ABSTRACT:
Microvasculature failure is expected in sepsis and at higher amine
concentrations. Therefore, special attention focused individually on
microcirculation is needed. Here, we present that methylene blue can prevent
leukocytes from adhering to the endothelium in a rat model of
lipopolysaccharide-induced endotoxemia. As hypothesis evidence, an intravital
microscopy image is presented.
Keywords: Methylene Blue, Microcirculation, Microvessels, Endothelium, Lipopolysaccharides.
Carátula del artículo
Intravital Microscopy Evidence That Methylene Blue Should Be a
Vasopressor-Sparing Agent in Sepsis Vasoplegia
Fabiola Leslie Antunes Cardoso Mestriner
Universidade de São Paulo, Brazil
Pedro Brüch Dantas
Universidade de São Paulo, Brazil
Jéssyca Michelon Barbosa
Universidade de São Paulo, Brazil
 Paulo Roberto B. Evora prbevora@fmrp.usp.br
Paulo Roberto B. Evora prbevora@fmrp.usp.br
Universidade de São Paulo, Brazil
Christiane Becari
Universidade de São Paulo, Brazil
Universidade de São Paulo, Brazil
Brazilian Journal of Cardiovascular Surgery, vol. 39, no. 3, e20230066, 2024
Sociedade Brasileira de Cirurgia Cardiovascular
Received: 18 February 2023
Accepted: 04 September 2023
Funding
Funding source: CAPES
Contract number: 2017/21539-7
Contract number: 2018/23718-8
Funding
Funding source: FAPESP
Contract number: 2019/21721-4
Funding statement: Financial support: This study was funded by the
CAPES (Christiane Becari 2017/21539-7, 2018/23718-8); Fundação de Amparo à
Pesquisa do Estado de São Paulo (FAPESP) (M. Barbosa 2019/21721-4); Conselho
Nacional de Desenvolvimento Científico e Tecnológico, Faculdade de Medicina de
Ribeirão Preto, Universidade de São Paulo.
INTRODUCTION
Gomes[1] first described vasoplegic
syndrome in heart surgery patients have been undergoing treatment with methylene
blue (MB) for it. Evora et al (1996)[2] were the ones who suggested the use of MB for treatment. In
1996, Andrade et al.[3] first
documented this therapeutic approach in heart surgery patients. MB successfully
treats vasopressor-refractory septic shock vasoplegia by inhibiting endothelial
nitric oxide and improving responsiveness to amines. However, only one relevant
study has explored the microcirculatory effects of MB[4].
Intravital Microscopy Method
This study involved adult male Hannover rats under controlled conditions approved
by the Committee on Ethics in Animal Experimentation of the Faculdade de
Medicina de Ribeirão Preto, Universidade de São Paulo (2/2015). We anesthetized
the animals, exteriorized the mesentery, and examined postcapillary venules with
diameters of 10-18 micrometers. We evaluated leukocytes adhering to the
endothelium within 10-micrometer venule lengths. Furthermore, we considered
leukocytes adhered for up to 30 seconds for the microcirculatory protective
effect (Figures 1 and 2).
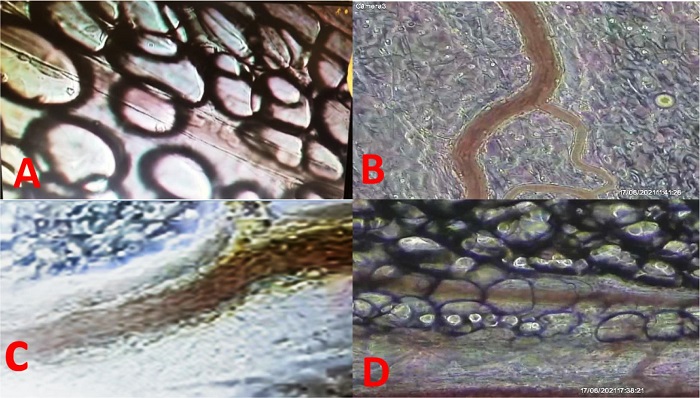 Fig. 1
Methylene blue (MB) inhibiting neutrophil leukocyte
rolling/adhesion after lipopolysaccharide (LPS) intravenous dose.
(A) Postcapillary venules of saline group (saline at zero and 15
min); (B) postcapillary venules of LPS group (LPS at zero and saline
at 15 min); (C) postcapillary venules of only MB (MB at zero and
saline at 15 min); (D) postcapillary venules of MB after LPS doses
(LPS at zero and MB at 15 min). # Intra peritoneal image of
postcapillary venules. (A) Control (roller mean = 52.4, adhesion
mean = 1.3); (B) LPS + salina (roller mean = 816, adhesion mean =
9.4); (C) LPS + MB (roller mean = 28.1, adhesion mean = 3.2); (D) MB
+ LPS (roller mean = 76.4, adhesion mean = .6).
Fig. 1
Methylene blue (MB) inhibiting neutrophil leukocyte
rolling/adhesion after lipopolysaccharide (LPS) intravenous dose.
(A) Postcapillary venules of saline group (saline at zero and 15
min); (B) postcapillary venules of LPS group (LPS at zero and saline
at 15 min); (C) postcapillary venules of only MB (MB at zero and
saline at 15 min); (D) postcapillary venules of MB after LPS doses
(LPS at zero and MB at 15 min). # Intra peritoneal image of
postcapillary venules. (A) Control (roller mean = 52.4, adhesion
mean = 1.3); (B) LPS + salina (roller mean = 816, adhesion mean =
9.4); (C) LPS + MB (roller mean = 28.1, adhesion mean = 3.2); (D) MB
+ LPS (roller mean = 76.4, adhesion mean = .6).
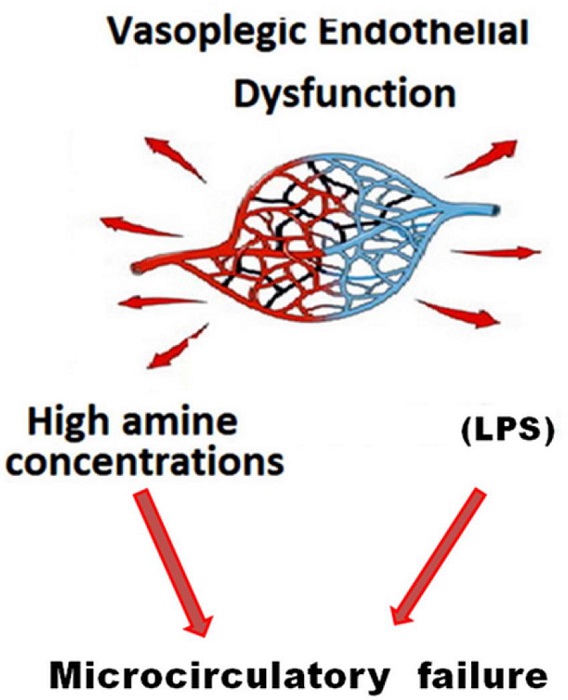 Fig. 2
Schematic representation of microcirculatory damage consequent to
lipopolysaccharide (LPS) and high doses of amine.
Fig. 2
Schematic representation of microcirculatory damage consequent to
lipopolysaccharide (LPS) and high doses of amine.
The technique is particularly useful for studying microcirculation. It allows
researchers to observe blood flow through capillaries and venules, providing
insights into blood perfusion, oxygen exchange, and interactions between blood
cells and vessel walls.
COMMENTS
We state that the medical literature underestimates the importance of cyclic
guanosine monophosphate. Combining three concepts could yield better results against
high mortality rates in critically ill patients: (1) using “broad-spectrum
vasopressors”, (2) employing vasopressor-sparing strategies, and (3) protecting
microcirculation.
MB should serve as a vasopressor-sparing agent. We need progressively minor
concentrations of amines to maintain blood pressure (around 65 mmHg). Additionally,
using high amine concentrations independently of blood pressure becomes reasonable.
We anticipate the disclosure, hoping that new research groups interested in the
subject will emerge. Therefore, we firmly believe that the briefly discussed
concepts will incorporate as paradigms in vasodilatory shock treatment.
“Microcirculatory protection” is an old concept. It assumes that microvasculature
failure is unavoidable even with arterial pressure under control, with increasing
amine concentrations. Therefore, special attention focused individually on
microcirculation is needed. The image presented, corresponding to the record of an
experiment, has been checked and reproduced in our laboratory. With the hope of
motivating different research groups, we decided the hypothesis disclosure. Chances
are that the briefly discussed hypothetical concepts can be incorporated as
paradigms in treating vasodilatory shock[5-7].
REFERENCES
Gomes WJ, Carvalho AC, Palma JH, Gonçalves I Jr, Buffolo E.
Vasoplegic syndrome: a new dilemma. J Thorac Cardiovasc Surg.
1994;107(3):942-3.
Evora PR, Ribeiro PJ, de Andrade JC. Methylene blue administration
in SIRS after cardiac operations. Ann Thorac Surg. 1997;63(4):1212-3. doi:
10.1016/s0003-4975(97)00198-7.
Andrade JCS, Batista Filho ML, Evora PRB, et al. Methylene blue
administration in the treatment of the vasoplegic syndrome after cardiac
surgery. Rev Bras Cir Cardiovasc. 1996;11:107-14.
Nantais J, Dumbarton TC, Farah N, Maxan A, Zhou J, Minor S, Lehmann
C. Impact of methylene blue in addition to norepinephrine on the intestinal
microcirculation in experimental septic shock. Clin Hemorheol Microcirc.
2014;58(1):97-105. doi: 10.3233/CH-141874.
Evora PRB, Braile DM. "Vasopressor Support Sparing
Strategies": a Concept to be Incorporated as a Paradigm in the Treatment of
Vasodilatory Shock. Braz J Cardiovasc Surg. 2019;34(1):I-II. doi:
10.21470/1678-9741-2019-0600.
Buckley MS, Barletta JF, Smithburger PL, Radosevich JJ, Kane-Gill
SL. Catecholamine Vasopressor Support Sparing Strategies in Vasodilatory Shock.
Pharmacotherapy. 2019;39(3):382-398. doi: 10.1002/phar.2199.
Evora PRB, Soares ROS, Bassetto S, Auxiliadora-Martins M, Silva
FLDS, Basile A Filho. After Thirty Years, We Still Cannot Understand Why
Methylene Blue is not a Reference to Treat Vasoplegic Syndrome in Cardiac
Surgery. Braz J Cardiovasc Surg. 2021;36(3):406-11. doi:
10.21470/1678-9741-2021-0955. Erratum in: Braz J Cardiovasc Surg. 2022 Mar
10;37(1):144.
Notes
Notes
Financial support: This study was funded by the CAPES (Christiane
Becari 2017/21539-7, 2018/23718-8); Fundação de Amparo à Pesquisa do Estado de
São Paulo (FAPESP) (M. Barbosa 2019/21721-4); Conselho Nacional de
Desenvolvimento Científico e Tecnológico, Faculdade de Medicina de Ribeirão
Preto, Universidade de São Paulo.
Conflict of interest declaration
No conflict of interest.
Author notes
This study was carried out at the Department of Surgery and Anatomy,
Faculdade de Medicina de Ribeirão Preto, Universidade de São Paulo, Ribeirão
Preto, São Paulo, Brazil.
Correspondence Address: Paulo Roberto B.
Evorahttps://orcid.org/0000-0001-9631-946X Bandeirantes Av., 3900,
Ribeirão Preto, SP, Brazil, Zip Code: 14049-900, E-mail:
prbevora@fmrp.usp.br







