STUDY PROTOCOLS
The effect of dyskinesia on postural control, balance, gait, and fall risk in people with Parkinson’s disease: a systematic review protocol
The effect of dyskinesia on postural control, balance, gait, and fall risk in people with Parkinson’s disease: a systematic review protocol
Geriatrics, Gerontology and Aging, vol. 18, e0000084, 2024
Sociedade Brasileira de Geriatria e Gerontologia, SBGG
Received: 10 October 2023
Revised document received: 07 February 2024
Accepted: 25 February 2024
Funding
Funding source: FAPESP
Contract number: 2022/14200-0
Abstract: Dyskinesia affects the limbs, trunk, and head and is more prevalent in people with Parkinson’s disease (PD) and a history of falls. More evidence about the effects of dyskinesia on postural control, balance, gait, and fall risk could help improve the quality of life of individuals with PD. This review aims to examine associations between dyskinesia and postural control, balance, gait, and fall risk in individuals with PD. Such information could lead to new approaches to quality of life improvement among individuals with PD. PubMed, CINAHL, PsycInfo, Scopus, and SciELO will be searched for longitudinal, cohort, and case-control studies published in English or Portuguese in any year that investigated the association between dyskinesia and postural control, balance, gait, and fall risk in individuals with PD. Two reviewers will independently evaluate the titles, abstracts, and full texts according to PRISMA guidelines to select eligible studies for the review. Data on participants, dyskinesia, postural control, balance, gait, and fall risk will be extracted and summarized in tables. Two reviewers will independently assess the methodological quality of each study using the Newcastle Ottawa quality assessment scale. Meta-analysis will not be performed. The results of this systematic review will offer insight into the effects of dyskinesia on postural control, balance, gait, and fall risk. Such information could significantly contribute to informed decisions about early motor intervention in individuals with PD.
Keywords: Parkinson’s disease, dyskinesia, risk factors, accidental falls, postural balance, gait.
INTRODUCTION
Individuals with Parkinson’s disease (PD) have a high incidence of falls.1,2,3,4,5,6 Recurrent falls in PD can lead to injuries,3,4,7 reduced participation in social and physical activities,8 fear of falling,8 and lower quality of life.9 The cause of falls in individuals with PD is multifactorial,10 with motor and non-motor symptoms contributing to increased fall risk. Postural instability, freezing of gait,11 motor fluctuation, executive dysfunction and dementia, and high levodopa levels5,12,13,14 are some of the main factors that contribute to falls in people with PD. Dyskinesia, a motor complication of PD, has also been associated with falls.12,14,15,16,17
Dyskinesia, involuntary movement that may occur in individuals with PD on chronic levodopa therapy, can include chorea, stereotypies, and dystonia,18 which can occur in several body parts, especially the limbs, trunk, and head.19 It is associated with long-term and high-dose levodopa use for motor symptoms, although its mechanisms are still unclear.19 Dyskinesia is purportedly caused by a combination of chronic pulsatile dopaminergic receptor stimulation and nigral denervation, which lead to inappropriate input between the striatum and motor cortex.20 The development of dyskinesia is associated with the duration and dose of levodopa therapy,21 as well as age at onset and disease severity.21,22 Van Gerpen et al. observed that in 5 years, approximately 30% of individuals with PD manifested dyskinesia; these values almost doubled in 10 years (i.e., 59%).23 Furthermore, 5-year incidence of dyskinesia in individuals with early-onset PD (i.e., aged 40–59 years), which is nearly 50%, is higher than that of people diagnosed after 70 years of age.22
Dyskinesia is more common in people with PD who have fallen than in those who have not.17 Based on this observation, Rascol et al. suggested that involuntary movements due to dyskinesia can affect balance and increase fall risk in individuals with PD.17 A 1-year prospective study found that 3.6% of falls in individuals with PD were due to dyskinesia.6 A more extensive prospective study of 205 individuals with PD found that freezing of gait and dyskinesia were highly related to falls.14 In addition, dyskinesia has been considered a significant predictor of future falls.17,18,22,24 This was supported by a more recent study, which found that dyskinesia was associated with recurrent falls over 6 months in individuals with PD.16
Given the association between the incidence of falls and dyskinesia, we can hypothesize that dyskinesia negatively affects the balance, postural control, and gait of individuals with PD, increasing fall risk. A previous study identified factors associated with recurrent falls in PD.1 However, no previous studies have determined whether dyskinesia affects postural control, balance, and gait, in addition to increasing fall risk in individuals with PD. Therefore, this systematic review will examine the evidence of associations between dyskinesia and postural control, balance, gait, and fall risk in individuals with PD. Specifically, we will answer 2 research questions: (I) Can dyskinesia affect the postural control, balance, and gait of individuals with PD?; (II) Based on the inconsistent relationship between dyskinesia and falls, can dyskinesia be a risk factor for increased falls in individuals with PD?
METHODS
For this systematic review, observational, cohort (retrospective and prospective), and case-control studies will be selected to investigate the association between dyskinesia and postural control, balance, gait, and fall risk in individuals with PD. The impact of dyskinesia on this outcome will be assessed over time through longitudinal studies, specifically cohort studies, while case-control studies will be used for cross-sectional analysis.
Protocol registration
On March 18, 2023, this systematic review’s protocol was prospectively registered in the International Prospective Register of Systematic Reviews (PROSPERO)(number CRD42023394684).25 This protocol was planned in accordance with PRISMA-P recommendations,26 and our review will be conducted according t PRISMA recommendations.27
Search strategy
Five electronic databases will be searched for articles: PubMed (http://www.ncbi.nlm.nih.gov/PubMed), CINAHL (www.EBSCO.com), PsycInfo (www.apa.org/pubs/databases/psycinfo/index.aspx), Scopus (www.scopus.com), and SciELO (www.scielo.br). The search strategy was defined using the following terms: ((“Parkinson*”) AND (“Dyskinesia*)) AND (“Gait” OR “Walking”; OR “Ambulation” OR “Accidental Fall” OR “Fall” OR “Postural Balance” OR “Balance” OR “Equilibrium” OR “Postur*” OR “Postural Control” OR “Body Sway”).
Searching other resources
The search for potential articles will include 2 additional steps. First, the reference lists of the included studies will be searched to identify additional articles relevant to the review’s theme. Second, other publications by each author of the included studies will be searched for relevant articles. After these steps, the data extraction procedure will be performed (detailed below). The authors of the included studies will be contacted for additional information when necessary.
Inclusion and exclusion criteria
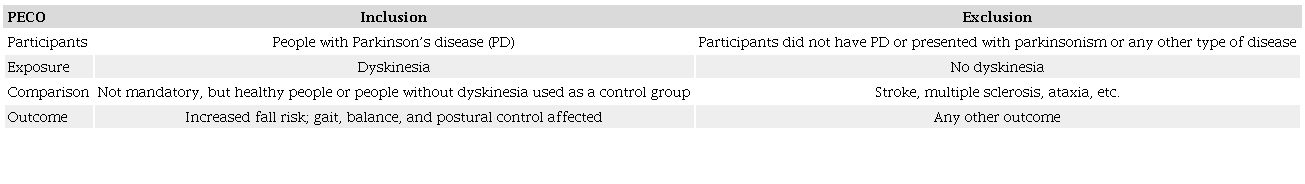
The inclusion and exclusion criteria were developed according to the participants, exposure, comparison, and outcome model (Table 1). Peer-reviewed articles will be included based on the following criteria: dyskinesia assessed in people with PD; assessment of postural control, balance, gait, and fall risk outcomes; longitudinal, cohort (prospective or retrospective), or case-control studies published in English or Portuguese in any year. Articles not including participants with PD will be excluded. Samples including participants with Parkinsonism or other causes of dyskinesia, such as stroke and multiple sclerosis, will not be included. Studies in animal models, review articles, single-case studies, case series, controlled clinical trials, protocol articles, abstracts, conference proceedings, theses, dissertations, letters to the editor, and clinical practice guidelines will not be included.
Study selection
According to PRISMA guidelines, 2 reviewers will independently evaluate the studies’ titles and abstracts. When a study’s eligibility cannot be determined based on the title and abstract, the full article will be evaluated. The 2 reviewers will also read the full text of all studies selected for inclusion. If, after this step, a study’s eligibility still cannot be determined, a third investigator will be invited to help. The study selection process will be presented in a flow chart.
Data extraction
After the screening process, 2 authors will extract the data from all eligible studies. In this review, we will summarize each study according to its characteristics:
- 1. Author(s) and year of publication;
- 2. Sample characteristics (number of participants, ratio of participants’ sex/gender [whichever is reported], time since diagnosis, and country);
- 3. Study design;
- 4. Study aims;
- 5. How dyskinesia was assessed;
- 6. How falls (if prospective, the follow-up duration will be recorded), postural control, balance, and gait were assessed;
- 7. Main and relevant results;
- 8. Study limitations relevant to this review;
- 9. Conclusions.
If necessary, the authors of the included studies will be contacted by email to provide additional information.
Methodological quality assessment
Two reviewers will independently assess the methodological quality of each study, and disagreements will be discussed with a third reviewer. The reviewers will not be blinded to the author(s) or the journal in which the article was published. Instead, a methodological quality assessment will be performed to determine the validity of the findings and possible biases that could affect interpretation of the results. The Newcastle-Ottawa quality assessment scale will be used to assess the methodological quality of the included studies. This scale is divided into 3 categories: selection of study groups (4 items), group comparability (1 item), and outcome determination (3 items). The scale uses a ‘star system’ for assigning points; the higher the study quality, the more stars the study earns (a maximum of 9).
Data synthesis
We will use the PRISMA flow chart to show the number of studies found in each database, duplicates, reasons for exclusion, and the eligible studies. After the search, the complete reference information will be tabulated in Microsoft Excel. Since this review aims to determine whether dyskinesia affects postural control, balance, and gait, increasing fall risk in individuals with PD, the extracted data will be combined and qualitatively presented. The methodological quality of the studies will be summarized based on the overall scores.
Due to the different outcomes, we assume there will be great heterogeneity in study design, methods of outcome assessment and statistical analysis, follow-up duration in cohort studies, data presentation, and methodological quality. If this is the case, no meta-analysis will be conducted and only a qualitative synthesis will be performed. However, if the results are homogeneous, a meta-analysis will be also undertaken.
EXPECTED RESULTS & RELEVANCE
Dyskinesia is a highly relevant issue for individuals with PD and may be considered one of many factors associated with fall risk,4,12 but whether it directly or indirectly affects postural control, balance, and gait in individuals with PD remains unclear. This is the first review to comprehensively and systematically summarize the literature on the association between dyskinesia and postural control, balance, and gait in individuals with PD. Several studies have investigated factors that contribute to falls in individuals with PD,5,12,14 and their findings on the relationship between dyskinesia and falls have been inconsistent. Although many studies have observed an association between dyskinesia and falls,6,12,14,16,17 others have not.4,28,29 Dyskinesia is common in individuals with PD who have previously experienced a fall17 and worsens with disease progression and duration, affecting the limbs, trunk, and head.19 Dyskinesia may significantly affect postural control, balance, and gait and increase fall risk in individuals with PD. Therefore, research into the effects of dyskinesia on postural control, balance, gait, and falls would contribute to our understanding of fall risk in PD. Such information would be critical for new interventions to manage falls and improve quality of life in individuals with PD.
REFERENCES
Allen NE, Schwarzel AK, Canning CG. Recurrent falls in Parkinson’s disease: a systematic review. Parkinsons Dis. 2013;906274. https://doi.org/10.1155/2013/906274
Caetano MJD, Lord SR, Allen NE, Song J, Paul SS, Canning CG, et al. Executive functioning, muscle power and reactive balance are major contributors to gait adaptability in people with Parkinson’s disease. Front Aging Neurosci. 2019;11:154. https://doi.org/10.3389/fnagi.2019.00154
Castro IPR, Valença GT, Pinto EB, Cavalcanti HM, Oliveira-Filho J, Almeida LRS. Predictors of falls with injuries in people with Parkinson’s disease. Mov Disord Clin Pract. 2022;10(2):258-68. https://doi.org/10.1002/mdc3.13636
Murueta-Goyena A, Muiño O, Gómez-Esteban J. Prognostic factors for falls in Parkinson’s disease: a systematic review. Acta Neurol Belg. 2023. https://doi.org/10.1007/s13760-023-02428-2
Pelicioni PHS, Menant JC, Latt MD, Lord SR. Falls in Parkinson’s disease subtypes: risk factors, locations and circumstances. Int J Environ Res Public Health. 2019;16(12):2216. https://doi.org/10.3390/ijerph16122216
Rudzińska M, Bukowczan S, Stozek J, Zajdel K, Mirek E, Chwała W, et al. Causes and consequences of falls in Parkinson disease patients in a prospective study. Neurol Neurochir Pol. 2013;47(5):423-30. https://doi.org/10.5114/ninp.2013.38222
Gazibara T, Kisic-Tepavcevic D, Svetel M, Tomic A, Stankovic I, Kostic VS, et al. Indoor and outdoor falls in persons with Parkinson’s disease after 1 year follow-up study: differences and consequences. Neurol Sci. 2016;37(4):597-602. https://doi.org/10.1007/s10072-016-2504-2
Bloem BR, Grimbergen YA, Cramer M, Willemsen M, Zwinderman AH. Prospective assessment of falls in Parkinson’s disease. J Neurol. 2001;248(11):950-8. https://doi.org/10.1007/s004150170047
Soh SE, McGinley JL, Watts JJ, Iansek R, Murphy AT, Menz HB, et al. Determinants of health-related quality of life in people with Parkinson’s disease: a path analysis. Qual Life Res. 2013;22(7):1543-53. https://doi.org/10.1007/s11136-012-0289-1
Schrag A, Choudhury M, Kaski D, Gallagher DA. Why do patients with Parkinson’s disease fall? A cross-sectional analysis of possible causes of falls. NPJ Parkinsons Dis. 2015;1:15011. https://doi.org/10.1038/npjparkd.2015.11
Herman T, Barer Y, Bitan M, Sobol S, Giladi N, Hausdorff JM. A meta-analysis identifies factors predicting the future development of freezing of gait in Parkinson’s disease. NPJ Parkinsons Dis. 2023;9(1):158. https://doi.org/10.1038/s41531-023-00600-2
Fasano A, Canning CG, Hausdorff JM, Lord S, Rochester L. Falls in Parkinson’s disease: a complex and evolving picture. Mov Disord. 2017;32(11):1524-36. https://doi.org/10.1002/mds.27195
Latt MD, Lord SR, Morris JGL, Fung VSC. Clinical and physiological assessments for elucidating falls risk in Parkinson’s disease. Mov Disord. 2009;24(9):1280-9. https://doi.org/10.1002/mds.22561
Paul SS, Sherrington C, Canning CG, Fung VSC, Close JCT, Lord SR. The relative contribution of physical and cognitive fall risk factors in people with Parkinson’s disease: a large prospective cohort study. Neurorehabil Neural Repair. 2014;28(3):282-90. https://doi.org/10.1177/1545968313508470
Cenci MA, Riggare S, Pahwa R, Eidelberg D, Hauser RA. Dyskinesia matters. Mov Disord. 2020;35(3):392-6. https://doi.org/10.1002/mds.27959
Lima D P, de-Almeida SB, Bonfadini JC, Carneiro AHS, Luna JRG, Alencar MS, et al. Falls in Parkinson’s disease: the impact of disease progression, treatment, and motor complications. Dement Neuropsychol. 2022;16(2):153-61. https://doi.org/10.1590/1980-5764-DN-2021-0019
Rascol O, Perez-Lloret S, Damier P, Delval A, Derkinderen P, Destée A, et al. Falls in ambulatory non-demented patients with Parkinson’s disease. J Neural Transm (Vienna). 2015;122(10):1447-55. https://doi.org/10.1007/s00702-015-1396-2
Rascol O, Fabre N, Brefel-Courbon C, Ory-Magne F, Perez-Lloret S. Dyskinesias. In: Kompoliti K, Metman LV, editors. Encyclopedia of movement disorders. Oxford: Academic Press; 2010. p. 350-61.
Colosimo C, Martínez-Martín P, Fabbrini G, Hauser RA, Merello M, Miyasaki J, et al. Task force report on scales to assess dyskinesia in Parkinson’s disease: critique and recommendations. Mov Disord. 2010;25(9):1131-42. https://doi.org/10.1002/mds.23072
Yang K, Zhao X, Wang C, Zeng C, Luo Y, Sun T. Circuit mechanisms of L-DOPA-Induced Dyskinesia (LID). Front Neurosci. 2021;15:614412. https://doi.org/10.3389/fnins.2021.614412
Thanvi B, Lo N, Robinson T. Levodopa-induced dyskinesia in Parkinson’s disease: Clinical features, pathogenesis, prevention and treatment. Postgrad Med J. 2007;83(980):384-8. https://doi.org/10.1136/pgmj.2006.054759
Kumar N, Van Gerpen JA, Bower JH, Ahlskog JE. Levodopa-dyskinesia incidence by age of Parkinson’s disease onset. Mov Disord. 2005;20(3):342-4. https://doi.org/10.1002/mds.20360
Van Gerpen JA, Kumar N, Bower JH, Weigand S, Ahlskog EJ. Levodopa-associated dyskinesia risk among Parkinson disease patients in Olmsted County, Minnesota, 1976-1990. Arch Neurol. 2006;63(2):205-9. https://doi.org/10.1001/archneur.63.2.205
Lindholm B, Eek F, Skogar Ö, Hansson EE. Dyskinesia and FAB score predict future falling in Parkinson’s disease. Acta Neurol Scand. 2019;139(6):512-8. https://doi.org/10.1111/ane.13084
Santos LHCC, Freitas SMSF, Garbus RBSC, Garcia TH, McDonald K, Alty J, et al. The effect of dyskinesia on postural control, balance, gait and risk of falling in people with Parkinson’s disease: a systematic review [Internet]. Prospective Register of Systematic Reviews. 2023;1-5. Available from: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42023394684. Accessed in Mar 18, 2023.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4(1):1. https://doi.org/10.1186/2046-4053-4-1
Page M, McKenzie J, Bossuyt P, Boutron I, Hoffmann T, Mulrow C, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71
Custodio N, Lira D, Herrera-Perez E, Montesinos R, Castro-Suarez S, Cuenca-Alfaro J, et al. Predictive model for falling in Parkinson disease patients. eNeurologicalSci. 2016;5:20-4. https://doi.org/10.1016/j.ensci.2016.11.003
Hoskovcová M, Dušek P, Sieger T, Brožová H, Zárubová K, Bezdíček O, et al. Predicting falls in parkinson disease: what is the value of instrumented testing in OFF medication state? PLoS One. 2015;10(10):e0139849. https://doi.org/10.1371/journal.pone.0139849
Notes
Not applicable.
The authors followed the PRISMA guidelines, which is reported in the manuscript.
Notes
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – Finance Code 001 and the São Paulo Research Foundation (FAPESP) (2022/14200-0) (Lucas H.C.C. Santos)”.
Author notes
Correspondence data Paulo Henrique Silva Pelicioni – Wallace Wurth building, room 205 – University of New South Wales, Randwick, 2031 – New South Wales, Australia. E-mail: paulo.silvapelicioni@unsw.edu.au
Conflict of interest declaration
Associate Professor Jane Alty declared the following clinflicts of interest: (i) NHMRC Ideas grant (Research) 2021-2025; (ii) RHHRF Major Project grant 2022-24; (iii) Taylor and Francis/ CRC; (iv) Stada Ltd; (v) Michael J Fox foundation – to attend GP2 Parkinson’s investigators meetings 2023; (vi) Shake It Up Australia Foundation – to attend World Parkinsons Congress 2023. The other authors declare no conflicts of interest.
