical nurses, indicating that higher-level professionals have a more solid theoretical foundation in this area.28,29
Although the majority of licensed practical nurses answered correctly, many professionals, regardless of professional category or region in Brazil, still believe that the most frequent source is the hospital environment, rather than the patient and their surroundings. This indicates the need for guidance and monitoring of nurses regarding HH practices for the healthcare staff, patients, and family members.28,30–32 Many professionals report performing HH with soap and water when they could be using alcohol-based hand rub. The knowledge gap regarding the use of alcohol-based preparations can be justified by the fact that simple handwashing with soap and water is still the preferred method among healthcare professionals.33,34 However, it is important to highlight that, during the COVID-19 pandemic, the use of alcohol-based products was strongly encouraged everywhere, especially in healthcare settings.33,34 It is worth noting that different regions of Brazil have their own cultural peculiarities. However, it is crucial to emphasize that HH protocols and recommendations are adopted based on both national and international guidelines. Regarding HH training, it is noteworthy that the vast majority of professionals reported having received training on this topic.29,31,35
The COVID-19 pandemic has brought to light the importance of HH as a preventive measure to avoid the spread of infectious diseases. However, studies conducted during the pandemic have shown the need for approaches to improve nursing professionals’ knowledge about HH.12,36,37 A study conducted in an Adult Intensive Care Unit before the COVID-19 pandemic revealed that, after providing care, the moment when professionals performed HH the most was when they had contact with patients, prioritizing only their own safety.38This highlights the need to implement strategies for HH, such as easy access to alcohol-based preparations and other supplies intended for this purpose, professional education, visual re-minders in strategic locations, and monitoring of HH practices with performance feedback to professionals. These actions are likely to improve overall compliance with practice. The World Health Organization has developed an electronic guide for implementing the multimodal strategy to improve HH, which includes key elements such as staff instruction and motivation programs, adoption of alcohol-based products as the gold standard, use of performance indicators, and strong commitment from all stakeholders, including frontline staff, managers, and healthcare leaders.39 It is important to note that, despite 95.5% of participants in the studies having received HH training, there are knowledge gaps in this topic among the investigated staff. This indicates the need to encourage measures aimed at improving compliance with HH, especially in future situations that may require similar preventive measures. It is essential for nursing professionals to have a comprehensive understanding of the importance of HH as one of the primary measures against HAI, with a particular emphasis on pandemics.12,29,36,38
The study in question points to the need for intensifying educational strategies and monitoring indicators to enhance nursing staff’s knowledge and ensure proper HH implementation. When it comes to general knowledge about HH, no nursing professional was classified as desirable, and only a very small percentage was considered adequate. Based on the results obtained in recent studies, there is a clear need to expand nursing staff’s knowledge regarding HH and, consequently, improve the proper implementation of this practice.27,30,34,35 Nurses demonstrated more adequate knowledge compared to nursing assistants and licensed practical nurses. The longer training duration and the ongoing demands within the nursing profession may have contributed to their enhanced understanding. This highlighting the importance of nurses’ leadership in the staff, always encouraging and teaching the staff about the most current and appropriate protocols.40
The assessment of nursing professionals’ knowledge about HH is of utmost importance to ensure patient safety, especially during pandemics like the case of COVID-19. In this regard, our research conducted in all regions of Brazil revealed a knowledge that is borderline to poor, even though there is a low representativeness of the regions, the sample is heterogeneous. Although using a self-assessment questionnaire at a time when there were incentives, investments, fear, and motivation for HH showed a knowledge far below the desirable, indicating a concern in other moments when HH is not as evident.41,42 We can have a snapshot of professionals’ reality in Brazil during the pandemic, which was a delicate and important period for controlling HAI, especially COVID-19. Thus, it is crucial for healthcare professionals to be properly trained and aware of the importance of HH in preventing disease transmission. Studies like this can provide valuable information for implementing patient safety policies and practices in hospitals and healthcare units worldwide as well as healthcare professional safety, especially during pandemics.43,44
Some limitations should be considered when interpreting our results, such as convenience sample, online data collection, and the specific context of the study. However, it provides significant contributions to HH, with valuable insights for nursing professionals and a basis for interventions and policies. The findings encourage future research on the effectiveness of HH in preventing HAI.
Considering the presented results, it is possible to conclude that the training of nursing professionals regarding HH should be continuous and assessed in order to ensure the desired knowledge of HH protocols and reduce the risk of HAI. It is necessary to recognize that the nursing staff plays a crucial role in promoting HH not only for themselves but also for the community at large. Therefore, investments in training and awareness should be prioritized to ensure patients and healthcare professional safety at all times, with even greater emphasis during pandemics.
Nursing professionals, in general, have a limited and poor knowledge of HH. It is important to note that there are differences among professional categories and in some aspects across regions in Brazil. The nursing staff should be constantly trained and guided in infection control and prevention, raising awareness about the importance of HH knowledge in crucial moments such as pandemics, as Florence Nightingale already emphasized in the early days of nursing, to ensure the quality of healthcare, prevent HAI, and ensure healthcare professional safety. This analysis will enable the development of more accurate and effective strategies for improving HH knowledge and practice, thereby reducing the spread of SARS-CoV-2 and other pathogens.
Additionally, to enhance the knowledge and practice of HH among nursing professionals, it is essential to provide specific recommendations. This may include implementing educational programs, practical training sessions, regular assessments, and feedback mechanisms. Emphasizing the impact on patient safety is crucial, highlighting the consequences of inadequate HH practices, such as increased rates of HAI, patient morbidity and mortality, and the economic burden on healthcare systems. Connecting with global initiatives and guidelines, such as the World Health Organization’s “My 5 Moments for Hand Hygiene” approach, reinforces the importance of addressing the identified knowledge gaps. By aligning the study’s findings with internationally recognized standards, the conclusion emphasizes the urgency of improving knowledge and HH practices.
REFERENCES
1. WHO. World Heal Organ WHO-China Jt Mission Coronavirus. 2020. Avaliable: https://www.who.int/publications/i/item/report-of-the-who-china-joint-mission-on-coronavirus-disease-2019-(covid-19)
2. Carlos WG, DelaCruz CS, Cao B et al. COVID-19 disease due to SARS-CoV-2 (novel coronavirus). Am J Respir Crit Care Med. 2020;201(4):P7–8. Avaliable: https://www.atsjournals.org/doi/pdf/10.1164/rccm.2014P7
3. WHO. World Heal Organ WHO-China Jt Mission Coronavirus Dis 2019. 2020. Avaliable: https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf
4. Ong SWX, Tan YK, Chia PY, et al. Air, surface environmental, and personal protective equipment contamination by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) from a symptomatic pa-tient. Jama. 2020;323(16):1610–2. doi: https://doi.org/10.1001/jama.2020.3227
5. Yang C. Does hand hygiene reduce SARS-CoV-2 transmission? Graefe’s Arch Clin Exp Ophthalmol. 2020;258:1133–4. Avaliable: https://link.springer.com/article/10.1007/s00417-020-04652-5
6. Kwok YLA, Gralton J, McLaws M-L, et al. Se toucher le visage: une habitude fréquente qui a des conséquences sur l’hygiène des mains. American journal of infection control. Elsevier. 2015. Avaliable: file:///C:/Users/jessi/Downloads/Setoucherlevisageunehabitudefrquentequiadesconsquencessurlhyginedesmains.Americanjournalofinfectioncontrol.Elsevier.2015.KwokYenLeeAngelaetGraltonJanetMcLawsMary-Louise_traducteur_Dufour_Olivier.pdf
7. Przekwas A, Chen Z. Washing hands and the face may reduce COVID-19 infection. Med Hypotheses. 2020;144:110261. doi: https://doi.org/10.1016/j.mehy.2020.110261
8. Hirose R, Ikegaya H, Naito Y, et al. Survival of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and influenza virus on human skin: importance of hand hygiene in coronavirus disease 2019 (COVID-19). Clin Infect Dis. 2021;73(11):e4329–35. doi: https://doi.org/10.1093/cid/ciaa1517
9. Szumska E, Czajkowski P, Zablocki M, et al. A Multifaceted Approach to the “Bare below the Elbow” Concept and Hand Hygiene Compliance among Healthcare Professionals—Multicenter Population-Based Study. Int J Environ Res Public Health. 2023;20(5):4435. doi: https://doi.org/10.3390/ijerph20054435
10. COFEN. Brasil responde por 30% das mortes de profissionais de Enfermagem por covid-19. Obs da Enferm. 2023. Avaliable: https://www.cofen.gov.br/brasil-responde-por-30-das-mortes-de-profissionais-de-enfermagem-por-covid-19/
11. Silva VGF, Silva BN, Pinto ÉSG, et al. The nurse’s work in the context of COVID-19 pandemic. Rev Bras Enferm. 2021;74. doi: https://doi.org/10.1590/0034-7167-2020-0594
12. Baretta D, Amrein MA, Bäder C, et al. Promoting Hand Hygiene During the COVID-19 Pandemic: Parallel Randomized Trial for the Optimization of the Soapp App. JMIR mHealth uHealth. 2023;11:e43241. doi: https://doi.org/10.2196/43241
13. WHO. WHO Guidel hand Hyg Heal care First Glob patient Saf Chall clean care is safe care. 2009. Avaliable: https://pubmed.ncbi.nlm.nih.gov/23805438/#:~:text=The%20WHO%20guidelines%20on%20hand%20hygiene%20in%20health,transmission%20of%20pathogenic%20microorganisms%20to%20patients%20and%20HCWs.
14. Kong A, Botero-Suarez CS, Rahamatalli B, et al. Hand Hygiene and Hospital-Acquired Infections during COVID-19 Increased Vigilance: One Hospital’s Experience. HCA Healthc J Med. 2021;2(5):11. doi: https://doi.org/10.36518/2689-0216.1296
15. Centers for Disease Control. (CDC). Guidel Hand Hyg Heal Settings Recomm Healthc Infect Control Pract Advis Comm. 2020. Avaliable: https://www.who.int/publications/i/item/9789241597906
16. WHO. Guidel Core Components Infect Prev Control Program Natl Acute Heal Care Facil Level. 2016. Avaliable: https://www.who.int/teams/integrated-health-services/infection-prevention-control/core-components
17. Bergman L, Falk A, Wolf A, et al. Registered nurses’ experiences of working in the intensive care unit during the COVID‐19 pandemic. Nurs Crit Care. 2021;26(6):467–75. doi: https://doi.org/10.1111/nicc.12649
18. Wang Y, Yang J, Qiao F, et al. Compared hand hygiene compliance among healthcare providers before and after the COVID-19 pandemic: A rapid review and meta-analysis. Am J Infect Control. 2022;50(5):563–71. doi: https://doi.org/10.1016/j.ajic.2021.11.030
19. Lipsitch M, Swerdlow DL, Finelli L. Defining the epidemiology of Covid-19—studies needed. N Engl J Med. 2020;382(13):1194–6. doi: https://doi.org/10.1056/NEJMp2002125
20. Moore LD, Robbins G, Quinn J, et al. The impact of COVID-19 pandemic on hand hygiene performance in hospitals. Am J Infect Control. 2021;49(1):30–3. doi: https://doi.org/10.1016/j.ajic.2020.08.021
21. Johansson MA, Quandelacy TM, Kada S, et al. SARS-CoV-2 transmission from people without COVID-19 symptoms. JAMA Netw open. 2021;4(1):e2035057–e2035057. doi: https://doi.org/10.1001/jamanetworkopen.2020.35057
22. Thomas JR, Martin P, Etnier J, et al. Research methods in physical activity. Human kinetics; 2022. Avaliable: https://books.google.at/books?hl=pt-BR&lr=&id=pJFSEAAAQBAJ&oi=fnd&pg=PR1&dq=Research+methods+in+physical+activity&ots=vTMsPqMp71&sig=MdStsfDyrg6k0Eg0pH1wGCfMPNQ&redir_esc=y#v=onepage&q=Research%20methods%20in%20physical%20activity&f=false
23. Haddad MCL, Évora YDM. Qualidade da assistência de enfermagem: a opinião do paciente internado em hospital universitário público. Ciência, Cuid e Saúde. 2008;7:45–52. Avaliable: https://periodicos.uem.br/ojs/index.php/CiencCuidSaude/article/view/6559/3875
24. Nonino E, Anselmi ML, Dalmas JC. Qualidade do procedimento curativo em pacientes internados em um hospital universitário. Rev Latino-am Enfermagem[Internet]. 2008;16(1). doi: https://doi.org/10.1590/S0104-11692008000100010
25. ANVISA. Manual de Segurança do Paciente: Higienização das mãos. 2010. Avaliable: https://bvsms.saude.gov.br/bvs/publicacoes/seguranca_paciente_servicos_saude_higienizacao_maos.pdf
26. Cordeiro JFC, Menegueti MG, Laus AM, Tipple AFV, Santana RC, Canini SRMS. Higienização das mãos pela equipe de enfermagem na atenção domiciliar: um estudo transversal. Rev da Esc Enferm da USP. 2021;55. doi: https://doi.org/10.1590/1980-220X-REEUSP-2021-0104
27. Korb JP, Jezewski G, Aozane F, et al. Conhecimento sobre higienização das mãos na perspectiva de profissionais de enfermagem em um pronto atendimento. Rev Pesqui Cuid é Fundam. 2019;11(1):517–23. doi: http://dx.doi.org/10.9789/2175-5361
28. Derhun FM, Souza VS, Costa MAR, et al. Conhecimento de profissionais de enfermagem sobre higienização das mãos. Cogitare Enferm. 2016;21(3). Avaliable: https://www.redalyc.org/journal/4836/483653826006/html/v
29. Locks L, Lacerda JT, Gomes E, et al. Qualidade da higienização das mãos de profissionais atuantes em unidades básicas de saúde. Rev Gaúcha Enferm. 2011;32:569–75. doi: https://doi.org/10.1590/S1983-14472011000300019
30. Kısacık ÖG, Ciğerci Y, Güneş Ü. Impact of the fluorescent concretization intervention on effectiveness of hand hygiene in nursing students: A randomized controlled study. Nurse Educ Today. 2021 Feb;97:104719. doi: https://doi.org/10.1016/j.nedt.2020.104719
31. Chun H-K, Kim K-M, Park H-R. Effects of hand hygiene education and individual feedback on hand hygiene behaviour, MRSA acquisition rate and MRSA colonization pressure among intensive care unit nurses. Int J Nurs Pract. 2015 Dec;21(6):709–15. doi: https://doi.org/10.1111/ijn.12288
32. Sharma M, Bachani R. Knowledge, Attitude, Practice, and Perceived Barriers for the Compliance of Standard Precautions among Medical and Nursing Students in Central India. Int J Environ Res Public Health. 2023;20(8):5487. doi: https://doi.org/10.3390/ijerph20085487
33. Noleto RC, Campos CF. Estratégias desenvolvidas pelos enfermeiros para garantir a segurança do paciente na unidade de terapia intensiva neonatal. Facit Bus Technol J. 2020;2(16). Avaliable: http://revistas.faculdadefacit.edu.br/index.php/JNT/article/view/605#:~:text=Discuss%C3%A3o%3A%20Evidenciou-se%20que%20as%20principais%20estrat%C3%A9gias%20desenvolvidas%20foram,de%20erros%20de%20medica%C3%A7%C3%A3o%20e%20cria%C3%A7%C3%A3o%20de%20subcategorias.
34. Silva EL, Crivellaro WH, Martins CC, et al. Adesão à prática de higienização das mãos por profissionais de saúde de um hospital do interior paulista. An Enferm DO UNIFUNEC. 2019;5(5). Avaliable: https://www.redalyc.org/journal/4836/483653650011/html/
35. Montero-Vilchez T, Martinez-Lopez A, Cuenca-Barrales C, et al. Assessment of hand hygiene strategies on skin barrier function during COVID-19 pandemic: A randomized clinical trial. Contact Dermatitis. 2022 Apr;86(4):276–85. doi: https://doi.org/10.1111/cod.14034
36. Bazaid AS, Aldarhami A, Binsaleh NK, et al. Knowledge and practice of personal protective measures during the COVID-19 pandemic: A cross-sectional study in Saudi Arabia. PLoS One. 2020;15(12):e0243695. doi: https://doi.org/10.1371/journal.pone.0243695
37. Wangchuk T, Kinga-Wangdi U, Tshering U, et al. Hand Hygiene, Face Mask Use, and Associated Factors during the COVID-19 Pandemic among the Students of Mongar Higher Secondary School, Bhutan: A Cross-Sectional Study. Int J Environ Res Public Health. 2023;20(2):1058. doi: https://doi.org/10.3390/ijerph20021058
38. Magnago TSBS, Ongaro JD, Greco PBT, et al. Infraestrutura para higienização das mãos em um hospital universitário. Rev Gaúcha Enferm. 2019;40. doi: https://doi.org/10.1590/1983-1447.2019.20180193
39. WHO. Higiene das Mãos na Assistência à Saúde. SALVE VIDAS. Higienize suas Mãos/ Organ Mund da Saúde Hig das Mãos na Assist à Saúde Extra-hospitalar e Domic e nas Instituições Longa Permanência - Um Guia para a Implementação da Estratégia Multimodal da OMS para a Melhor. 2014;73p. Avaliable: https://www.paho.org/pt/campanhas/dia-mundial-higiene-das-maos-2023
40. Almeida MC, Lopes MBL. Atuação do enfermeiro na atenção básica de saúde. Rev saúde dom alberto. 2019;4(1):169–86. Avaliable: https://revista.domalberto.edu.br/revistadesaudedomalberto/article/view/145
41. Tebbeb N, Villemagne F, Prieur T, et al. COVID-19 health crisis workloads and screening for psychological impact in nursing home staff: A qualitative and quantitative survey. Int J Environ Res Public Health. 2022;19(7):4061. doi: https://doi.org/10.3390/ijerph19074061
42. Ashinyo ME, Dubik SD, Duti V, et al. Infection prevention and control compliance among exposed healthcare workers in COVID-19 treatment centers in Ghana: A descriptive cross-sectional study. PLoS One. 2021;16(3):e0248282. doi: https://doi.org/10.1371/journal.pone.0248282
43. McDonald MV, Brickner C, Russell D, et al. Observation of hand hygiene practices in home health care. J Am Med Dir Assoc. 2021;22(5):1029–34. doi: https://doi.org/10.1016/j.jamda.2020.07.031
44. Abbas K, Nawaz SMA, Amin N et al. A web-based health education module and its impact on the preventive practices of health-care workers during the COVID-19 pandemic. Health Educ Res. 2020;35(5):353–61. doi: https://doi.org/10.1093/her/cyaa034
Información adicional
redalyc-journal-id: 5704