Article
Perception and use of herbal medicine in Hermosillo, Sonora (Northwest Mexico)
Percepción y uso de la medicina herbolaria en Hermosillo, Sonora (noroeste de México)
Perception and use of herbal medicine in Hermosillo, Sonora (Northwest Mexico)
Biotecnia, vol. 26, e2284, 2024
Universidad de Sonora, División de Ciencias Biológicas y de la Salud
Received: 07 March 2024
Accepted: 17 May 2024
Published: 01 July 2024
Abstract: Using herbal resources for medicinal purposes has persisted across diverse cultures, harnessing potential bioactivities. Despite the availability of commercial drugs, populations, including those in Mexico, continue to integrate herbal medicine into their healthcare practices. This study on Hermosillo, city in Northwest Mexico, explored the prevalence and patterns of herbal medicine use. A cross-sectional study was conducted from May to September 2023, surveying 441 residents through a structured questionnaire. Demographic characteristics, awareness, and experiences with herbal medicine were assessed. Most participants were female (67.57 %), age 30 years old or younger (67.57 %), and urban residents (90.70 %). The family was the primary source of knowledge for herbal medicine (73.92 %), emphasizing cultural continuity. Most participants (93.65 %) used herbal medicine when regarded as necessary, with 57.59 % reporting partial success. Despite reservations about safety (41.59 %), concurrent use with conventional treatments was common. The study underscores the persistent cultural connection to herbal medicine in families of Hermosillo. Awareness campaigns emphasizing responsible herbal medicine use, especially in vulnerable groups, are crucial. These findings contribute to a broader understanding of herbal medicine trends and practices, emphasizing the importance of local perspectives.
Keywords: Herbal resources, alternative medicine, herbal knowledge.
Resumen: El uso de recursos herbolarios medicinales ha persistido en diversas culturas, aprovechando posibles bioactividades. A pesar de los medicamentos comerciales disponibles, las poblaciones, incluyendo México, siguen usando hierbas en cuidados de salud. Este estudio en Hermosillo, ciudad del noroeste de México, explora la prevalencia y uso de medicina herbolaria. Se realizó un estudio transversal de mayo a septiembre de 2023, encuestando a 441 residentes mediante cuestionarios estructurados. Se evaluaron características demográficas, conocimiento y experiencias con medicina herbolaria. La mayoría de los participantes fueron mujeres (68.56 %), menores de 30 años (67.12 %) y residentes urbanos (90.82 %). La familia fue la principal fuente de conocimientos sobre fitoterapia (73.7 %), destacando la continuidad cultural. El 93 % de los participantes utilizaron hierbas medicinales cuando lo consideraron necesario, y el 56.9 % informó éxito parcial. A pesar de las reservas sobre su seguridad (41.6 %), el uso simultáneo con tratamientos convencionales fue común (48.1 %). El estudio subraya la conexión cultural entre medicina herbolaria y familias mexicanas. Son necesarias campañas de sensibilización fomentando el uso responsable de medicinas herbolarias, especialmente en grupos vulnerables. Los hallazgos comparten una comprensión más amplia de tendencias y prácticas de la medicina herbolaria, enfatizando las perspectivas locales.
Palabras clave: Recursos herbolarios, medicina alternativa, conocimientos herbolarios.
Introduction
Herbal resources have been used by humankind worldwide for years, often in undiscovered forms. Numerous plants contain metabolites with potential biological activities, including hepatoprotective, antitumor, antioxidant, and antimicrobial properties (Veiga et al., 2008). In this regard, plants have traditionally been employed to treat or cure diseases (Armendáriz-Barragán et al., 2016). Despite the availability of a wide array of commercial drugs, some communities continue to incorporate herbal medicine into their daily lives (Al Akeel et al., 2018). It is estimated that the use of herbal medicine has increased over the last decade at specific regions worldwide, potentially influenced by regional cultural factors (Welz et al., 2019).
Based on this, there have been comparisons regarding the use of traditional herbal medicine between different regions, such as China, and North American indigenous communities like the Chumash, which has historically inhabited coastal areas of California (USA). Despite belonging to geographically distinct regions, these communities have similarities in the therapeutic use of plants (Adams et al., 2010).
On the other hand, the use of medicinal plants in Mexico is an integral part of its culture, being the second country with the most registered medicinal plants (Rojas et al., 2022). In Central-Western Mexico, around 59.2 % of the population was estimated to use herbal resources to treat type 2 diabetes mellitus (Rodriguez-Fragoso et al., 2008; Ruiz-Noa et al., 2021). Similarly, an estimated 14.6 % of pregnant women residing in the central region of Mexico used herbal remedies (Alonso-Castro et al., 2018). Nevertheless, variations in practice and knowledge about herbal medicine may be region-dependent (Hopkins, 2011). Aligned with this perspective, in Mexico, some ethnic communities living at different areas and diverse environments, use plants from their surroundings to meet multiple needs, including their health improvement. Some of these practices are inherited generationally, and some persist, while others are forgotten (Cruz-Perez et al., 2021). Despite sharing Mexican traditions, cultural differences, particularly in the Northern part of the country, are due to factors such as its proximity to the United States and environmental conditions. However, the information about the frequency and practice of herbal medicine in each region of the country, specifically in the Northwest, is limited. This study aimed to survey the residents of Hermosillo, Sonora, in Northwest Mexico, to gain information about the use of herbal medicine, and its relationship with the sociodemographic characteristics of the population. Knowledge will be provided about the differences or similarities on the use of herbal medicine, to allow data comparisons among the different regions in the country and worldwide. Additionally, data associated with the practice of herbal medicine may help to elaborate regulations about the distribution and sale of herbal medicine in the country. This information will contribute to our understanding and analysis on the region’s current use trends in herbal medicine, and to keep health professionals informed about this practice in Mexico.
Material and methods
A cross-sectional study was conducted in the city of Hermosillo (29°04′30″N, 110°57′30″O), which has a population of 936,263 inhabitants (Ayuntamiento de Hermosillo, 2022). The study was carried out from May to September 2023. The inclusion criteria were adults of both sexes, aged over 18 years old, and residents of the municipality for at least two years. Furthermore, the Cochran formula was employed to calculate the minimum required sample size.
Where n = minimum sample size required in the study, z = Z score or standard deviations, p = proportion of people using herbal medicine in the study area and d = acceptable error level.
The estimated sample size was 384 subjects, calculated based on acceptable parameters with similar studies. These parameters include an acceptable error level of 3 % (0.03) and a 95 % confidence interval, corresponding to a Z score 1.96 (Aina et al., 2020). Subsequently, a structured and validated questionnaire with multiple-choice answers was applied to the participants based on Al Akeel et al. (2018) and culturally adapted (Al Akeel et al., 2018). Five questions for sociocultural data constituted the questionnaire, eight for socioeconomic information, and 11 for use and knowledge of herbal medicine. The responses were kept simple, objective, and concise to ensure optimal understanding by the participants.
Moreover, the socioeconomic level was determined using the AMAI rule 8 X 7, 2020, which has a scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). This classification was processed considering various factors, such as educational levels, occupation, possession of assets, and home dimensions. The distribution of questionnaires was conducted electronically through popular social media platforms such as X® (previously known as Twitter), Facebook®, and WhatsApp®. Google Forms® was employed for data collection, ensuring the participants’ anonymity during the information-sharing process.
Descriptive statistics were used to interpret the data, and a chi-square test was carried out on the questions that did not allow more than one answer at a time, to find associations between the sociodemographic characteristics of the participants and their answers. All the statistical analyses were performed with the NCSS 2021 statistical package.
Results and discussion
Sociodemographic characteristics of the participants
The survey was conducted between July and September 2023, encompassing public spaces and academic institutions. A total of 441 individual agreed to participate. Regarding the demographic characteristics of the participants (Table 1), the majority were female (67.57 %), most participants were 30 years old or younger (67.57 %) and resided at urban areas (90.70 %). Regarding education, 51.94 % had completed university studies or attained a higher level of education, while the remainder had educational levels below this threshold. Additionally, the majority were employees (40.81 %) or students (34.92 %); therefore, they had a socioeconomic level of C.
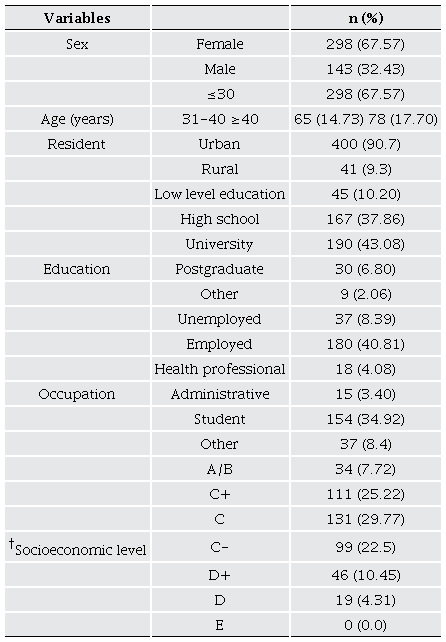
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E).
Use and knowledge of herbal medicine
Regarding the responses provided by the survey participants (Table 2), 84.12 % affirm their awareness of, and experience with, herbal medicine. Notably, the primary source of knowledge about these alternatives is family, as 73.92 % of the participants reported. This is in agreement with previous findings indicating that even Mexican American residents continue to rely on traditional medicine within their family networks (Lopez, 2005). Similarly, González-Stuart (2010) reported that from interviews with herbal medicine vendors in Monterrey, 42 % indicated that their understanding of this alternative medicine stemmed from family traditions or personal experiences. This suggested a persistent cultural connection to herbal medicine within Mexican families, displaying limited variation in the Northern region.
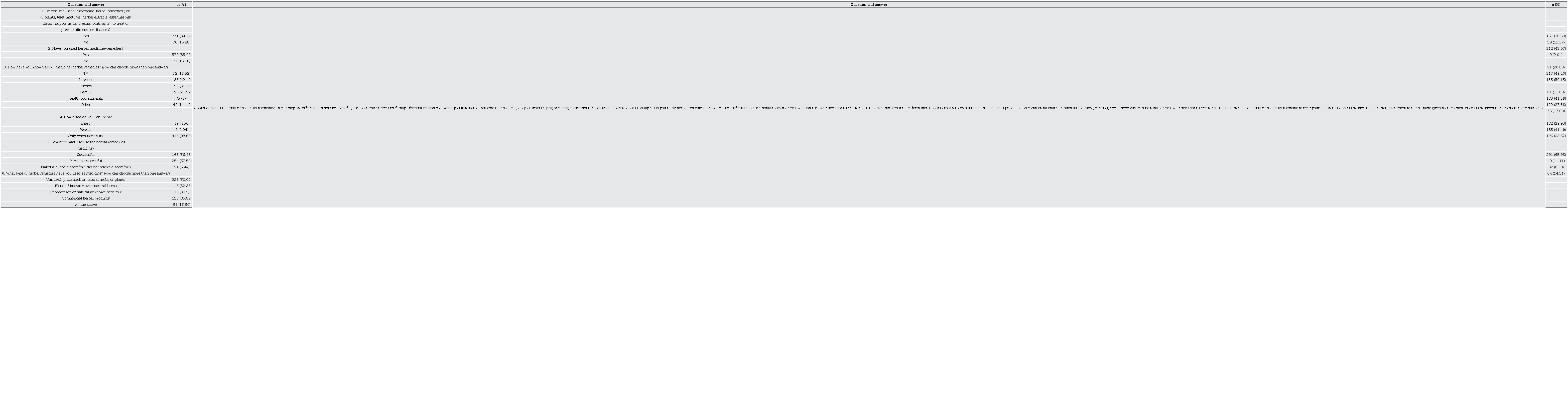
On the other hand, the country’s southern region has also highlighted the family’s significant influence on adopting these medicinal alternatives, mainly attributed to mothers (Cabada-Aguirre et al., 2023). This underscores the notion that Mexican communities predominantly preserve this cultural practice. Furthermore, reports from the La Rosita community at Puerto Colombia reveal that like Mexico, mothers take a lead role in traditional medicine usage, followed by grandmothers (Duque et al., 2018). However, this pattern may differ from experiences in other countries worldwide. For instance, a study conducted in Saudi Arabia indicated that most participants who used herbal remedies, did so based on recommendations from friends and neighbors (Al Akeel et al., 2018), highlighting behaviors that may not necessarily be replicated in other regions.
Furthermore, 93.65 % of the participants indicated they exclusively resort to this medicine when necessary. Of these, 57.59 % reported partial success with the treatment, while 36.96 % deemed it entirely successful. Only 5.44 % reported undesirable effects or inadequate relief from discomfort. Herbal medicine has demonstrated historical efficacy in treating and alleviating conditions such as allergies, arthritis, migraines, burns, and gastrointestinal discomfort. However, the effectiveness of herbal medicine can be influenced by the product’s origin, and although currently national institutions such as CANIFARMA, COFEPRIS, Farmacopea de los Estados Unidos Mexicanos A.C., and the Federacion Nacional de la Industria Herbolaria, Medicina Alternativa, Tradicional y Naturista A.C., rules the herbal medicine, additional work is required to ensure the optimal distribution conditions and, to optimize their potential benefits (Guerrero-Encinas et al., 2023; Sam, 2019).
In addition, most respondents stated that they consumed unmixed, processed, or natural herbs or plants (50.02 %) and natural herbs or plants, while 35.82 % opted for commercial herbal products.
Additionally, a significant portion of participants (48.07 %) attributed their consumption of herbal remedies to family-inherited beliefs, and 36.50 % expressed a belief in the efficacy of these remedies. Presently, one of the primary motivations for using herbs in treating ailments is their natural origin and longstanding historical use by our ancestors. This inclination is reinforced by the perception that conventional medicine can occasionally lead to adverse effects on health (Elechi-Amadi et al., 2021). The industry has capitalized on this preference by investing in developing herbal medicine for commercial purposes. Reports indicate a substantial rise in the commercialization of herbal products for medicinal use, growing at a rate of 15 % annually, as per information from the World Bank (Gunjan et al., 2015). This information suggests that the commercialization of these products is emerging as a focal point for private initiatives fueled by a rising demand among the population.
On the other hand, 20.63 % of participants stated that they continue the use of herbal remedies even while undergoing conventional medical treatments, and 30.15 % suspend them occasionally. Furthermore, 41.59 % expressed a lack of belief in the safety of herbal medicine. In comparison, 27.66 % claimed uncertainty about its safety. Interestingly, despite the majority having reservations about the safety of herbal treatments, they tend to consume them concurrently with traditional medications. It is crucial to acknowledge that the combined effects of herbal medicine and allopathic medications may lead to antagonistic or, in some cases, synergistic effects that may not always be favorable. This concern is underscored by a study conducted on diabetic patients at the Jazan region of Saudi Arabia, where 33.7 % of participants reported the use of complementary and alternative medicine alongside modern medicine. Alarmingly, 67.4 % did not discuss their use of traditional remedies with their doctors, raising the possibility of either diminishing the intended effect, leading to hyperglycemia, or intensifying the effect, resulting in hypoglycemia (Meraya et al., 2022).
Furthermore, it has been evident that in Africa, a significant proportion of individuals, ranging from 12.4 to 77.1 %, concurrently consume both traditional and conventional medicine. Sometimes, healthcare providers may need to be aware of this dual consumption (Ekpor et al., 2023). Despite the benefits of phytotherapy, it is crucial to raise awareness among the population to encourage responsible use of these resources and prevent potential adverse effects, resulting from the current lack of comprehensive information about these treatments.
On the other hand, 41.49 % of respondents believe that the media’s promotion of herbal medicine is unreliable, while 29.93 % express trust in it, and 28.57 % remain indifferent. Presently, there is a shift in public preferences, with doubts arising about the safety of conventional medicine. Consequently, individuals opt for herbal medicine due to its natural composition without synthetic chemical compounds. Exploiting these emerging opportunities, the industry markets products centered around plant extracts (Khayru and Issalillah, 2021). Nevertheless, regulations are imperative in overseeing the claims made by companies regarding these products. Many companies promise to alleviate a myriad of discomforts without substantial evidence, and these products often lack evaluations to substantiate the safety of their consumption (Ismail et al., 2018).
Finally, 65.98 % of the participants did not have children, but 22.90 % said they had given herbal treatment to their children once or more. A review carried out in the Latino population (from 1994 to 2013) indicated that most mothers perceive herbs as safe because they are natural, reporting their use to treat stomach pains, skin abrasions and dermatitis, constipation, and colic (Acorda et al., 2020). Additionally, a systematic review carried out in 2017, reported that over 66 % of children and adolescents who went to the doctor for gastrointestinal discomfort used complementary medicine, which included herbal medicine, and the parents surveyed thought that complementary medicine should also be considered by health professionals (Anheyer et al., 2017). The survey outcomes reveal a notable awareness and application of herbal medicine among participants, predominantly influenced by familial knowledge. This cultural connection to herbal remedies is consistent across diverse Mexican regions, highlighting the enduring impact of family traditions on healthcare decisions. Participants generally turn to herbal medicine when they perceive a need, reporting varying degrees of treatment success, with a small percentage noting undesirable effects. The choice among natural, processed, or commercial herbal products varies, reflecting a combination of family-inherited beliefs and general trust in the efficacy of these remedies. Concerns about the safety of herbal medicine, mainly when used alongside conventional treatments, emphasize the importance of heightened awareness and responsible use.
Relationship between sociodemographic characteristics and use and knowledge of herbal medicine
Regarding the data collected, an association was observed between knowing herbal medicine and being a woman (Table 3). The connection between women and their knowledge of herbal medicine (p = 0.0096) does not originate exclusively in a specific cultural context; somewhat, it is shaped by several factors that exhibit variations depending on the region and community under consideration. In specific cultural contexts, women have historically been assigned traditional roles focused on health care and household management. Within this framework, these women possess deep-rooted knowledge and practice using herbal remedies as an essential part of healthcare within the domestic setting (Boerma, 1995). On the other hand, some women may turn to herbal medicine to address specific health concerns, such as menstrual disorders and menopause, or even as a complement to prenatal and postnatal care (Magtalas et al., 2023).
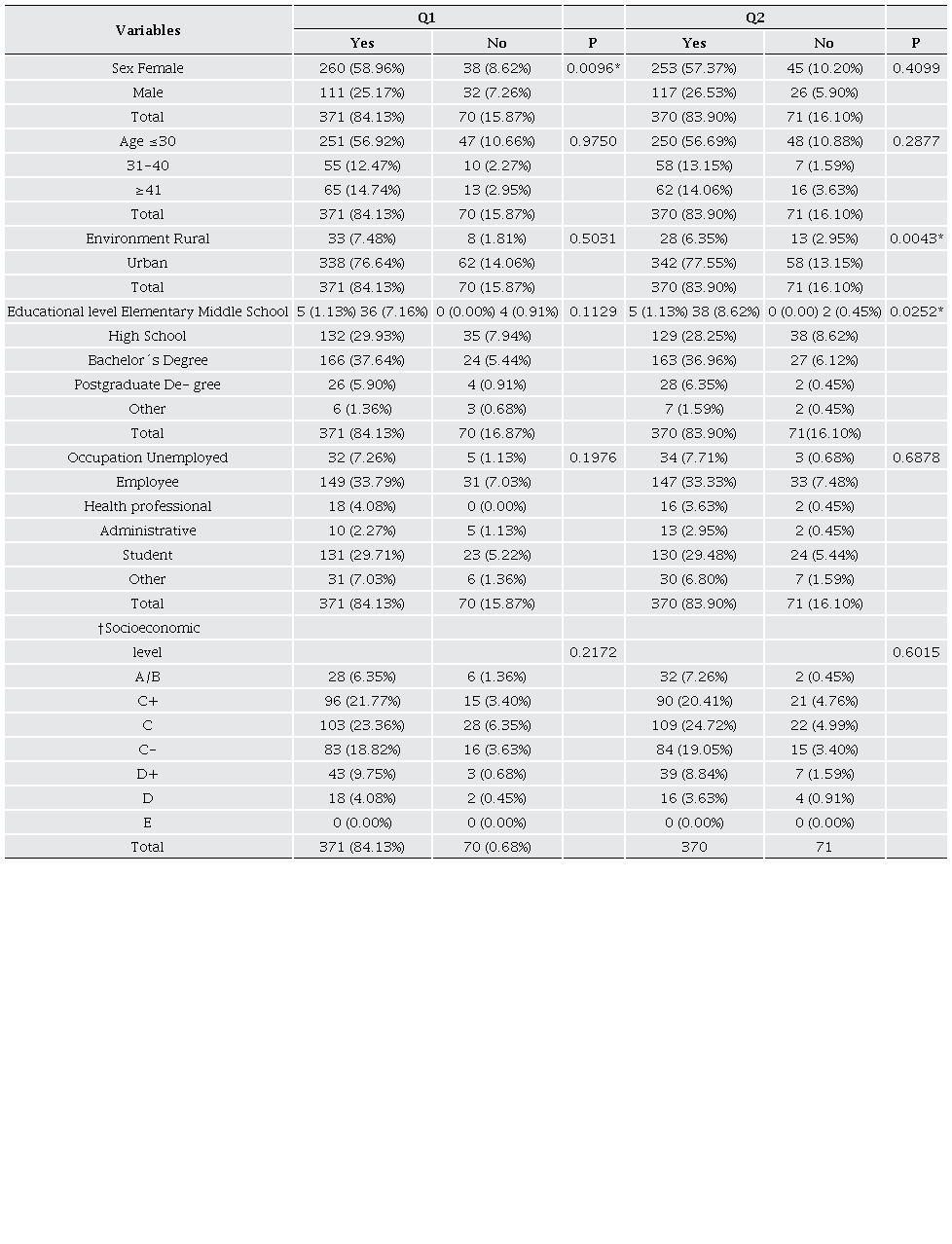
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). Q1; question 1, Q2; question 2. 2-sided Chi-square test, *Significant (p < 0.05).
On the other hand, an association was also found between being an urban resident and having used herbal medicine (p = 0.0043). In this context, this data is contradictory since rural communities, characterized by their close interaction with natural environments, frequently have direct access to various medicinal plants. This proximity to nature eases the acquisition of knowledge and the collection of herbs for medicinal purposes (Cordero et al., 2020). Likewise, herbal medicine has been transmitted from generation to generation in many rural communities as part of their cultural tradition. People learn about the use of medicinal plants through observation and oral teaching contributing to the continuity of these practices (Ouma, 2022). Nevertheless, increasing knowledge about the relevance of natural health has resulted in increased integration of herbal medicine into urban settings. Furthermore, the marketing of natural products and herbalists by urban commercial establishments is increasing, and this may explain this association. In addition, inadvertently herbal resources can be consumed, since are widely employed across some domains, including food, agriculture, and chemistry. These natural raw materials are used to create healthy food products, enhance soil quality in organic farming, and develop chemical compounds for various industrial and pharmaceutical applications (Bolouri et al., 2022).
In addition, there is an association among using herbal medicine occasionally and being an urban resident (p = 0.0415) with a university level of education (p = 0.0001), and affirms that the results of this use were partially successful (Table 4). The association among the occasional use of herbal medicine, urban residence, and college education raises interesting considerations. The evaluation of the partial success of these treatments highlights the complexity of measuring health outcomes and the need for additional research to understand the determinants of this relationship.
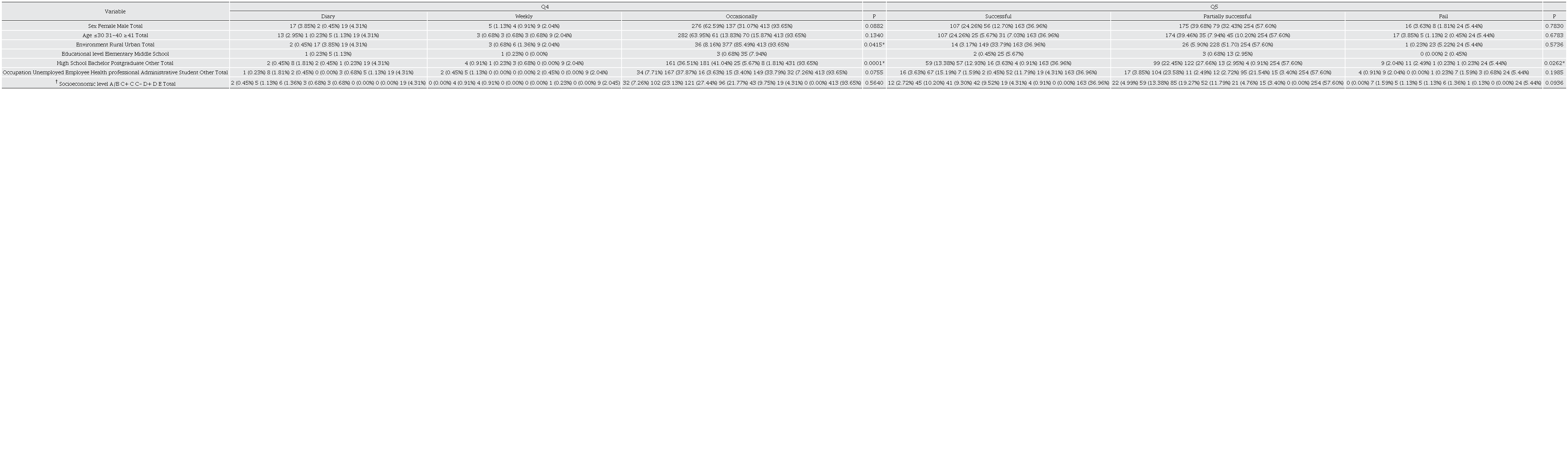
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). Q4; question 4, Q5; question 5. 2-sided Chi-square test, *Significant (p < 0.05).
Likewise, an association was found between using herbal medicine occasionally, being an urban resident, and a university level of education, and the affirmation that the results of its use were partially successful (p = 0.0262) (Table 4). The association between the occasional use of herbal medicine, urban residence, and college education raises exciting considerations. The evaluation of the partial success of these treatments highlights the complexity of measuring health outcomes and the need for additional research to understand the determinants of this relationship.
Another interesting fact was observing an association between having a university education level and using herbal medicine based on “beliefs” (p = 0.0011) (Table 5). Although a college education can offer access to scientific and technological information, cultural and family connections often still play a significant role in health choices. The intergenerational transmission of knowledge about herbal remedies can influence the health practices of people with university training, showing the persistence of family traditions in medicine (Nworu et al., 2015).
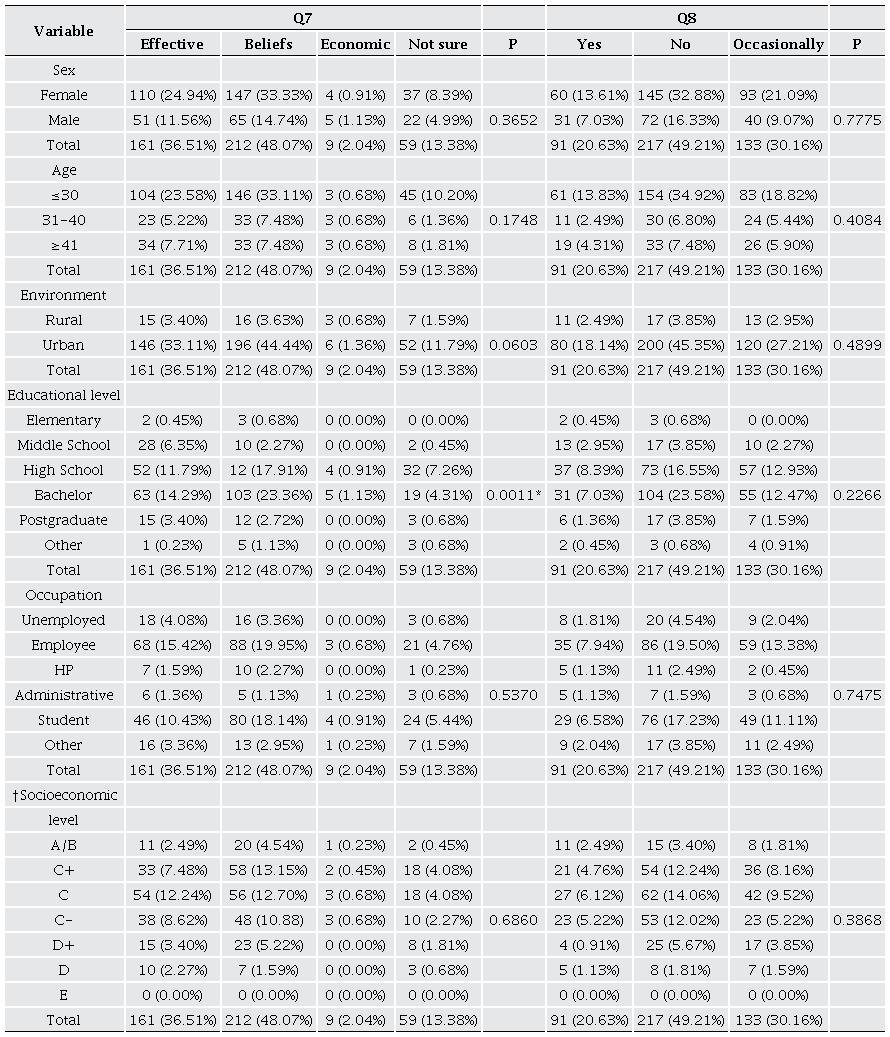
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). Q7; question 7, Q8; question 8. 2-sided Chi-square test, *Significant (p < 0.05).
Besides, an association was found between respondents who did not believe in media propaganda regarding herbal medicine and respondents under 30 years of age (p = 0.0256), who had university studies (p = 0.0008), and were still students (p = 0.0016) (Table 6). Younger, more educated individuals are often more critical and exposed to various information sources. University training can foster essential evaluation skills, leading to greater distrust in advertising messages. Additionally, the preference for more natural approaches in healthcare may influence the perception of herbal medicine, especially among those still immersed in academic settings. Even so, the influence of mass media on the use of herbal medicine is undeniable. Through various platforms such as television, internet, and social media, information is spread widely, shaping public perceptions and behaviors (Ng et al., 2023). Media coverage often highlights the perceived benefits of herbal medicine, leading to increased interest and adoption among consumers seeking alternative or complementary healthcare options.
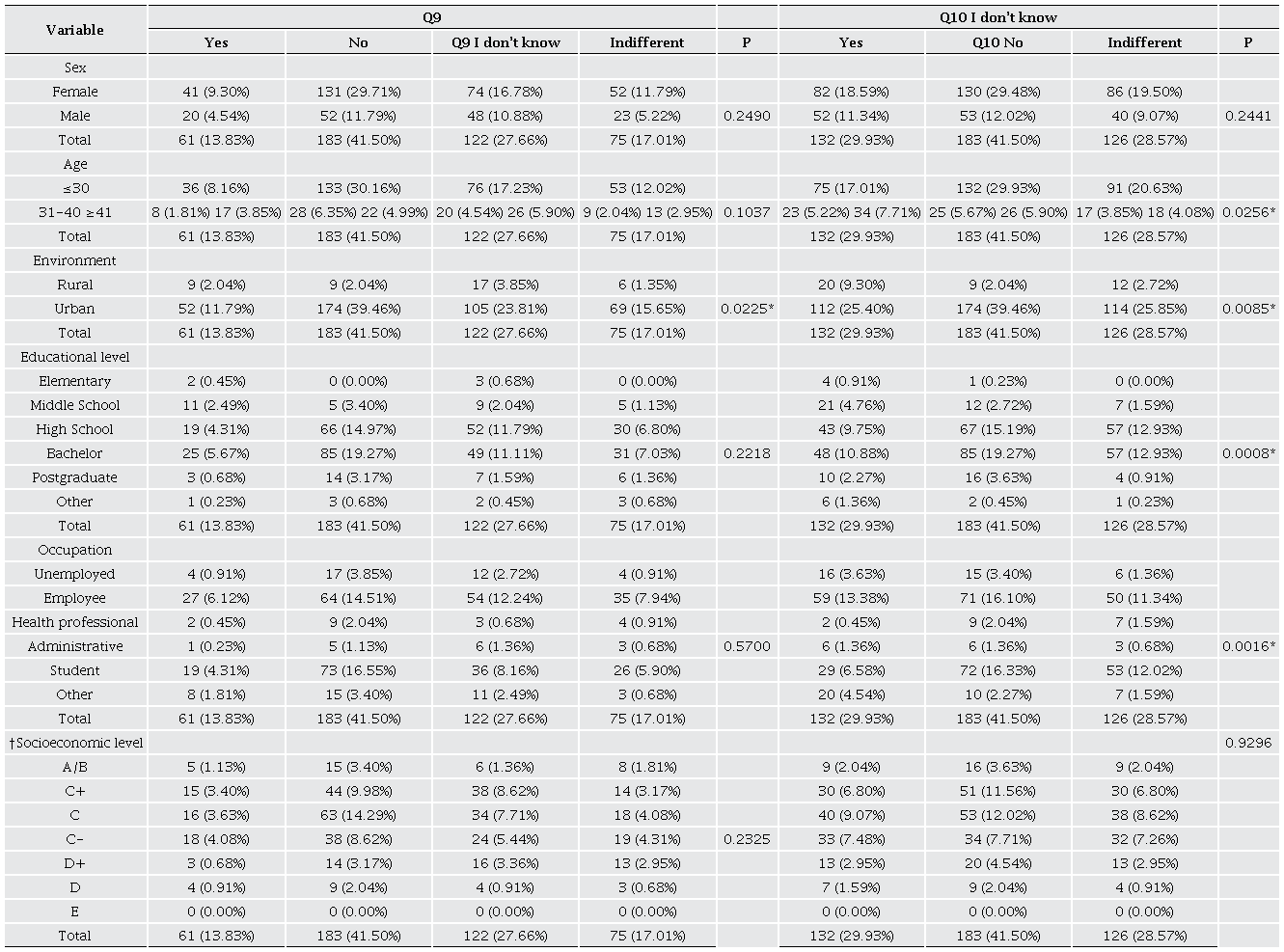
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). Q9; question 9, Q10; question 10. 2-sided Chi-square test, *Significant (p < 0.05).
Finally, it is worth to note the no association between the socioeconomic level and herbal medicine use and knowledge. Currently, herbal medicine is not conditioned by socioeconomic strata, evidencing a trend toward democratizing this practice in various communities. Unlike in the past, where specific natural health approaches might have been tied to certain economic levels, today, a broader and more diverse acceptance of herbal medicine is seen across all sectors of society (Kemppainen et al., 2018). On the another hand, although wealthy people have access to high-priced products that promise to be more effective, current government institutions have not been able to fully regulate the process of these products, increasing the risk of accessing to unexpected less effective items (Balekundri and Mannur, 2020). People from different socioeconomic backgrounds are turning to herbal medicine to address various health needs, reflecting a shift toward a more accessible appreciation of natural care methods. This phenomenon suggests that herbal medicine has surpassed economic barriers and has become a treatment option appreciated for its accessibility and comprehensive approach to well-being. On another hand, most of participants reported that they did not have children, observing an association between this and being a student, and/or having high school as level of education (Table 7). For this reason, no association was found between sociodemographic characteristics and administering herbal medicine to their children.
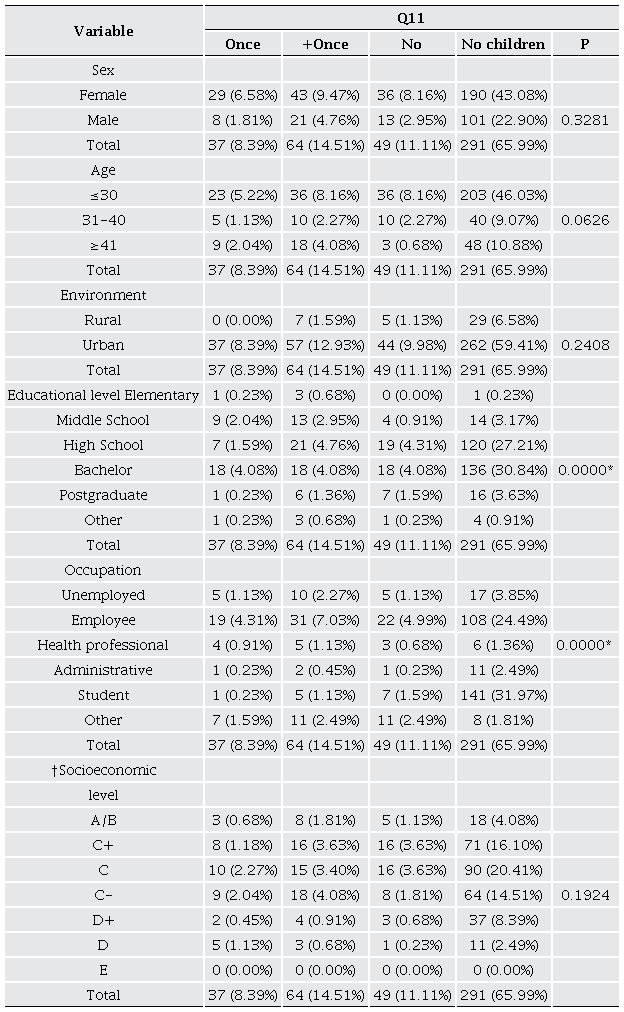
† Scale that categorizes Mexican households into different socioeconomic segments, ranging from level A/B, which indicates the highest socioeconomic stratum, to level E, which reflects the lowest socioeconomic stratum (A/B, C+, C, C-, D+, D, and E). Q11; question 11. 2-sided Chi-square test, *Significant (p < 0.05).
In herbal medicine, it is strongly recommended to consult a healthcare professional before starting its administration. Thorough research on herbs, their proper dosage, and possible interactions, are essential for safe application. Informing health professionals about herbal medicine usage, purchasing quality products, and being aware of potential adverse reactions are crucial practices. Furthermore, it is emphasized that herbal medicine should not replace conventional medical treatments, and that variety in the diet, including herbs and medicinal foods, can be a balanced way to take advantage of its benefits. These recommendations are significant for vulnerable groups such as pregnant women, older people, and those with preexisting medical conditions.
Conclusions
Our findings reveal the persistence of intergenerational solid and cultural ties that significantly influence adopting herbal practice despite the educational level achieved. The widespread awareness and positive perception of herbal medicine underline its roots in the daily lives of Mexican families. Sociodemographic characteristics such as gender, urban residence, and education level, among others described above, are associated with the knowledge and usage of herbal medicine, highlighting the complex interplay among cultural, social, and educational factors in shaping health practices. This may reflect similarities between the Northwest region, specifically the city of Hermosillo, and what is reported in other areas. However, measures are still necessary to promote the safe use of these treatments. The need for clear and compelling regulations in this area is highlighted. Furthermore, the relevance of addressing these issues stands out from a local perspective, the culture and social particularities that shape the relationship between the population and herbal medicine.
Acknowledgments
Thanks to the people who participated in the survey, to CONAHCyT for doctoral scholarships awarded to Ildefonso Guerrero Encinas and Javier N. González González.
References
Adams, J.D., Garcia, C., and Lien, E.J. 2010. A comparison of Chinese and American Indian (Chumash) medicine. Evidence-Based Complementary and Alternative Medicine 7, 219-225. https://doi.org/10.1093/ecam/nem188
Aina, O., Gautam, L., Simkhada, P., and Hall, S. 2020. Prevalence, determinants and knowledge about herbal medicine and non-hospital utilisation in southwest Nigeria: a cross-sectional study. BMJ Open 10, e040769. https://doi.org/10.1136/bmjopen-2020-040769
Al Akeel, M., Al Ghamdi, W., Al Habib, S., Koshm, M., and Al Otaibi, F. 2018. Herbal medicines: Saudi population knowledge, attitude, and practice at a glance. Journal of Family Medicine and Primary Care 7, 865-875. https://doi.org/10.4103/jfmpc.jfmpc_315_17
Alonso-Castro, A.J., Ruiz-Padilla, A.J., Ruiz-Noa, Y., AlbaBetancourt, C., Domínguez, F., Ibarra-Reynoso, L.D.R., Maldonado-Miranda, J.J., Carranza-Álvarez, C., BlancoSandate, C., Ramírez-Morales, M.A., Zapata-Morales, J.R., Deveze-Álvarez, M.A., Mendoza-Macías, C.L., SolorioAlvarado, C.R., and Rangel-Velázquez, J.E. 2018. Selfmedication practice in pregnant women from central Mexico. Saudi Pharmaceutical Journal 26, 886-890. https://doi.org/10.1016/j.jsps.2018.03.008
Anheyer, D., Frawley, J., Koch, A.K., Lauche, R., Langhorst, J., Dobos, G., and Cramer, H. 2017. Herbal medicines for gastrointestinal disorders in children and adolescents: a systematic review. Pediatrics 139, e20170062. https://doi.org/10.1542/peds.2017-0062
Armendáriz-Barragán, B., Zafar, N., Badri, W., Galindo-Rodríguez, S.A., Kabbaj, D., Fessi, H., and Elaissari, A. 2016. Plant extracts: from encapsulation to application. Expert Opinion on Drug Delivery 13, 1165-1175. https://doi.org/10.1080/17425247.2016.1182487
Balekundri, A., Mannur, V. 2020. Quality control of the traditional herbs and herbal products: a review. Future Journal of Pharmaceutical Sciences 6, 67. https://doi.org/10.1186/s43094-020-00091-5
Boerma, T. 1995. The epidemiological transition: policy and planning implications for developing countries. [Workshop Proceedings]. Population Studies 49, 178-180. https://doi.org/10.1080/0032472031000148376
Bolouri, P., Salami, R., Kouhi, S., Kordi, M., Asgari Lajayer, B., Hadian, J., and Astatkie, T. 2022. Applications of essential oils and plant extracts in different industries. Molecules 27, 8999. https://doi.org/10.3390/molecules27248999
Cabada-Aguirre, P., López López, A.M., Mendoza, K.C.O., Garay Buenrostro, K.D., Luna-Vital, D.A., and Mahady, G.B. 2023. Mexican traditional medicines for women’s reproductive health. Scientific Reports 13, 2807-2820. https://doi.org/10.1038/s41598-023-29921-1
Cordero, S., Gálvez, F., Arenas, J., and Rodríguez Valenzuela, E. 2020. Does access to natural environments explain differences in the use of wild plants between rural and urban populations? Botanical Sciences 99, 104-123. https://doi.org/10.17129/botsci.2622
Duque, M., Gómez, C.M., Cabrera, J.A., and Guzmán, J.D. 2018. Important medicinal plants from traditional ecological knowledge: the case La Rosita community of Puerto Colombia (Atlántico, Colombia). Boletín Latinoamericano y del Caribe de Plantas Medicinales y Aromáticas 17, 324-341.
Ekpor, E., Osei, E., and Akyirem, S. 2023. Prevalence and predictors of traditional medicine use among persons with diabetes in Africa: a systematic review. International Health ihad080. https://doi.org/10.1093/inthealth/ihad080
Elechi-Amadi, K.N., Briggs, O.N., Konne, F.E., Giami, L.K.C. and Ajufo, B. 2021. Perception and acceptance of herbal medicines among residents of Port Harcourt, Nigeria. Journal of Complementary and Alternative Medical Research 12, 2434. https://doi.org/10.9734/jocamr/2020/v12i330209
González-Stuart, A.E. 2010. Use of medicinal plants in Monterrey, Mexico. Notulae Scientia Biologicae 2, 07-11. https://doi.org/10.15835/nsb245399
Guerrero-Encinas, I., González-González, J.N., Ayala-Zavala, J.F., González-Aguilar, G.A., Ledesma-Osuna, A.I., LópezMata, M.A., Morales-Figueroa, G.G., and Quihui-Cota, L. 2023. Reviewing the potential of natural antimicrobials for Salmonella spp. gastrointestinal infections: in vitro and in vivo evaluations. Revista Brasileira de Farmacognosia. https://doi.org/10.1007/s43450-023-00481-9
Gunjan, M., Naing, T.W., Saini, R.S., Naidu, D.J.R., and Kumar, I. 2015. Marketing trends & future prospects of herbal medicine in the treatment of various disease. World Journal of Pharmaceutical Research 4, 132-155.
Hopkins, A., 2011. Use of network centrality measures to explain individual levels of herbal remedy cultural competence among the Yucatec Maya in Tabi, Mexico. Field Methods 23, 307-328. https://doi.org/10.1177/1525822X11399400
Ismail, S.F., Daud, M., Jalil, J.Abd., Azmi, I.M.A.G., and Safuan, S. 2018. Protecting consumers from misleading online advertisement for herbal and traditional medicines in Malaysia: are the laws sufficient? 6th International Conference on Cyber and IT Service Management 1-6. https://doi.org/10.1109/CITSM.2018.8674372
Kemppainen, L.M., Kemppainen, T.T., Reippainen, J.A., Salmenniemi, S.T., and Vuolanto, P.H. 2018. Use of complementary and alternative medicine in Europe: health-related and sociodemographic determinants. Scandinavian Journal of Public Health 46, 448-455. https:// doi.org/10.1177/1403494817733869
Khayru, R.K., and Issalillah, F. 2021. Study on consumer behavior and purchase of herbal medicine based on the marketing mix. Journal of Marketing and Business Research 1. 1-14.
Lopez, R.A. 2005. Use of alternative folk medicine by Mexican American women. Journal of Immigrant Health 7, 23-31. https://doi.org/10.1007/s10903-005-1387-8
Lucía, C.-P.A., Jacqueline, B.-R., Alberto, B.-R.L., David, B.-A., and Beatriz, R.-A. 2021. Actualized inventory of medicinal plants used in traditional medicine in Oaxaca, Mexico. Journal of Ethnobiology and Ethnomedicine 17, 7. https://doi.org/10.1186/s13002-020-00431-y
Magtalas, M.C., Balbin, P.T., Cruz, E.C., Adizas, A.V., Gerardo, J.P.Z., Sausa, R.B., Lee, K.Y., and Tantengco, O.A.G. 2023. A systematic review of medicinal plants used in the treatment of gynecologic diseases in the Philippines. Phytomedicine Plus 3, 100462. https://doi.org/10.1016/j.phyplu.2023.100462
Meraya, A.M., Ahsan, W., Albratty, M., Alhazmi, H.A., and Najmi, A. 2022. Perception of individuals with diabetes about efficacy and safety of complementary and alternative medicines (CAM) in the Jazan Region, Saudi Arabia. Evidence-Based Complementary and Alternative Medicine 2022, 1-8. https://doi.org/10.1155/2022/2104056
Ng, J.Y., Verhoeff, N., and Steen, J. 2023. What are the ways in which social media is used in the context of complementary and alternative medicine in the health and medical scholarly literature? a scoping review. BMC Complement Med Ther 23, 32. https://doi.org/10.1186/s12906-023-03856-6
Nworu, C.S., Udeogaranya, P.O., Okafor, C.K., Adikwu, A.O., and Akah, P.A. 2015. Perception, usage and knowledge of herbal medicines by students and academic staff of University of Nigeria: A survey. European Journal of Integrative Medicine 7, 218-227. https://doi.org/10.1016/j.eujim.2015.01.005
Ouma, A. 2022. Intergenerational learning processes of traditional medicinal knowledge and socio-spatial transformation dynamics. Frontiers in Sociology 7, 661992. https://doi.org/10.3389/fsoc.2022.661992
Rodriguez-Fragoso, L., Reyes-Esparza, J., Burchiel, S.W., HerreraRuiz, D., and Torres, E. 2008. Risks and benefits of commonly used herbal medicines in Mexico. Toxicology and Applied Pharmacology 227, 125-135. https://doi.org/10.1016/j.taap.2007.10.005
Rojas, P., Jung-Cook, H., Ruiz-Sánchez, E., Rojas-Tomé, I.S., Rojas, C., López-Ramírez, A.M., and Reséndiz-Albor, A.A. 2022. Historical aspects of herbal use and comparison of current regulations of herbal products between Mexico, Canada and the United States of America. International Journal of Environmental Research and Public Health 19, 15690. https://doi.org/10.3390/ijerph192315690
Ruiz-Noa, Y., Ibarra-Reynoso, L.D.R., Ruiz-Padilla, A.J., AlonsoCastro, A.J., Ramírez-Morales, M.A., Zapata-Morales, J.R., Orozco-Castellanos, L.M., Solorio-Alvardo, C.R., and LaraMorales, A. 2021. Use of herbal medicine for diabetes mellitus in adults from the central-western region of Mexico. Primary Care Diabetes 15, 1095-1099. https://doi.org/10.1016/j.pcd.2021.08.010
Sam, D.S. 2019. Importance and effectiveness of herbal medicines. Journal of Pharmacognosy and Phytochemistry 8, 354-357.
Veiga, M., Costa, E.M., Silva, S., and Pintado, M. 2018. Impact of plant extracts upon human health: a review. Critical Reviews in Food Science and Nutrition 60, 873-886 https://doi.org/10.1080/10408398.2018.1540969
Welz, A.N., Emberger-Klein, A., and Menrad, K. 2019. The importance of herbal medicine use in the German healthcare system: prevalence, usage pattern, and influencing factors. BMC Health Serv Res 19, 952. https://doi.org/10.1186/s12913-019-4739-0
Author notes
*Author for correspondence: Luis Quihui Cota. e-mail: lquihui@ciad.mx
Conflict of interest declaration
The authors declare no conflict of interest.
