Artículos
Unveiling the Relationship: Sacroiliac Joint Dysfunction as an Overlooked Factor in Lumbar Back Pain*
Revelando la relación entre la disfunción de la articulación sacroilíaca como un factor pasado por alto en el dolor de espalda lumbar
Revelando a relação entre a disfunção da articulação sacroilíaca como um fator negligenciado na dor lombar
Unveiling the Relationship: Sacroiliac Joint Dysfunction as an Overlooked Factor in Lumbar Back Pain*
Revista Med, vol. 32, núm. 1, pp. 75-82, 2024
Universidad Militar Nueva Granada. Facultad de Medicina
Recepção: 11 Março 2024
Aprovação: 14 Abril 2024
Publicado: 29 Junho 2024
Abstract
Introduction: The Sacroiliac joint (SIJ) serves as a crucial connection between the sacrum and ilium, playing a vital role in transferring forces during physical activity. Its biomechanical function is essential for stability, supported by ligaments and pelvic floor muscles. However, SIJ dysfunction can contribute to lower back pain, a condition affecting 70-85 % of Western society.
Causes: SIJ dysfunction can stem from various factors, including abnormal motion or malalignment, triggered by arthritis, trauma, or atypical gait patterns.
Diagnosis: Diagnosis SIJ dysfunction involves physical examinations such as FABER, compression, distraction, thigh thrust, and Gaenslen tests. Typically, three positive provocative test results are required for diagnosis, supplemented by imaging techniques like X-rays, MRIS, and joint injections.
Misdiagnosis: Despite the availability of diagnostic methods, SIJ dysfunction is frequently misdiagnosed due to symptoms overlap with other conditions and overlooked etiology.
Treatment: Upon diagnosis, SIJ dysfunction can be managed with conservative measures like physical therapy and NSAIDS, or more invasive interventions such as surgery.
Conclusion: SIJ dysfunction is a prevalent yet often misdiagnosed condition, emphasizing the importance of raising awareness among both the public and clinicians to ensure accurate diagnosis and appropriate treatment.
Keywords: Sacroiliac Joint Dysfunction+ low-back pain+ SIJD misdiagnosis+ fixation+ SIJD diagnosis.
Resumen
Introducción: La articulación sacroilíaca (SIJ) sirve como una conexión crucial entre el sacro y el Ilion, desempeñando un papel vital en la transferencia de fuerzas durante la actividad física. Su función biomecánica es esencial para la estabilidad, apoyada por ligamentos y músculos del suelo pélvico. Sin embargo, la disfunción de la SIJ puede contribuir al dolor lumbar, una condición que afecta al 70-85 % de la sociedad occidental.
Causas: La disfunción de la SIJ puede derivar de varios factores, incluyendo movimiento anormal o desalineación, a menudo desencadenados por artritis, trauma o patrones de marcha atípicos.
Diagnóstico: El diagnóstico de la disfunción de la SIJ implica exámenes físicos como las pruebas FABER, de compresión, distracción, empuje del muslo y Gaenslen. Típicamente, se requieren tres resultados positivos de pruebas provocativas para el diagnóstico, complementados por técnicas de imagen como radiografías, resonancias magnéticas y inyecciones articulares.
Diagnóstico erróneo: A pesar de la disponibilidad de métodos diagnósticos, la disfunción de la SIJ es frecuentemente mal diagnosticada debido a la superposición de síntomas con otras condiciones y la etiología pasada por alto.
Tratamiento: Tras el diagnóstico, la disfunción de la SIJ puede ser tratada mediante medidas conservadoras como la fisioterapia y los AINES, o intervenciones más invasivas como procedimientos quirúrgicos.
Conclusión: La disfunción de la SIJ es una condición prevalente pero frecuentemente mal diagnosticada, destacando la importancia de aumentar la conciencia tanto entre el público como entre los clínicos para garantizar un diagnóstico preciso y un tratamiento adecuado.
Palabras clave: Disfunción de la articulación sacroilíaca, dolor lumbar, diagnóstico erróneo, fijación, diagnóstico.
Resumo
Introdução: A articulação sacro-ilíaca (SIJ) serve como uma conexão crucial entre o sacro e o ilíaco, desempenhando um papel crucial na transferência de forças durante a atividade física. Sua função biomecânica é essencial para a estabilidade, apoiada por ligamentos e músculos do assoalho pélvico. No entanto, a disfunção da SIJ pode contribuir para a dor lombar, uma condição que afeta 70-85 % da sociedade ocidental.
Causas: A disfunção da SIJ pode derivar de vários fatores, incluindo movimento anormal ou desalinhamento, muitas vezes desencadeados por artrite, trauma ou padrões de marcha atípicos.
Diagnóstico: O diagnóstico da disfunção da SIJ implica exames físicos como os testes FABER, de compressão, distração, empurrão do fêmur e Gaenslen. Tipicamente, são necessários três resultados positivos de testes provocativos para o diagnóstico, complementados por técnicas de imagem como radiografias, ressonâncias magnéticas e injeções articulares.
Diagnóstico errôneo: Apesar da disponibilidade de métodos diagnósticos, a disfunção da SIJ é frequentemente mal diagnosticada devido à sobreposição de sintomas com outras condições e a etiologia negligenciada.
Tratamento: Após o diagnóstico, a disfunção da SIJ pode ser tratada por meio de medidas conservadoras como fisioterapia e AINES, ou intervenções mais invasivas como procedimentos cirúrgicos.
Conclusão: A disfunção da SIJ é uma condição prevalente, mas frequentemente mal diagnosticada, destacando a importância de aumentar a conscientização tanto entre o público quanto entre os clínicos para garantir um diagnóstico preciso e um tratamento adequado.
Palavras-chave: Disfunção da articulação sacro-ilíaca, dor lombar, diagnóstico errôneo, fixação, diagnóstico.
Introduction
The Sacroiliac Joints (SIJ) are auricular-shaped and lie between the sacrum and ilium, constituting the largest axial joint in the pelvis and facilitating the articulation iliac bones to the sacrum 1,2. Their anatomy allows for the exchange of load located in the lumber spine and lower limbs. The SIJ is around 1-2 mm in width, and each joint on either side of the sacrum is bound by a fibrous capsule. The iliac aspect of the sacroiliac joint (SIJ) has cartilage that is thinner than the sacral aspect, thicker cortical bone, and denser cacellous bone. Numerous ligaments and pelvic floor muscles, such as the levator ani and coccygeus muscles, support the SIJ Due to its anatomical and biophysical properties, the SIJ is crucial in preserving the mechanical stability of the human body. The joint's main biomechanical function is to transfer forces from the legs to the body. This function is crucial, especially during bipedal walking 2,3Numerous ligaments and pelvic floor muscles, such as the levator ani and coccygeus muscles, support the SIJ. These elements aid in the transmission of shear forces by supporting the joint limiting its range of motion, and maintaining its stability of the joint1. Women have more flexibility in their SIJ ligaments and have a center of gravity that is more forward on the body. In contrast, the male pelvis is wider than the female pelvis, particularly in the distance between the iliac crests 2,3
The result of this load transmission is significant mechanical stress on the SIJ 2. The mechanism of injury SIJ can be addressed as a mixture of axial loading and sudden rotation. Many alterations in the structure of SI joints can create a sensation of pain. These alterations include: small or large fractures, cartilage softening, soft tissue destruction, inflammation, disruption of the capsule or synovium, stress in the capsule and ligaments, restricted or excessive joint mobility, external compression, or shearing forces, and irregular joint function 4.
According to estimates, between 70% and 85 % of people in Western societies will suffer from lower back pain at some point in their lives1. SIJ dysfunction is thought to be the root cause of lower back pain in up to 30 % of cases 3. The epidemiology of SIJ dysfunction is not well-known, but it is known that this pathology is common worldwide and disabling. According to Sembrano and Polly, 65 % of patients with Low Back Pain (LBP) had spine-only pathology, followed by 14.5 % of patients with SIJ dysfunction, 12.5 % with hip pathology, and the remaining 10 % with pain of unknown etiology2. SIJ pain is often seen in young people who play sports and receive trauma or injuries. Additionally, elderly people can experience SIJ pain if they have degenerative joint disease, and pregnant women also complain of SIJ discomfort. Since women have heightened SIJ joint flexibility, more stress is placed on their mobility and the load on surrounding tissues, making them more prone to experiencing SIJ dysfunction 5.
Causes
SIJ dysfunction typically results from abnormal motion, including hyper or hypomobile Sacroiliac joints and malalignment 2,6. This condition may develop due to various factors, such as limb length inequality (LLD), high-velocity trauma, previous lumbar fusion surgeries, injuries, degenerative arthritis, moderate impact exercise, overexertion, inflammatory bowel disease, spondyloarthropathies like ankylosing spondylitis, joint infections, abnormal gait patterns, and scoliosis2,7. Dysfunction can also occur during atypical lifting, forward bending, or assuming a lordotic posture, causing a misalignment of the body's center relative to the acetabular center. Dysfunction is likely to arise if the abdominal muscles cannot adequately support rotation and force transmission 2. Despite the underlying cause, the relationship between pain and SIJ dysfunction remains consistent 7.
Diagnosis
Specific physical examination tests, including the FABER, compression, distraction, thigh thrust, and Gaenslen tests, are used to diagnose SIJ dysfunction. A diagnosis of SIJ pain is typically made when three out of the five provocative tests return positive results, with at least one of these being the compression or thigh thrust test. However, a recent study, to diagnose SIJD in patients, this study compared motion palpation and pain provocation tests to the gold-standard sacroiliac joint block procedure 8.
The FABER test involves positioning the hip and knee, with a positive result indicated by pain on the side of the flexed knee. In the FABER test, also known as Patrick's test, the patient lies supine. One knee is flexed at a 90-degree angle, while the opposite knee is laid flat on the examination table. The examiner presses the contralateral Anterior Superior Iliac Spine (ASIS) against the table, and then pushes the bent knee down towards the table 8.
In the Gaenslen test, a posterior force is applied to the caudal knee, while the pelvis is mobilized by a superior or posterior force directed towards the cephalad knee.
In the Thigh Thrust Test, force is directed through the axis of the femur with the cephalad hand, creating a shear force. This is done simultaneously with the sacrum being stabilized against the table with the caudal hand.
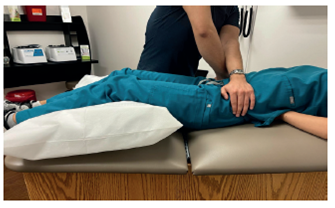
Figure 1
Distraction Test
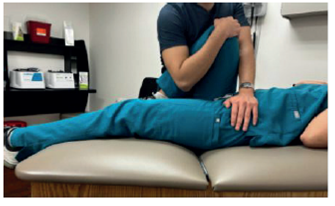
Figure 2
Thigh Thrust Test
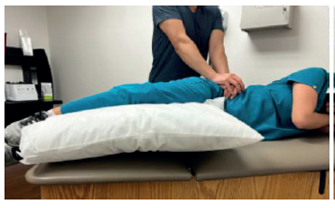
Figure 3
Compression Test
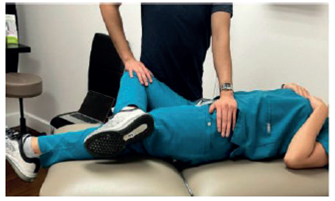
Figure 4
FABER Test
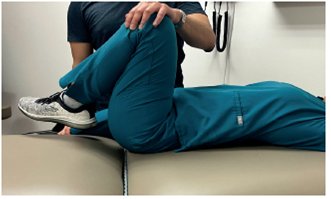
Figure 5.1
Gaenslen Test. Lateral View
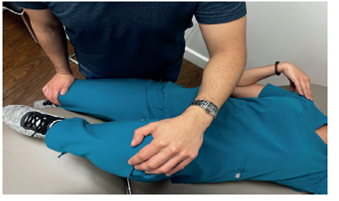
Figure 5.2
Gaenslen Test. Superior View
In the Distraction test, a posteriorly directed force is applied to the anterior superior iliac spine, distracting the sacroiliac joints.
In the Compression test, similar to the Distraction test, a posteriorly directed force is applied to the iliac crest, compressing the sacroiliac joint 9.
If performed correctly, one of the highest sensitivities among the five tests can come from the FABER test 10.
During the Thigh Thrust Test, compression of the SIJ resulting in pain indicates a successful result. A positive outcome of the Gaenslen test causes pain in the lower back, stressing both SIJ. Compression of the SIJ during the Compression Test, with resulting pain, indicates a successful result. The Distraction Test distinguishes between ASIS and SIJ pain based on a positive outcome.
Based on responses to pain, these tests assist in diagnosis SIJ dysfunction8. Diagnostic imaging such as magnetic resonance imaging (MRIS) and X-rays are also employed to achieve accurate diagnoses of SIJ. The diagnostic gold standard has shifted towards using intra-articular SIJ blocks, as there is no conclusive evidence that any specific provocative test or imaging technique definitively indicates SIJ pain. These involve the injection of local anesthetics as a diagnostic tool, sometimes supplemented with steroids1.
Misdiagnosis
Despite the various methods available for diagnosing SIJ dysfunction, it remains commonly misdiagnosed due to symptom similarities with other conditions such as intervertebral discs and facet joints11. Furthermore, since SIJ pain may coincide with non-neurological symptoms like dyspareunia and bladder dysfunction, it can be mistaken for issues unrelated to its underlying cause and attributed to other areas12.
In a study by Song et al., a 33-year-old woman initially diagnosed with Ankylosing Spondylitis (AS) experienced chronic buttock pain and sacroiliitis progression, (detected using plain X-ray and an MRI). Treatment with nonsteroidal anti-inflammatory drugs (NSAIDS), for AS proved ineffective. Subsequent pelvic bone computed tomography (CT) revealed an Accessory Sacroiliac Joint (ASIJ) with degenerative alterations, sclerosis, and osteophytes in the right SI joint13.
In another study, Prassopoulos et al. utilized CT scans to analyze SIJ anatomical variations, identifying ASIJ as the most prevalent variant at 19 %14. Despite its prevalence, the clinical significance of ASIJ often overlooked, particularly because most cases are asymptomatic and incidentally diagnosed13.
For example, Demir et al., discovered ASIJ to be the most prevalent SIJ variant in their study, with 17.5 % of patients exhibiting it on a CT scan. Notably, many of these patients were asymptomatic for lower back pain15. Nevertheless, this absence of symptoms does not preclude the possibility of symptomatic presentation. ASIJ frequently manifest as chronic buttock pain and/or lower back pain, particularly among patients with severe arthritis and degenerative alterations.
In a study evaluating lower back pain in individuals under 40 years old using CT scans, ASIJ was identified as a source of pain in 4.5 % of cases. Additionally, 31 % showed abnormal SIJ examinations, 10.2 % were suspected to have sacroiliitis, and 3.3 % had confirmed sacroiliitis among 484 lumbar spine CT analysis 16.
Clinicians must maintain awareness of symptoms associated with SIJ dysfunction, and its specific variants. This awareness can aid in preventing misdiagnosis and ensuring appropriate treatment 10.
Treatments
The treatment options for SIJ dysfunction range from conservative management to surgical approaches. Conservative management includes physical therapy, oral painkillers like NSAIDS, medical therapy, and chiropractic care. Patients should receive education on lifestyle modifications and proper weightlifting, and outpatient physical therapy should be pursued after acute management 2. If pelvic instability is identified as part of the SIJ pain etiology a sacroiliac belt may be used for a short period as additional support 2,17.
If conservative measures fail within 6 weeks, further interventions such as injections (intraarticular or periarticular), nerve blocks, and radiofrequency procedures may be considered2. A diagosis SIJ joint injections serve both diagnostic and therapeutic purposes. A diagnostic SIJ block may be considered if a patient responds favorably to three or more of these tests, indicating a likelihood of SIJ problems. An anesthetic is injected into the SI joint during diagnostic blocks. Confirmation of SIJ dysfunction occurs if the patient experiences at least a 75 % reduction in pain while performing previously painful movements during the anesthetic 18.
Initial treatments for pain managing typically involve a combination of methods like pain control and physical therapy. However, there is a growing body of evidence supporting the use of minimally invasive procedures. These procedures can complement conservative approaches or secondary options for patients who do not respond to initial treatments.
In a study, it was found that after 12 months, pain scores improved by 2.7 points in the group using traditional open treatments and by 6.2 points in the group using minimally invasive procedures. For the 2-year assessment (available for 96 patients), there was an improvement of 2 points in the open treatment group and 5.6 points in the minimally invasive treatment group. Therefore, minimally invasive treatment options have also been considered effective in treating SIJ pain 19. They have also been shown to be more effective than conservative treatment.
Results comparing conservative vs. surgical procedures were examined in a study by Dengler et al. Fifty-one patients received conservative treatment, consisting of six months of physical therapy. Two participants received additional sacroiliac corticosteroid injections, and one received injections along with radiofrequency ablation. Fifty-two patients underwent minimally invasive sacroiliac arthrodesis with triangular titanium implants. When the results were analyzed, there was a significant improvement in lower back pain in the group that received invasive therapy at 6 and 24 months after treatment 20.
Conclusion
SIJ dysfunction is a condition with increasing prevalence, often leading to misdiagnosis despite available diagnostic methods. Raising awareness of SIJ dysfunction among medical professionals and the public is crucial to ensure correct diagnosis and proper treatment. As research continues to elucidate SIJ dysfunction's etiology and methods for preventing misdiagnosis, comprehensive reviews become essential for refining clinical practices and enhancing patient health. By deepening understanding and improving diagnostic reliability and accuracy, efforts focused on SIJ dysfunction pave the way for refined neurological care and treatment effectiveness. Overall, these efforts benefit patients by ensuring that appropriate care is tailored to their specific condition.
References
Buchanan, P., Vodapally, S., Lee, D. W., Hagedorn, J. M., Bovinet, C., Strand, N., Sayed, D., and Deer, T. (2021). Successful Diagnosis of Sacroiliac Joint Dysfunction. Journal of pain research, 14, 3135-3143. https://doi.org/10.2147/JPR.S327351
Gartenberg, A., Nessim, A., and Cho, W. (2021). Sacroiliac joint dysfunction: pathophysiology, diagnosis, and treatment. European Spine Journal, 30(10), 2936-2943. https://doi.org/10.1007/s00586-021-06927-9
Abdollahi, S., Sheikhhoseini, R., Rahimi, M., and Huddleston, W. E. (2023). The sacroiliac dysfunction and pain are associated with history of lower extremity sport related injuries. BMC sports science, medicine and rehabilitation, 15(1), 36. https://doi.org/10.1186/s13102-023-00648-w
Capobianco R, Cher D, SIFI Study Group (2015) Safety and effectiveness of minimally invasive sacroiliac joint fusion in women with persistent post-partum posterior pelvic girdle pain: 12-month outcomes from a prospective, multi-center trial. Springerplus. 4:570. https://doi.org/10.1186/s40064-015-1359-y
Kiapour, A., Joukar, A., Elgafy, H., Erbulut, D. U., Agarwal, A. K., and Goel, V. K. (2020). Biomechanics of the Sacroiliac Joint: Anatomy, Function, Biomechanics, Sexual Dimorphism, and Causes of Pain. International journal of spine surgery, 14(Suppl 1), 3-13. https://doi.org/10.14444/6077
Nejati, P., Sartaj, E., Imani, F., Moeineddin, R., Nejati, L., and Safavi, M. (2020, March). Accuracy of the diagnostic tests of sacroiliac joint dysfunction. Journal of chiropractic medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7646135/https://doi.org/10.1016/j.jcm.2019.12.002
Telli, H., Telli, S., and Topal, M. (2018). The Validity and Reliability of Provocation Tests in the Diagnosis of Sacroiliac Joint Dysfunction. Pain physician, 21(4), E367-E376. https://doi.org/10.36076/ppj.2018.4.E367
Barros, G., McGrath, L., and Gelfenbeyn, M. (2019). Sacroiliac Joint Dysfunction in Patients with Low Back Pain. Federal practitioner: for the health care professionals of the VA, DoD, and PHS, 36(8), 370-375.
Cusi M. F. (2010). Paradigm for assessment and treatment of SIJ mechanical dysfunction. Journal of bodywork and movement therapies, 14(2), 152-161. https://doi.org/10.1016/j.jbmt.2009.12.004
Song, R., Lee, S., and Lee, S. H. (2019). Progressive sacroiliitis due to accessory sacroiliac joint mimicking ankylosing spondylitis: A case report. Medicine, 98(16), e15324. https://doi.org/10.1097/MD.0000000000015324
Prassopoulos, P. K., Faflia, C. P., Voloudaki, A. E., and Gourtsoyiannis, N. C. (1999). Sacroiliac joints: anatomical variants on CT. Journal of computer assisted tomography, 23(2), 323-327. https://doi.org/10.1097/00004728-199903000-00029
Demir, M., Mavi, A., Gümüsburun, E., Bayram, M., Gürsoy, S., and Nishio, H. (2007). Anatomical variations with joint space measurements on CT. The Kobe journal of medical sciences, 53(5), 209-217.
Klang, E., Lidar, M., Lidar, Z., Aharoni, D., and Eshed, I. (2017). Prevalence and awareness of sacroiliac joint alterations on lumbar spine CT in low back pain patients younger than 40 years. Acta radiologica (Stockholm, Sweden: 1987), 58(4), 449-455. https://doi.org/10.1177/0284185116656490
Raj MA, Ampat G, Varacallo M (2020) Sacroiliac Joint Pain. StatPearls Publishing
Wu, L., Tafti, D., and Varacallo, M. (2023, September 4). Sacroiliac joint injection - statpearls - NCBI bookshelf. Sacroiliac Joint Injection. https://www.ncbi.nlm.nih.gov/books/NBK513245/
Aranke, M., McCrudy, G., Rooney, K., Patel, K., Lee, C. A., Hasoon, J., Urits, I., Viswanath, O., and Kaye, A. D. (2022). Minimally Invasive and Conservative Interventions for the Treatment of Sacroiliac Joint Pain: A Review of Recent Literature. Orthopedic reviews, 14(3), 31915. https://doi.org/10.52965/001c.31915
Notas
