Article
Contributions of Health Literacyfor Patient Safety in Primary Care: A Scoping Review
Aportaciones de la alfabetización en salud a la seguridad del paciente en atención primaria: una revisión de alcance
Contribuições do letramento em saúde para a segurança do paciente na atenção primária: scoping review
Contributions of Health Literacyfor Patient Safety in Primary Care: A Scoping Review
Aquichan, vol. 24, no. 1, e2414, 2024
Universidad de La Sabana
Received: 21 June 2023
Accepted: 24 November 2023
Abstract
Introduction: This study provides unprecedented scientific evidence for the expansion of health literacy as a tool capable of increasing patient safety through effective communication between health care professionals and their patients, especially in primary health care.
Objective: To map the evidence available regarding the impact of health literacy on care safety for adult patients in primary health care.
Materials: and methods: This is a scoping review in line with the Joanna Briggs Institute method, which covers care, techniques, protocols, or health literacy methods used to improve primary health care. The Medline (PubMed), Web of Science, Scientific Electronic Library Online (SciELO), Virtual Health Library, Scopus, Cinahl, and Google Scholar databases were used for the gray literature search. Original studies available in full and published until January 2023, in all languages covering the topic, were included. Two reviewers screened them by title and abstract, and three reviewers read the full texts and extracted data from the selected articles presented in flowcharts, tables, and descriptive narratives.
Results: A total of 3749 studies were found, of which 23 were selected. From these, the following categories emerged: ‘The impact of health literacy on the engagement and health outcomes of primary health care users;’ ‘Interventions that contribute to health literacy in primary health care;’ and ‘Evaluation of users’ and professionals’ perspectives on health literacy.’
Conclusions: Health literacy interventions focused on primary care should be encouraged within health care services to promote care, prevent illnesses, and inspire the population’s transformation process, with a direct impact on patient safety.
Keywords (Source: DeCS) Health literacy+ patient safety+ primary health care+ nursing+ patient-centered care.
Resumen
Introducción: el estudio aporta evidencias científicas sin precedentes para la expansión de la alfabetización en salud como herramienta capaz de aumentar la seguridad del paciente a través de una comunicación eficaz entre los profesionales de la salud y sus pacientes, especialmente en atención primaria.
Objetivo: mapear la evidencia sobre el impacto de la alfabetización en salud en la seguridad de la atención a pacientes adultos en atención primaria.
Material y método: revisión exploratoria según el método del Instituto Joanna Briggs, en la que se contemplaron cuidados, técnicas, protocolos o métodos de alfabetización en salud utilizados para mejorar la atención primaria de salud. Se utilizaron las bases de datos Medline (PubMed), Web of Science, Scientific Electronic Library Online (SciELO), Virtual Health Library, Scopus, Cinahl y Google Scholar para la literatura gris. Se incluyeron los estudios originales disponibles en su totalidad, publicados hasta enero de 2023, en todos los idiomas que cubrían el tema. Dos pares seleccionaron por título y resumen, y tres pares leyeron los textos completos y extrajeron los datos de los artículos seleccionados, que se presentaron en flujogramas, tablas y narrativas descriptivas.
Resultados: se encontraron 3749 estudios, de los que se seleccionaron 23. De ellos surgieron las siguientes categorías: “impacto de la alfabetización en salud sobre el compromiso y los resultados en salud de los usuarios de atención primaria”; “intervenciones que contribuyen a la alfabetización en salud en atención primaria” y “evaluación de las perspectivas de los usuarios y los profesionales sobre la alfabetización en salud”.
Conclusiones: las intervenciones de alfabetización en salud centradas en la atención primaria deben fomentarse en los servicios de salud para promover la atención, prevenir enfermedades e inspirar el proceso de transformación de la población, lo que repercute directamente en la seguridad de los pacientes.
Palabras clave (Fuente DeCS): Alfabetización en salud, seguridad del paciente, atención primaria de salud, enfermería, atención dirigida al paciente.
Resumo
Introdução: este estudo traz evidências científicas inéditas para a ampliação do letramento em saúde, como uma ferramenta capaz de aumentar a segurança do paciente através da comunicação eficaz entre os profissionais de saúde e seus pacientes, em especial nos cuidados primários em saúde.
Objetivo: mapear evidências sobre o impacto do letramento em saúde na segurança do cuidado de pacientes adultos da atenção primária à saúde.
Materiais e método: revisão de escopo de acordo com o método do Instituto Joanna Briggs, em que foram contemplados cuidados, técnicas, protocolos ou métodos de letramento em saúde utilizados para melhorar a assistência primária à saúde. Utilizaram- se as bases Medline (PubMed), Web of Science, Scientific Electronic Library Online (SciELO), Biblioteca Virtual em Saúde, Scopus, Cinahl e Google Acadêmico na literatura cinzenta. Foram incluídos estudos originais disponíveis na íntegra, publicados até janeiro de 2023, em todos os idiomas que englobassem a temática. Dois revisores realizaram a triagem por título e resumo, e três revisores leram os textos completos e extraíram dados dos artigos selecionados, sendo apresentados através de fluxo, tabela e narrativa descritiva.
Resultados: foram encontrados 3749 estudos, dos quais 23 foram selecionados. Destes, surgiram as seguintes categorias: “impacto do letramento em saúde no engajamento e desfechos de saúde de usuários da atenção primária à saúde”; “intervenções que contribuem para o letramento em saúde na atenção primária à saúde” e “avaliação das perspectivas de usuários e profissionais quanto ao letramento em saúde”.
Conclusões: intervenções para o letramento em saúde com foco nos cuidados primários devem ser estimuladas dentro dos serviços de saúde a fim de promover o cuidado, prevenir agravos e inspirar o processo de transformação da população, impactando diretamente na segurança do paciente.
Palavras-chave (Fonte DeCS): Letramento em saúde, segurança do paciente, Atenção Primária à Saúde, enfermagem, assistência centrada no paciente.
Introduction
‘Health literacy’ is the expression used to describe the ability to use information in health care services. It concerns the personal characteristics and social resources necessary for individuals and communities to access, understand, evaluate, and use information and services to make health-related decisions. It includes the ability to communicate, assert, and act upon such decisions (1-4).
The health literacy approach and shared decision-making are considered important tools that increase patient safety and improve communication between health care professionals and their patients (5, 6), which can favor better patient participation and autonomy in their care process. In this sense, the Agência Nacional de Vigilância Sanitária (National Health Surveillance Agency) guidelines emphasize the combination of health literacy and patient safety by improving the communication process which is essential for the development of a partnership relationship. Health care services with a safety culture centered on patient and family care must ensure the quality of communication at all levels of care as an integral part of health care (7, 8).
Primary health care (PHC) is considered to be the patient’s gateway to the Brazilian Unified Health System (better known by its acronym, SUS), where first contact takes place and basic care is provided by the health care services in which the population concerned lives or works (1, 9, 10). Even though they are in the same territory, PHC can come across a variety of people at different levels, who, to be welcomed in a comprehensive and qualified way, require an approach based on health literacy so that communication is effective (11, 12).
In the Shanghai Declaration 2020/2030, three cornerstones were established to promote health: Good governance, healthy cities, and health literacy. Health literacy was widely discussed at this conference, which took place in 2016 (1). Since then, the aim has been to improve it through better access to information and to enable people to make more informed decisions about their health and that of their families, from which they can more effectively advocate their political views and formulate adequate public policies (3, 13-15).
Health promotion addresses this wide range of determinants through a combination of strategies, including health promotion in all policies and the creation of supportive health environments; it also improves personal health literacy and health competencies. The drive to address health determinants is intrinsically linked to health equity and is fundamentally concerned with the distribution of power and resources within populations (14, 16-19).
The aim of studies on health literacy and patient safety is to help transform health care organizations into health literacy-responsive organizations, redesigning their structures and processes to support patients with low levels of health literacy to understand and use information and services to maintain their own health (20-22).
However, there is a growing need to further understand the effects of personal care experiences (e.g., patient-centered care) and patient-specific factors (e.g., socioeconomic status, health beliefs, level of health literacy) on patient-reported outcomes regarding health care provision quality (e.g., satisfaction with care). Improved insights into these interrelationships would enable the development of measures to initiate organizational change toward a more patient-centered and health literacy-friendly environment.
Initially, a preliminary search was conducted using the following descriptors: ‘Health literacy,’ ‘patient safety,’ and ‘primary care’ in the PubMed, Cochrane Systematic Reviews, and the Joanna Briggs Institute (JBI) Evidence Synthesis databases; no systematic, integrative, narrative, or scoping reviews covering the theme were found.
In this setting, the following research question was raised, based on the PCC strategy (population, concept, and context), which will be addressed below: How can health literacy contribute to the safety of PHC patients? Based on this, the review aimed to map the evidence regarding the impact of health literacy on care safety for adult PHC patients.
Materials and Methods
The present study was done following the JBI methodology for scoping reviews (23). The protocol was prospectively registered in the Open Science Framework (https://osf.io/8xjb9/?view_only=8d67d5618bf34fffa013d7f407a9cbfb ).
This scoping review covered experimental and quasi-experimental study designs, including randomized clinical trials, non-randomized controlled trials, before-and-after studies, and interrupted time series studies. Analytical observational studies, including prospective and retrospective cohort studies, case-control studies, and analytical cross-sectional studies were also covered. Descriptive observational studies, including case series, individual case reports, and descriptive cross-sectional studies were included. Qualitative studies focused on qualitative data were covered, including but not limited to projects such as phenomenology, grounded theory, ethnography, qualitative description, action research, and feminist research. In addition, texts and opinion pieces, as well as systematic reviews that met the inclusion criteria were also included, depending on the research question.
The search for articles was based on the descriptors indexed in the Medical Subject Headings (MeSH)/Descriptors in Health Sciences (DeCS): ‘Health literacy,’ ‘primary health care,’ ‘patient safety,’ and ‘risk management,’ using the Boolean operators AND and OR (Table 1).

Source: Research data.
Search Strategy
The search strategy aimed to find published and unpublished studies and was performed in three steps. The first search, which was done in December 2022, consisted of an initial search in the electronic databases Medline (PubMed) and Virtual Health Library. Next, the words contained in the title, abstract, and keywords of the articles found were analyzed. The descriptors were compared to those registered in MeSH for searches in PubMed, while DeCS was used for searches in the Virtual Health Library (VHL).
In the second step, which was done in February 2023, the search strategy, including all the keywords and indexing terms identified, was adapted for each database and/or information source included. The search strategy was tested by two reviewers. The following databases were included: Medline (PubMed), Web of Science, Scientific Electronic Library Online (SciELO), VHL, Scopus, Cinahl, and Google Scholar in the gray literature (Table 2). The reference list of all the evidence sources included was examined for additional studies in April 2023. The third stage was done between March and May 2023, with the extraction and analysis of data from all the selected studies.

Source: Research data.
Inclusion Criteria
The PCC strategy was used to draw up the research question in which: Population refers to studies where the participants were users of PHC services, in this case, adults who received health care (excluding studies where participants received home care); concept refers to studies that addressed care, techniques, protocols, or health literacy methods used to improve health care; context refers to studies on patient safety, patient engagement and/or self-management in PHC. Patient safety entails not subjecting the user to avoidable risks resulting from the care or assistance provided, as well as preventing any complications (7). Thus, all studies that addressed this context along with the concept and participants described above were included in the search.
Original studies available in full, classified in line with the JBI Sumari and their methodological potential, as well as gray literature, were also included. The studies included had been published until February 2023, in all languages, and covered the review theme. Publications on websites, editorials, and book chapters were excluded.
Study Selection and Evidence Source
After the search, all the identified citations were grouped and uploaded to the Mendeley V.1.19.4 bibliographic software and duplicates were removed. After a pilot test, the titles and abstracts were then screened by three independent reviewers to assess the inclusion criteria for the review. Potentially relevant sources were retrieved in full and their citation details were imported into the JBI System for unified information management, evaluation, and review (JBI Sumari [24]).
The full text of the selected citations was assessed in detail according to the inclusion criteria by three independent reviewers. The reasons for excluding evidence sources in the full text that did not meet the inclusion criteria were recorded and reported. Any disagreements that emerged between the reviewers at each step of the selection process were settled through discussion or by consulting one or more additional reviewers. The results of the search and study inclusion process were reported in full in the final scoping review and were presented in a flow diagram (Figure 1) of Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR [25]).
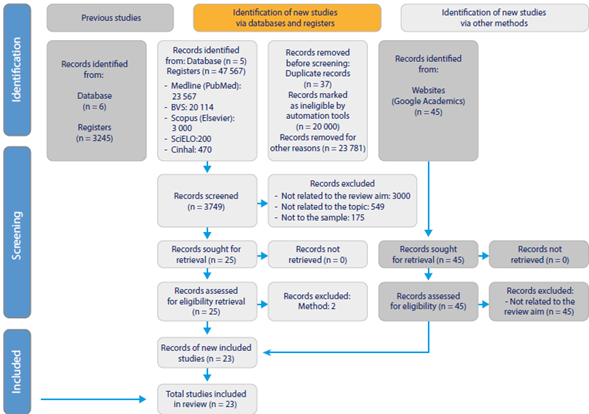
Figure 1
Flowchart for the Search and Selection Process of Studies for the Scoping Review
Source: Based on (25).
Data Extraction
Both reviewers used the JBI Sumari tool to extract the data from the studies included in this review. After this step, the data were presented in a table with the following information: Article title, publication year, country, study objective, population/sample, study design, main conclusions, findings related to the question of this scoping review, and levels of evidence. To classify the level of evidence of the materials selected in this review, the guidelines of Melnyk and Fineout-Overholt (26) were used (Table 3). Disagreements between the reviewers, when found, were settled by a third reviewer.
Data Analysis and Presentation
The results were expressed through narrative synthesis, tables, and charts, pointing to the relevant characteristics found in the mapped objective in the scoping review.
Results
Study Inclusion
Of the 23 studies selected, 6 were published in 2020; 3 were published in 2022; followed by 4 studies in 2016; 3 studies in 2014 and 2017; 2 studies in 2022; and only 1 study was published in each of the following years: 2013, 2015, 2018, 2019, and 2021 (Figure 2).
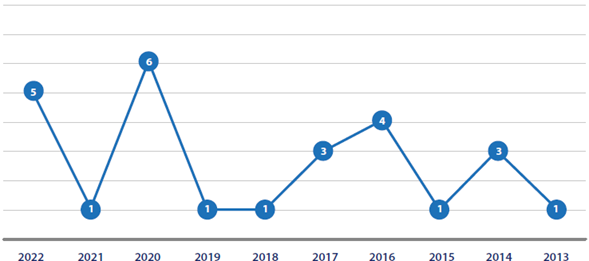
Figure 2
Distribution of Publication Periods by Year (N = 23). Brasília, Distrito Federal, 2023
Source: Research data.
Regarding the country where the studies were conducted, most of them (11) were done in the United States; 3 studies in the United Kingdom; 2 studies in Germany, Japan and Australia; and only 1 study in Sweden, Spain, and China (Figure 3).
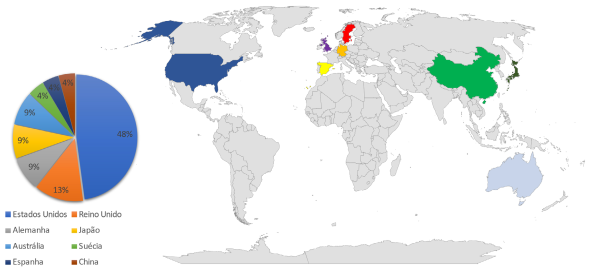
Figure 3
Distribution of Publications by Country (N = 23). Brasília, Distrito Federal, 2023
Source: Research data.
The data extracted from the articles is shown in Table 4 for a better overview of the information related to the objectives and questions posed by the present study.

Source: Prepared by the authors.
Discussion
To discuss the evidence found in this review, the following categories were delimited: ‘The impact of health literacy on patient safety in PHC;’ ‘Interventions that contribute to health literacy in PHC,’ and ‘The assessment of users’ and professionals’ perspectives on health literacy.’
The Impact of Health Literacy on Patient Safety in PHC
The framework used to design health literacy interventions targets learning stimulation and motivation, recognizing that patient involvement in the learning process is likely to be a key contributing factor to their ability to understand and act on health-related recommendations (49). For this purpose, it is necessary to develop strategies that meet their preferences and needs effectively, in balance with the provider’s knowledge, skills, and structural constraints (39).
Health literacy can be a key factor in the self-management of care, as shown in a study that assessed adherence to the use of oral anticoagulants in patients with cardiovascular diseases. Patients with higher levels of health literacy reported being confident in their ability to manage information, empowerment, and self-efficacy. In addition, they had better self-care, treatment management, excellent appointment attendance, and fewer complications, room admissions and hospitalizations (34). A cluster-randomized controlled study aiming to carry out high-quality blood pressure monitoring at home found that interactive group education and subsequent individual counseling can reduce the rate of patients with uncontrolled hypertension compared to conventional individual counseling. Positive effects were found in patients with both adequate and inadequate health literacy (37).
Patient-centered care that respects individual preferences and needs is attainable when health care organizations strengthen interpersonal relationships and shift away from disease-oriented care, trying to produce the best outcome for the patient (29). Some aspects that should be considered in decision-making are information provision / patient education (focused on benefits and risks), clear medical doctor-patient communication and structure for decision-making (39).
A randomized controlled trial (28), using data registered in the Patient-Physician Partnership, evaluated the effectiveness of intensive interventions directed to patients and medical doctors to improve adherence among hypertensive patients. There were no significant differences in the desire of users with low and adequate literacy levels to become engaged with their health care. However, users with a lower level of health literacy asked fewer questions, while still asking those of a psychosocial nature, and experienced less shared decision-making, whereby the medical decision was imposed (28).
In this context, health literacy saw a significant improvement following the educational intervention. Valuing the patient’s role based on their own knowledge led to a change in the beliefs and behaviors of health care service users who became active participants in the system. Investing in the motivation of individuals to learn about health care systems and to collaborate with their health care providers with the necessary knowledge and skills can enable them to maintain and promote their own health and that of their families and loved ones (40).
Communication is among the international goals for patient safety, since it is vital for individuals living in society, especially in the health and illness process (30). Patients with limited health literacy tend to not understand or remember the content of the health education offered by their primary care provider (30). Another study (38) found that parents with poor health literacy experience worse outcomes and care deficits in terms of their children’s health. Poor communication compromises safety and leads to patient and family dissatisfaction with health care (38).
It is worth understanding that patients seek different types of information beyond technical aspects; they also consider the recommendations, the step-by-step process, and knowing what should be expected from a process involving their health. Due to the time constraints of appointments, professionals and patients find it beneficial to offer tools and professionals who can reiterate the educational content, summarize what health decisions have been made, and support the continued retention of information in environments outside the doctor’s office (39).
Health literacy can be improved by providing information, effective communication, and structured education, in which health care professionals can personalize and target care according to the user’s profile (40). The various cultures, traditions and the context in which they live must be considered for adapting the most suitable strategy to be used (41). A study carried out with refugees in Australia mentions the importance of an interface with facilitators who can help them make decisions (41). A multifaceted approach involving patients, communities, and health care professionals is ideal.
Interventions that contribute to health literacy in PHC
Health literacy strategies can be taught, and skill learning can be measured (49). Health care professionals, regardless of their category, have a key role to play in the development of health systems’ capacity to address health literacy to ensure that they meet users’ literacy needs (38, 46). However, a large number of health care professionals are unaware of alternative strategies that can improve and facilitate communication with users. In this sense, it is essential that health care professionals who provide direct care to patients know the principles of health literacy and how to implement them in practice, as this is a necessary step to promote safety and improve care in all contexts, including primary care (38).
The lack of information continuity and transfer between patients and several different health care professionals has been identified as a source of uncertainty and vulnerability among primary care users in Switzerland (27). Interactive professional-centered interventions were associated with improved knowledge, behaviors, and confidence among team members regarding the use of health literacy strategies. This type of study can lead to better outcomes, such as the prevention of misunderstandings related to medication, immunization, and preventive care (49).
In one study, a pop-up notification was implemented in the electronic medical record system so that medical doctors and nurses, when providing care to a patient at risk of low health literacy, could apply the health literacy knowledge learned during the educational intervention (46). Pictogram-based medication instruction sheets, written at a lower level of health literacy, along with demonstration, teach-back/ show-back and the availability of dosing tools can complement these professionals’ verbal advice and reduce dosing errors (49).
Three studies (45-47) used digital resources as their intervention, one of which highlighted that the level of user engagement can vary according to health literacy, spoken language proficiency, and digital literacy. A better understanding of how to consider, define, and incorporate digital literacy when developing health-related information technology is needed, as well as continued efforts to better engage vulnerable populations in research. Ownership of a smartphone, even with daily personal use, does not accurately predict comfort or ability to use basic phone features such as text messaging (45).
It is important to ensure that an intervention is effective, efficient, and sustainable (38). Adequately monitoring the quality of a study and the various stages of a complex intervention, along with meticulous planning of a pilot study that tests unrecognized variability sources, is a must before implementing essential intervention studies (47). Two interventions targeting digital health literacy did not produce a statistically significant effect (45, 47), presenting various limitations and problems in their implementation, such as difficulty in understanding the proposal by the target population; inadequacy and inefficiency of the technique applied; low engagement (45); short implementation period of the intervention; no access to the proposed digital tool; and a high drop-out rate among study participants (47).
The effectiveness of interventions can be maximized when they are in line with and based on the best and most recent scientific evidence and through feedback from the target population (46). The creation of realistic practical scenarios relating to the primary care environment also leads to an increased possibility that participants will recognize how the principles of health literacy can be applied (38). Although a shorter training period may be more attractive to busy professionals, a full day of health literacy training may be necessary to address all the relevant issues of the educational intervention, which corroborates the literature findings on the subject (46).
Other factors that increase the effectiveness of the educational intervention entail multi-component training with small group work and role-playing; identifying barriers to changes and devising plans to overcome them; and involving a local opinion leader and/or team representative in the training (46).
The Assessment of Users’ and Professionals’ Perspectives on Health Literacy
Health literacy is a predictor of individual health status and enables the identification of people in vulnerable situations and the effective management of health inequalities. A study (34) has shown a strong relationship between the dimensions of health literacy and the social determinants that comprise the axes of health inequality (34).
In PHC, patient safety goes beyond technical measures and includes the relational context of care, which is responsive to the patient’s priorities and must be agreed upon between health care professionals and patients. Different needs must be addressed and active communication with patients is recommended to avoid making assumptions about their capacity and priorities. Participatory design studies seem to be useful for understanding not only how a recommendation should be perceived, but also how it should feel in practice (42).
In a qualitative study, semi-structured interviews were conducted with refugee health care leaders, pharmacists, nurses, and general practitioners to explore the barriers and facilitators to quality medication use experienced in the PHC setting in Australia. Five barriers were found: communication, language restriction, cultural issues, limited health literacy, and financial costs. Communication barriers were the most common and impacted quality access to medication, which highlighted the vital role of interpreters and training for health care professionals in providing cross-cultural care. Collaboration between health care professionals can improve the safe use of medication and users can benefit from a medication review carried out by a pharmacist. Low health literacy in a person’s mother tongue can limit the effectiveness of translated resources, although written information is useful. In addition, pictograms designed to support medication instructions for consumers with low health literacy can be misinterpreted, especially in cross-cultural contexts (41).
Most users are willing to trust the health care system and its professionals, but a lack of communication and continuity of care is an obstacle. PHC users in Switzerland rated the language skills of health care professionals as poor, hindering the establishment of a bond. The stress caused by the reduction of the minimum time spent in each appointment resulted in feelings of incomprehension and aversion by patients towards health care professionals. Furthermore, the lack of information continuity and transfer between patients and several different health care professionals has been identified as a source of uncertainty and vulnerability (27).
The perception of systemic inertia inherent to PHC has a negative influence on user satisfaction, which impacts aspects such as monitoring and receiving test results (27). According to an American study that assessed the communication of test results, the responsibility for communicating test results is not clear among health care professionals; communication does not follow standards or protocols and normal results are not commonly reported. The communication of abnormal results by non-health care professionals, as they have no knowledge of how to clarify doubts, leads to anxiety among patients (43).
Effectiveness in communication is needed at several stages of the health and illness process, as shown in a study assessing breast cancer patients’ perspectives on information regarding their care and survival plan. According to a study (33), a written document with a survival plan is no replacement for direct communication with professionals about treatment, symptom management and transition, which was assessed as a failure by the participants. In the absence of information, patients turned to peer support and community organizations. Data suggests that patients are less interested in a treatment summary and more interested in information and education regarding what to do and how to manage survival. Some women report the need for better communication related to side effects, pain, healthy eating, and reconstructions. This lack of information leads to concern, fear, and anxiety in patients (33).
Health literacy is part of the complexity inherent to health care services, which must provide tools to improve written, oral, and documental communication to improve patient-centered care. A study (35) evaluated the level of health literacy of patients at a medical center in the United States through an initial screening and the information included in the patient’s record, based on a model of improvement in which health care professionals participated in the training. The participating nurses adopted the new process quickly and reported it as beneficial for patient education discussions. A key facilitator for the adoption and acceptability of the instrument being evaluated was the support of the leadership and the integration of all stages of the project into the existing infrastructure and workflows. The initiative promoted change in the nursing team’s practice and provided important information regarding barriers and facilitators to health literacy. The evaluation of health literacy enabled the team to increase their awareness of low health literacy among the patients they treated, which allowed them to develop adequate resources, carry out large-scale research into the consequences of low health literacy, and evaluate the effect of the system’s interventions according to patients’ level of health literacy (35).
Implementing the assessment of users’ level of health literacy and training health care professionals to use it routinely can improve the quality of care and promote healthier long-term outcomes. An exploratory cross-sectional study evaluated the perceptions and perspectives of patients and professionals regarding the use of the Newest Vital Sign health literacy assessment tool. It showed that health care professionals, especially medical doctors, are unaware of the tools needed to assess patients’ literacy. At the study’s conclusion, the routine application of the Newest Vital Sign tool was recommended during the user’s admission appointment, since it covers the various dimensions of health literacy, is quick (3-5 minutes) and easy to apply by professionals and acceptable to users (44).
A study assessed patients’ perceptions of the Universal Medication Schedule to expand it. According to the participants, clear and concise words and sentences should be used whenever possible; in addition, there was a greater acceptance of the term ‘half’ instead of the fraction ‘½’. Improving prescriptions is not enough to promote safe and consistent medication use, and additional support for patients is needed. Participants suggested that dosage instruments should be made available, since measurements can vary and are not well known. They also asked for the maximum dosage of painkillers to be specified and for the use of medication to be linked to specific times (32).
Conclusions
The contributions of health literacy are vast since patients and professionals become partners and get involved in the search for safe, quality care, where the focus is placed on patients and their individual needs. The impact may not be noticeable immediately, as the established safety culture requires time to change, but this process of reflection and change must be initiated. Communication is the keyword, but it also presents a daily challenge within the context of health care teams. Engaging patients and their families with strategies that enable a comprehensive assessment of health conditions and consider individual variations in each context is essential in terms of primary health care. Creative and more visual strategies facilitate understanding and improve acceptance of what is new. Synthesizing the results can contribute to decision-making and guiding care practices, leading to increased safety for both patients and the professional teams in PHC.
The impact of using strategies based on health literacy assists communication, patient engagement in their care and, consequently, the safety of care in PHC. Health care based on evidence-based pillars that ensure patient safety emphasizes the need for health-literate patients who understand their role in the health-disease process, focusing on health promotion and prevention, which are the foundations of PHC care.
References
Astier-Peña MP, Martínez-Bianchi V, Torijano-Casalengua L, Ares-Blanco S, Bueno-Ortiz JM, et al. El Plan de acción mundial para la seguridad del paciente 2021-2030: identificando acciones para una atención primaria más segura. Aten Primaria [Internet]. 2021;53:102224. DOI: https://doi.org/10.1016/j.aprim.2021.102224
World Health Organization (WHO). Health promotion glossary of terms 2021. Geneva; 2021.
World Health Organization (WHO). Health literacy development for the prevention and control of noncommunicable diseases [Internet]. Genebra; 2022 [citado 13 abril 2023]. Disponível em: Disponível em: https://www.who.int/publications/i/item/9789240055391
Kim MT, Kim KB, Ko J, Murry N, Xie B, Radhakrishnan K et al. Health literacy and outcomes of a community-based self-help intervention: A case of Korean Americans with type 2 Diabetes. Nurs Res [Internet]. 2020;69(3):210-8. DOI: https://doi.org/10.1097/NNR.0000000000000409
Durrant LA, Taylor J, Thompson H, Usher K, Jackson D. Health literacy in pressure injury: Findings from a mixed-methods study of community-based patients and carers. Nurs Health Sci [Internet]. 2019;21(1):37-43. DOI: https://doi.org/10.1111/nhs.12429
Serbian AK, Santos NO Dos, Paskulin LMG. Effects of the Alpha-Health intervention on elderly’s health literacy in primary health care. Rev Bras Enferm. 2022;75(supl. 4):e20200978. DOI: https://doi.org/10.1590/0034-7167-2020-0978
Brasil. Assistência segura: uma reflexão teórica aplicada à prática. 2a ed. Brasília: Agência Nacional de Vigilância Sanitária; 2017.
Murugesu L, Heijmans M, Rademakers J, Fransen MP. Challenges and solutions in communication with patients with low health literacy: Perspectives of healthcare providers. PLoS One. 2022;17(5):e0267782. DOI: https://doi.org/10.1371/journal.pone.0267782
Lima RIM, Parente MA, Ferreira TISP, Coelho AAS, Loureiro EVS de, Barbosa TM et al. Letramento funcional em saúde de usuarios da atenção primária de Altamira, Pará. Revista Brasileira de Medicina de Família e Comunidade. 2022;17(44):2763. DOI: https://doi.org/10.5712/rbmfc17(44)2763
Macinko J, Mendonça CS. Estratégia Saúde da Família, um forte modelo de Atenção Primária à Saúde que traz resultados. Saúde em Debate [Internet]. 2018 [citado 15 abril 2023];42(esp. 1):18-37. DOI: DOI: https://doi.org/10.1590/0103-11042018s102
Ghalenow H, Nikpeyma N, Kazemnejad A, Ansari M, Pashaeypoor S. Effect of educational program based on health literacy index on self-care ability among older adults: A randomized clinical trial. Int J Prev Med. 2022;13(1). https://doi.org/10.4103/ijpvm.IJPVM_506_20
Persai D, Balu RK, Singh K, Prabhu RR, Lahoti S, Rout S et al. Patient satisfaction with quality of primary care health servicesfindings from India. Int J Health Plann Manage. 2022;37(4):2256-65. DOI: https://doi.org/10.1002/hpm.3467
Xiang Yang BR, Professor A, Xia LR, Luo DR, Liu QR, Jun Kang LB et al. Relationship between eHealth literacy and psychological status during COVID-19 pandemic: A survey of Chinese residents Post-graduate Student. J Nurs Manag. 2021;29(4):805-12. DOI: https://doi.org/10.1111/jonm.13221
World Health Organization. (2017). Promoting health in the SDGs: report on the 9th Global conference for health promotion, Shanghai, China, 21-24 November 2016: All for health, health for all. World Health Organization. https://iris.who.int/handle/10665/259183
Dias S, Gama A, Maia AC, Marques MJ, Campos Fernandes A, Goes AR, et al. Migrant communities at the center in co-design of health literacy-based innovative solutions for non-communicable diseases prevention and risk reduction: Application of the OPtimising HEalth LIteracy and Access (Ophelia) Process. Front Public Health [Internet]. 2021;9. DOI: https://doi.org/10.3389/fpubh.2021.639405
Nutbeam D, Muscat DM. Health Promotion Glossary 2021. Health Promot Int. 2021;36(6):1578-98. DOI: https://doi.org/10.1093/heapro/daaa157
Okan O, Bauer U, Levin-Zamir D, Pinheiro P, Sørensen K. International handbook of health literacy: Research, practice and policy across the lifespan. Bristol; 2019. p. 768. DOI: https://doi.org/10.56687/9781447344520
World Health Organization (WHO). Plano de ação global para a segurança do paciente 2021-2030: em busca da eliminação dos danos evitáveis nos cuidados de saúde. Genebra; 2021.
Jansen CJM, Van’T Jagt RK, Reijneveld SA, van Leeuwen E, de Winter AF, Hoeks JCJ. Improving health literacy responsiveness: A randomized study on the uptake of brochures on doctor-patient communication in primary health care waiting rooms. Int J Environ Res Public Health. 2021;18(9):5025. DOI: https://doi.org/10.3390/ijerph18095025
Visscher BB, Steunenberg B, Heijmans M, Hofstede JM, Devillé W, van der Heide I et al. Evidence on the effectiveness of health literacy interventions in the EU: a systematic review. BMC Public Health [Internet]. 2018;18(1):1414. DOI: https://doi.org/10.1186/s12889-018-6331-7
Fernandez-Gonzalez L, Bravo-Valenzuela P. Effective interventions to improve the health literacy of cancer patients. Ecancermedicalscience. 2019;13. DOI: https://doi.org/10.3332/ecancer.2019.966
Chang X, Wang K, Wang Y, Tu H, Gong G, Zhang H. Medication literacy in Chinese patients with stroke and associated factors: A cross-sectional study. Int J Environ Res Public Health. 2023;20(1):620. DOI: https://doi.org/10.3390/ijerph20010620
Peters MDJ, Godfrey C, McInerney P, Khalil H, Larsen P, Marnie C et al. Best practice guidance and reporting items for the development of scoping review protocols. JBI Evid Synth [Internet]. 2022;20(4):953-68. DOI: https://doi.org/10.11124/JBIES-21-00242
Munn Z, Aromataris E, Tufanaru C, Stern C, Porritt K, Farrow J et al. The development of software to support multiple systematic review types: The Joanna Briggs Institute System for the Unified Management, Assessment and Review of Information (JBI Sumari). JBI Evid Implement [Internet]. 2019;17(1):36-46. DOI: https://doi.org/10.1097/XEB.0000000000000152
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D et al. PRISMA Extension for Scoping Reviews (Prisma-ScR): Checklist and explanation. Ann Intern Med [Internet]. 2018;169(7):467-73. DOI: https://doi.org/10.7326/M18-0850
Bernadette Mazurek Melnyk B, Fineout-Overholt E, Gallagher- Ford L, Stillwell SB. Sustaining evidence-based practice through organizational policies and an innovative model [Internet]. 2011;111(9):57-60. DOI: https://doi.org/10.1097/01.NAJ.0000405063.97774.0e
Abelsson T, Morténius H, Bergman S, Karlsson AK. Quality and availability of information in primary healthcare: The patient perspective. Scand J Prim Health Care [Internet]. 2020;38(1):33- 41. DOI: https://doi.org/10.1080/02813432.2020.1718311
Aboumatar HJ, Carson KA, Beach MC, Roter DL, Cooper LA. The impact of health literacy on desire for participation in healthcare, medical visit communication, and patient reported outcomes among patients with hypertension. J Gen Intern Med. 2013;28(11):1469-76. DOI: https://doi.org/10.1007/s11606-013-2466-5
Altin SV, Stock S. The impact of health literacy, patient-centered communication and shared decision-making on patients’ satisfaction with care received in German primary care practices. BMC Health Serv Res. 2016;16(1):450. DOI: https://doi.org/10.1186/s12913-016-1693-y
Aoki T, Inoue M. Association between health literacy and patient experience of primary care attributes: A cross-sectional study in Japan. PLoS One. 2017;12(9):e0184565. DOI: https://doi.org/10.1371/journal.pone.0184565
Badaczewski A, Bauman LJ, Blank AE, Dreyer B, Abrams MA, Stein REK et al. Relationship between teach-back and patient- centered communication in primary care pediatric encounters. Patient Educ Couns. 2017;100(7):1345-52. DOI: https://doi.org/10.1016/j.pec.2017.02.022
Bailey SC, Wolf MS, Lopez A, Russell A, Chen AH, Schillinger D et al. Expanding the universal medication schedule: A patient-centred approach. BMJ Open [Internet]. 2014;4:3699. DOI: https://doi.org/10.1136/bmjopen-2013-003699
Burke NJ, Napoles TM, Banks PJ, Orenstein FS, Luce JA, Joseph G. Survivorship care plan information needs: perspectives of safety-net breast cancer patients. 2016;11(12):e0168383. DOI: https://doi.org/10.1371/journal.pone.0168383
Cabellos-García AC, Martínez-Sabater A, Ángel Díaz-Herrera M, Gea-Caballero V, Castro-Sánchez E. Health literacy of patients on oral anticoagulation treatment-individual and social determinants and effect on health and treatment outcomes. BMC Public Health. 2021;21:1363. DOI: https://doi.org/10.1186/s12889-021-11259-w
Cawthon C, Willens DE, Kripalani S. Implementing routine health literacy assessment in hospital and primary care patient. Joint Commission J Qual Patient Safety. 2014;40(2):68-76. https://doi.org/10.1016/S1553-7250(14)40008-4
Chauhan A, Walton M, Manias E, Walpola RL, Seale H, Latanik M et al. The safety of health care for ethnic minority patients: a systematic review. Int J Equity Health. 2020;19:118. DOI: https://doi.org/10.1186/s12939-020-01223-2
Nga Fu MFMS, Chi Dao M, Luk MBChBW, Choi Hing Lam EdDM, Sau Fan Ho I, Keung Cheung S et al. Cluster-randomized study on the risk assessment and management program for home blood pressure monitoring in an older population with inadequate health literacy. J Clin Hypertens [Internet]. 2020;22(9):1565-76. DOI: https://doi.org/10.1111/jch.13987
Gibson C, Smith D, Morrison AK. Improving health literacy knowledge, behaviors, and confidence with interactive training. Health Lit Res Pract. 2022;6(2):e113-20. DOI: https://doi.org/10.3928/24748307-20220420-01
Gunn CM, Maschke A, Paasche-Orlow MK, Kressin NR, Schonberg MA, Battaglia TA. Engaging women with limited health literacy in mammography decision-making: Perspectives of patients and primary care providers. J Gen Intern Med [Internet]. 2021;36(4):938-83. DOI: https://doi.org/10.1007/s11606-020-06213-2
Ishikawa H, Ikuko Yamaguchi Ba, Nutbeam D, Kato M, Okuhara T, Okada M et al. Improving health literacy in a Japanese community population: A pilot study to develop an educational programme. Health Expectations [Internet]. 2018;21(4):814-21. DOI: https://doi.org/10.1111/hex.12678
Kay M, Wijayanayaka S, Cook H, Hollingworth S. Understanding quality use of medicines in refugee communities in Australian primary care: A qualitative study. British Journal of General Practice [Internet]. 2016 [citado 11 out. 2022];66(647):e397-409. DOI: DOI: https://doi.org/10.3399/bjgp16X685249
Knowles S, Hays Mphil R, Senra H, Bower P, Locock L, Protheroe J et al. (2018). Empowering people to help speak up about safety in primary care: Using codesign to involve patients and professionals in developing new interventions for patients with multimorbidity. Health Expectations. 2018;21(2):539-48. DOI: https://doi.org/10.1111/hex.12648
Litchfield IJ, Bentham LM, Lilford RJ, Greenfield SM. (2014). Test result communication in primary care: Clinical and office staff perspectives. Fam Pract, . 2014;31(5):592-7. DOI: https://doi.org/10.1093/fampra/cmu041
McCune RL, Lee H, Pohl JM. Assessing health literacy in safety net primary care practices. Applied Nursing Research. 2016;29:188-94. DOI: https://doi.org/10.1016/j.apnr.2015.04.004
Nouri SS, Avila-Garcia P, Cemballi AG, Sarkar U, Aguilera A, Lyles CR. Assessing mobile phone digital literacy and engagement in user-centered design in a diverse, safety-net population: Mixed methods study. JMIR Mhealth Uhealth. 2019;7(8):e14250. DOI: https://doi.org/10.2196/14250
Rowlands G, Tabassum B, Campbell P, Harvey S, Vaittinen A, Stobbart L et al. The evidence-based development of an intervention to improve clinical health literacy practice. Int J Environ Res Public Health, 2020;17(5):1513. DOI: https://doi.org/10.3390/ijerph17051513
Seidling HM, Mahler C, Strauß B, Weis A, Stützle M, Krisam J et al. An electronic medication module to improve health literacy in patients with type 2 Diabetes Mellitus: Pilot randomized controlled trial. JMIR Form Res. 2020;4(4):e13746. DOI: https://doi.org/10.2196/13746
Valdovinos C, Perez-Aguilar G, Huerta RG, Barrios C, Gutierrez G, Mendez C, Abhat A, Moreno G, Brown A, Casillas A. Electronic health literacy among linguistically diverse patients in the Los Angeles Country safety net health system. Ethn Dis. 2022;32(1):21-30. DOI: https://doi.org/10.18865/ed.32.1.21
Yin HS, Jay M, Maness L, Zabar S, Kalet A. Health literacy: An educationally sensitive patient outcome. J Gen Intern Med. 2015;30(9):1363-71. DOI: https://doi.org/10.1007/s11606-015-3329-z
Notes
Conflict of interest declaration

